Figuring out how to help someone who refuses rehab San Antonio can feel like an exhausting, uphill battle, especially when you are watching a loved one struggle with co-occurring disorders. You are not alone, and there are proven, compassionate ways to guide them toward the care they need.
Key Takeaways
- Essential Prerequisites: Patience, empathy, and a willingness to set healthy boundaries without using ultimatums.
- Support Tools: Open-ended questions, motivational language, and professional guidance from dual diagnosis experts.
- Understand the psychological and co-occurring factors driving your loved one’s resistance.
- Avoid confrontation, arguing, and control tactics that increase defensiveness.
- Implement evidence-based communication strategies and establish clear boundaries.
- Involve professional intervention and specialized dual diagnosis care when necessary.
By shifting from confrontation to compassionate support, you can successfully guide your resistant loved one toward the integrated care they need.
Why Resistance to Help Is Common: How to Help Someone Who Refuses Rehab San Antonio
Psychological Mechanisms Behind Treatment Refusal
When someone you care about refuses help, it’s easy to feel powerless and wonder if they’re just being stubborn. But research shows that resistance to treatment is rarely about defiance or not caring—it’s usually a way to protect themselves from fear, shame, or the unknown.5
The truth is, saying no to help often feels safer than facing the changes that recovery brings.
For many, even admitting there’s a problem can feel like opening the door to overwhelming guilt or anxiety. Most people who resist rehab don’t see themselves as ready for change. This isn’t a lack of willpower. It’s a real struggle with uncertainty, mixed emotions, and worry about what life will look like without the comfort of old habits.6
In fact, about 70% of resistance is driven by a person’s ambivalence about change—not because they are unwilling, but because they are caught between wanting things to improve and fearing what comes next.6 Family members often feel responsible, but it’s important to remember that pushing too hard can make loved ones dig in their heels even more.
Gentle, supportive conversations—focused on listening rather than convincing—help reduce shame and can slowly open the door to acceptance.4 Learning how to help someone who refuses rehab San Antonio means understanding these psychological roots. Your compassion and patience matter, and support is available even when it feels like every option has been tried. Next, we’ll look at how co-occurring mental health issues can make resistance feel even stronger.
How Co-occurring Disorders Amplify Resistance
If you’re supporting someone who struggles with both substance use and a mental health condition, you may notice their resistance feels even more intense. Common co-occurring disorders include:
- Depression
- Anxiety
- PTSD
- Bipolar disorder
These co-occurring disorders can make it much harder for a person to accept help or even see the possibility of change. It’s not just a matter of refusing treatment—it’s a tangled knot of emotions, symptoms, and fears that reinforce each other. Someone with both mental health and substance use challenges often feels doubly misunderstood.
