Key Takeaways
- Neighborhoods Served: Accessible care for residents in Alamo Heights, Stone Oak, Southtown, the Medical Center district, and Downtown San Antonio.
- Local Insight: In Bexar County, a significant portion of individuals seeking support also manage co-occurring mental health conditions, making integrated dual diagnosis care essential.
- Landmarks: Facilities and telehealth networks are designed to be convenient to major hubs like The Pearl and the San Antonio River Walk.
- Accessibility: Programs are easily reachable via major transit routes including I-35, Loop 410, and US-281, with flexible telehealth options to bypass traffic.
Understanding Relapse Prevention Programs San Antonio
If you are navigating recovery near the River Walk or commuting along Loop 410, you know that healing is a journey with its own unique rhythm. Finding the right relapse prevention programs San Antonio is a vital step for you or your loved one. In Bexar County, local data shows that many individuals seeking support are also balancing co-occurring mental health conditions, making compassionate, integrated care more important than ever. Ripple Ranch Recovery, located on a serene 20+ acre property in nearby Spring Branch, offers a sanctuary away from the city’s hustle, while our partner, Continuum Outpatient Center, provides accessible ongoing care right in the heart of the metro area.
Why Relapse Occurs as a Process
A return to use does not happen in a single moment—it unfolds as a process unique to each individual’s journey. For many in San Antonio, this process is shaped by a complex blend of emotional, mental, and environmental factors, rather than a lack of willpower or motivation. Research shows that 40 to 60 percent of people in recovery will experience a setback at some point, highlighting that it is a common and expected part of the chronic disease model.2

“A lapse is not a failure of character, but a signal that your recovery strategy needs a compassionate adjustment.”
The process often begins long before substance use resumes. Emotional upheaval, isolation, and mounting stress—especially in a city as vibrant and high-pressure as San Antonio—can all contribute to early warning signs. These signals may be subtle, such as withdrawing from support networks or neglecting self-care, and can build over time. Without acknowledging these indicators, the risk of progressing from a lapse to a full return to use increases.
Consider the story of Marcus, a resident of Southtown. He found that the stress of downtown traffic and demanding work hours slowly eroded his coping mechanisms. By engaging with relapse prevention programs San Antonio, he learned to recognize his early emotional triggers. Normalizing these setbacks as part of the ongoing recovery process allows individuals and families to respond with proactive support rather than shame.10
Recognizing Emotional and Mental Warning Signs
Recognizing emotional and mental warning signs is essential for anyone aiming to sustain recovery in San Antonio. These early signals often appear before any external behaviors change. Many people notice increased anxiety, restlessness, or a sense of isolation, especially when navigating life in bustling neighborhoods like Alamo Heights or the Medical Center, where social pressures and triggers may be more pronounced.
To help you or your loved one stay vigilant, watch for these common internal warning signs:
- Persistent irritability or unexplained sadness.
- Feeling overwhelmed by daily stress or traffic along I-35.
- Obsessive thinking about past substance use or romanticizing previous experiences.
- Doubting one’s ability to stay on the path of wellness.
- Difficulty concentrating and engaging in negative self-talk.
Research shows that identifying and addressing these internal signals early can dramatically reduce the risk of progressing from a lapse to a full return to use.3 Relapse prevention programs San Antonio often teach practical skills for monitoring mood and thought patterns, helping individuals intervene proactively. Open conversations with trusted peers, journaling, and using local resources—like support groups in Stone Oak or counseling near The Pearl—can be life-changing steps.
Evidence-Based Tools for Relapse Prevention Programs San Antonio
Cognitive and Behavioral Therapy Approaches
Cognitive and behavioral therapy approaches are at the foundation of most effective relapse prevention programs San Antonio. These therapies are designed to help individuals identify high-risk situations, challenge unhelpful thought patterns, and develop healthier coping mechanisms. Cognitive-Behavioral Therapy (CBT), for example, has been shown to significantly reduce return-to-use rates by teaching practical skills such as managing cravings, problem-solving, and restructuring negative thinking.6
| Therapy Type | Primary Focus | Benefit for Co-Occurring Conditions |
|---|---|---|
| Cognitive-Behavioral Therapy (CBT) | Restructuring negative thought patterns | Helps manage anxiety and depressive symptoms alongside cravings. |
| Dialectical Behavior Therapy (DBT) | Emotional regulation and distress tolerance | Empowers individuals to respond thoughtfully rather than react impulsively. |
| EMDR Therapy | Processing underlying trauma | Addresses root causes of PTSD that often fuel substance use. |
Mindfulness-based strategies are gaining traction in San Antonio as well. This approach combines traditional cognitive strategies with mindfulness practices, helping people observe cravings and difficult emotions without judgment or immediate action.2 Local programs, including Continuum Outpatient Center, integrate these therapies into group and individual sessions, tailoring strategies to the unique needs of neighborhoods like Monte Vista, Olmos Park, and King William.
Medication-Assisted Treatment Options
Medication-assisted treatment (MAT) is an essential element of many relapse prevention programs San Antonio, especially for those managing opioid, alcohol, or prescription drug use disorders. MAT combines FDA-approved medications with therapy and counseling, helping to restore brain chemistry, relieve intense cravings, and reduce the risk of return to problematic use. This approach is not about substituting one substance for another, but about supporting individuals through the vulnerable early stages of recovery and beyond.1
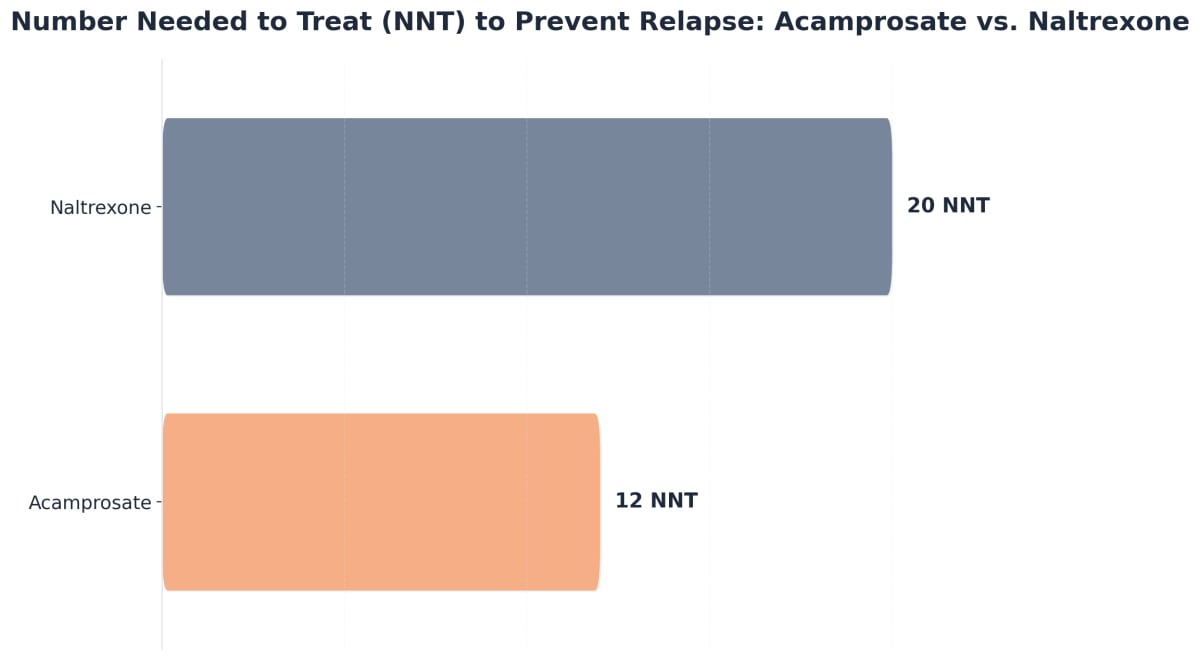
In San Antonio, common medications are used to treat dependence while supporting overall wellness. Research indicates that these medications can significantly lower return-to-use rates and improve treatment retention when integrated into a holistic care plan.2
Understanding the Impact of MAT
While medication provides physiological stability, ongoing support from counseling and community resources remains critical. No single medication is a cure, and success depends on addressing co-occurring mental health needs, social stressors, and local challenges unique to San Antonio neighborhoods. When combined with therapy and personalized care, MAT is a powerful tool for long-term wellness.1
Integrated Care for Co-Occurring Conditions
Living with both a substance use disorder and a mental health condition creates unique challenges that require specialized dual diagnosis treatment. When depression, anxiety, PTSD, or bipolar disorder coexist with substance use, addressing only one condition leaves the door open for setbacks. Integrated dual diagnosis treatment recognizes that these conditions fuel each other—untreated anxiety may drive alcohol use, while substance use intensifies depressive episodes or triggers mood instability. Breaking this cycle requires treating both conditions simultaneously within a coordinated plan.
The reality of co-occurring conditions means that a lapse happens, and it’s not a failure—it’s often part of the recovery process. What matters is having the right tools to prevent a full return to use and the support to respond effectively when warning signs appear. Effective relapse prevention programs San Antonio provide these tools by addressing the interconnected nature of mental health and substance use. Without this integrated approach, individuals often find themselves caught in a pattern where progress in one area gets undermined by the untreated condition.
To help manage these interconnected symptoms, many individuals utilize digital health tools alongside their therapy. For instance, when logging into a secure patient portal, you might use a keyboard shortcut like Ctrl + P to print your weekly coping strategies, or you might see a system confirmation such as sync_complete: true when your daily mood log updates. A typical digital check-in might look like this:
Daily Wellness Log: 1. Anxiety Level (1-10): 2. Trigger Encountered (Yes/No): 3. Coping Skill Applied: Deep Breathing / Reaching Out
The strength of dual diagnosis treatment lies in its coordinated approach. Psychiatrists, therapists, addiction counselors, and medical professionals work together, ensuring that every intervention considers both mental health stability and recovery goals. At Ripple Ranch Recovery, this integrated model extends throughout the continuum of care—from medically supervised detox through residential treatment on our peaceful Spring Branch campus, and into ongoing support.
Beyond clinical interventions, effective dual diagnosis treatment incorporates holistic elements that support overall wellness. Nutrition therapy addresses the physical impact of both conditions on the body. Mindfulness and yoga therapy provide practical tools for managing stress and building resilience in daily life. Long-term recovery requires ongoing support beyond initial treatment. Through the partnership between Ripple Ranch Recovery and Continuum Outpatient Center, individuals have access to flexible outpatient options that support sustained recovery while allowing them to maintain work and family commitments.
Long-Term Support Networks in San Antonio
Peer Support and Mutual Aid Communities
Peer support and mutual aid communities serve as a vital foundation for long-term recovery in San Antonio. These groups offer a space where individuals can share experiences, learn from others, and receive encouragement without judgment. The sense of belonging found in these communities helps normalize the ups and downs of recovery, including the reality that setbacks can be part of the process rather than a sign of failure.

In neighborhoods like Woodlawn Lake, Southtown, and Stone Oak, peer support groups meet regularly, making recovery accessible across much of the city. Whether you are taking VIA Metropolitan Transit or driving down US-281, finding a local meeting is easier than ever. Research highlights the significant impact of mutual aid: participation in peer-led groups is associated with a 35% lower risk of returning to use compared to other forms of treatment, underscoring the power of connection in supporting sustained change.7
Take Sarah, a professional working near the Convention Center. She found that connecting with a local alumni group provided the exact accountability she needed to navigate high-stress corporate events. Relapse prevention programs San Antonio frequently incorporate peer networks into their ongoing care models, recognizing that consistent support beyond the clinical setting is key to lasting wellness. This approach empowers individuals and families to remain engaged with recovery through every stage.
Outpatient and Telehealth Continuation Options
Outpatient and telehealth services have become essential pillars of relapse prevention programs San Antonio, providing critical continuity for individuals rebuilding their lives across neighborhoods such as North Central, Midtown, and the Medical Center district. Flexible outpatient care—including intensive programs and step-down support—allows participants to maintain daily commitments while receiving ongoing therapeutic, psychiatric, and medication management. This approach is especially valuable for those balancing work, school, or family responsibilities in busy areas like The Pearl and Terrell Hills.
Telehealth has dramatically expanded access to care, making it possible to connect with licensed clinicians and peer support from home or work. Recent research confirms that telehealth outcomes for recovery are comparable to in-person services, with similar rates of treatment retention.9 By bridging transportation gaps and reducing barriers related to traffic or parking, telehealth ensures that help is always within reach—whether someone lives near Downtown or on the city’s outskirts.
A lapse, when it happens, should be seen as a prompt to reengage with these support systems, not as a failure. Outpatient and telehealth options, like those offered by Continuum Outpatient Center, work together to provide the ongoing connection and professional guidance needed to adjust recovery strategies as life circumstances shift.9
Frequently Asked Questions
What areas of San Antonio do relapse prevention programs serve?
Relapse prevention programs San Antonio are accessible throughout the entire metro area, ensuring support for individuals and families in neighborhoods like Alamo Heights, Stone Oak, Southtown, and the Medical Center district. Many programs are conveniently located near central landmarks, such as the River Walk and The Pearl, and are accessible by major routes like I-35 and Loop 410, making it easier to attend sessions regardless of traffic patterns or parking concerns. Telehealth services extend coverage even to those living on the outskirts or in areas where transportation is a barrier. Recent studies confirm that telehealth and in-person options deliver similar results, allowing people to remain connected to care wherever they live in San Antonio9.
How soon after a lapse should someone seek professional support?
Seeking professional support as soon as possible after a lapse is strongly recommended. Even a single use or close call can be a valuable opportunity to adjust recovery strategies before patterns become entrenched. Research emphasizes that early intervention helps prevent a lapse from progressing into a full relapse and can significantly improve long-term recovery outcomes2. There is no “waiting period”—the sooner support is accessed, the more effective relapse prevention programs San Antonio can be in helping individuals regain stability and confidence. Reaching out quickly also reduces shame and isolation, instead reinforcing that setbacks are a normal, treatable part of recovery10.
Can someone participate in relapse prevention while maintaining employment?
Yes, many relapse prevention programs San Antonio are designed to support individuals who are actively employed. Flexible outpatient schedules, evening and weekend group sessions, and telehealth options make it possible to participate in therapy or peer support without interrupting work commitments. In busy areas like Downtown or the Medical Center, telehealth services have proven just as effective as in-person care for maintaining recovery, enabling professionals to attend appointments from home or the office9. By normalizing relapse as a part of recovery, these programs encourage ongoing engagement, even as work and life demands shift. Support is available to adapt recovery strategies while balancing employment and personal responsibilities.
What is the difference between a lapse and a full relapse?
A lapse refers to a single or brief episode of substance use after a period of abstinence, while a full relapse involves a return to previous, sustained patterns of use. Distinguishing between the two helps individuals and families understand that a lapse is not the same as losing all progress—rather, it signals a need to revisit recovery strategies and support systems. Research highlights that relapse is a process, often beginning with emotional or mental triggers before actual use occurs, and a lapse can provide valuable insight for future prevention2. Relapse prevention programs San Antonio encourage acknowledging and addressing lapses quickly to support ongoing recovery.
Are family members included in relapse prevention planning?
Yes, family members are commonly included in relapse prevention planning within relapse prevention programs San Antonio. Involving loved ones helps build a strong support network, improves communication, and can reduce feelings of isolation or shame for the person in recovery10. Family participation often includes education about the stages of relapse, training in healthy boundaries, and learning practical ways to support ongoing recovery efforts. Research shows that strong social support is a significant protective factor against relapse, making family involvement an evidence-based component of long-term success4. Including family members also helps everyone recognize warning signs and respond to setbacks with compassion and flexibility.
How does relapse prevention address co-occurring anxiety or depression?
Relapse prevention programs San Antonio specifically address co-occurring anxiety and depression by providing integrated care—meaning both mental health and substance use concerns are treated together, not separately. This approach often combines evidence-based therapies like Cognitive-Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT) to help individuals manage distressing thoughts and emotions while building coping skills for both conditions. Medication management may also be offered if appropriate. Research shows that treating substance use and mental health conditions at the same time improves long-term recovery outcomes and reduces the risk of relapse5. Support is tailored to each person’s needs, ensuring that anxiety or depression are not overlooked during recovery.
Building Sustainable Recovery in San Antonio
The integrated care approaches that effectively address co-occurring disorders during treatment must extend into long-term recovery planning to create lasting stability. Sustainable recovery reaches far beyond initial treatment completion—it requires understanding that setbacks are often part of the healing journey, particularly when managing both mental health and substance use challenges simultaneously. For individuals navigating these complexities, building a foundation that supports long-term wellness means acknowledging why a lapse happens and implementing specific strategies to maintain progress.
A return to use occurs more frequently with co-occurring disorders because untreated mental health symptoms can trigger cravings, while substance use intensifies psychiatric symptoms. Recovery sustainability depends on consistent engagement with therapeutic support and concrete tools found in relapse prevention programs San Antonio. Evidence-based approaches provide practical strategies for identifying early warning signs, managing triggers specific to both conditions, regulating emotions, and developing healthy coping mechanisms.
Structured aftercare programs create essential continuity between intensive treatment phases and independent living. Ripple Ranch’s aftercare program provides concrete ongoing support including weekly individual therapy sessions, bi-weekly group therapy, and regular psychiatric medication management appointments. Through our partnership with Continuum Outpatient Center, individuals transitioning from residential care can access flexible outpatient services including evening therapy sessions for working professionals and telehealth options for consistent connection. Alumni programs foster lasting connections with others who understand the unique complexities of managing co-occurring disorders, reducing isolation and reinforcing recovery principles throughout the journey toward sustained wellness.
References
- SAMHSA – Medications for Substance Use Disorders. https://www.samhsa.gov/medications-substance-use-disorders
- NCBI – Addiction Relapse Prevention StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK551500/
- VA Whole Health Library – Reducing Relapse Risk. https://www.va.gov/WHOLEHEALTHLIBRARY/tools/reducing-relapse-risk-for-addictive-behaviors.asp
- NCBI – Factors Associated with Relapses in Alcohol and Substance Use Disorders. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8914332/
- NIMH – Finding Help for Co-Occurring Substance Use and Mental Disorders. https://www.nimh.nih.gov/health/find-help
- NCBI – Comparing the Effectiveness of Cognitive-Behavioral Therapy and Brief Intervention for Relapse Prevention. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3212879/
- Mobilize Recovery – The Power of Connection: Peer Support and Mutual Support Groups. https://mobilizerecovery.org/the-power-of-connection-the-role-of-peer-support-and-mutual-support-groups-in-addiction-recovery/
- TXSUS – Update on Local ATOD Statistics in San Antonio and Bexar County. https://txsus.org/wp-content/uploads/2016/09/Update-on-Local-ATOD-Statistics-in-San-Antonio-and-Bexar-County.pdf
- NCBI – Telehealth for Addiction and Mental Health Treatment. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9345262/
- CDC – Stigma Beyond the Numbers: Substance Use Disorder. https://www.cdc.gov/stopoverdose/stigma/index.html