Depression may drain their hope, while anxiety makes every step toward change feel overwhelming. Add in substance use, and the cycle becomes even more entrenched. Research shows that when co-occurring anxiety or depression is present, people are three to four times more likely to refuse treatment unless they have access to care that addresses both issues together.3
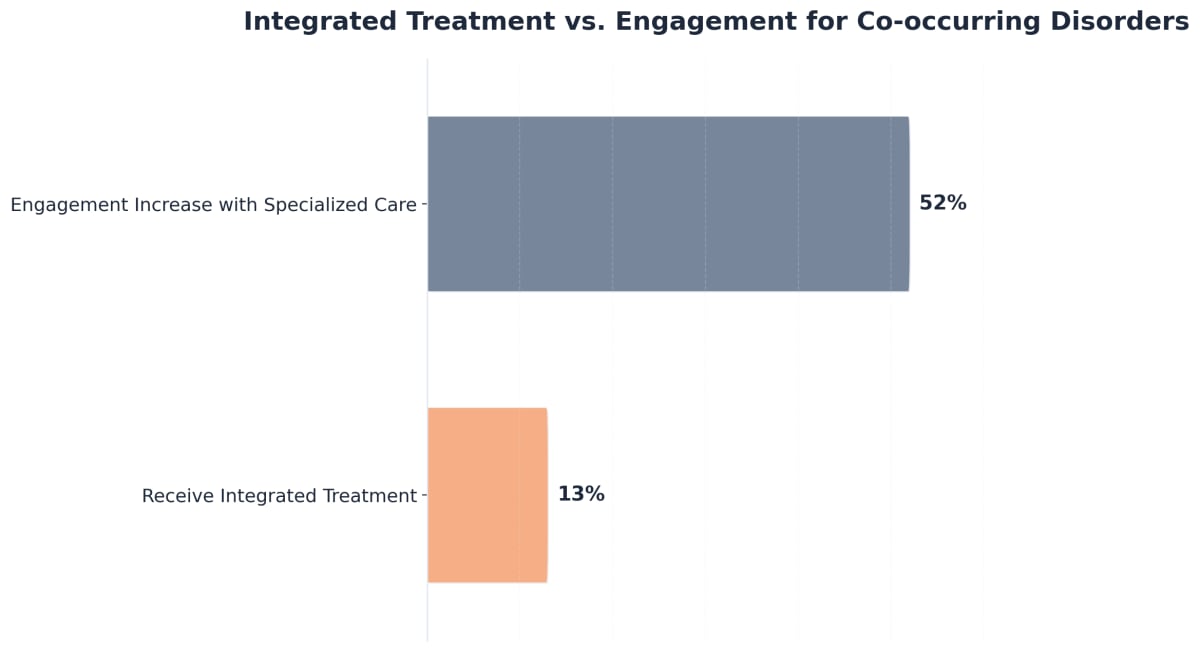
It’s also common for trauma to play a role. Individuals who have experienced trauma may be especially wary of treatment settings, fearing judgment or more pain. This added layer of emotional defense can look like stubbornness, but it’s often self-protection.8 Only 13% of people with co-occurring disorders actually receive the integrated treatment they need, yet specialized care increases engagement by more than 50%.7
If you feel worn out trying to figure out how to help someone who refuses rehab San Antonio, know that this level of resistance is not a sign of failure—yours or theirs. With the right approach, even deeply rooted resistance can shift. Next, we’ll explore why certain approaches, like arguing or forcing, actually make things harder.
What Doesn’t Work: Approaches That Backfire
Why Confrontation Increases Defensiveness
If you’ve found yourself raising your voice or repeatedly confronting your loved one, you’re not alone. It’s natural to want to break through resistance by arguing, pleading, or listing all the reasons why treatment is needed. Unfortunately, these heated conversations often push people even further away.
When someone feels cornered or attacked, their defenses go up. Instead of hearing your concern, they may focus on protecting themselves or proving you wrong. Research shows that confrontation actually increases defensiveness and makes people half as likely to seek help compared to when they feel supported and respected.4
This isn’t just theory—it happens in living rooms, kitchens, and car rides every day. A loved one might walk out, shut down, or throw your words back at you. The more intense the argument, the more likely it is they’ll dig in their heels. It’s important to remember that learning how to help someone who refuses rehab San Antonio means letting go of the idea that you can argue someone into recovery.
Instead, approaching conversations with empathy and patience can open doors that confrontation closes. While this may feel counterintuitive, it’s proven to be more effective in the long run.4 In the next section, we’ll look at why ultimatums and control tactics often fail as well, and what you can do instead to encourage real change.
The Failure of Ultimatums and Control Tactics
When every heartfelt conversation seems to go nowhere, it’s tempting to lay down an ultimatum—”Get help or else.” Many loved ones try using threats or control tactics in hope of sparking change. But research and real-life experience show that these approaches almost always backfire.
Ultimatums often leave the person you care about feeling trapped, shamed, or even more determined to assert their independence. Instead of encouraging openness, control tactics tend to breed resentment or secrecy. Someone who feels coerced into treatment is much more likely to disengage or drop out as soon as they can.
| Approach | Impact on Loved One | Likelihood of Seeking Help |
|---|---|---|
| Confrontation & Ultimatums | Increases defensiveness, shame, and secrecy | Significantly decreases engagement |
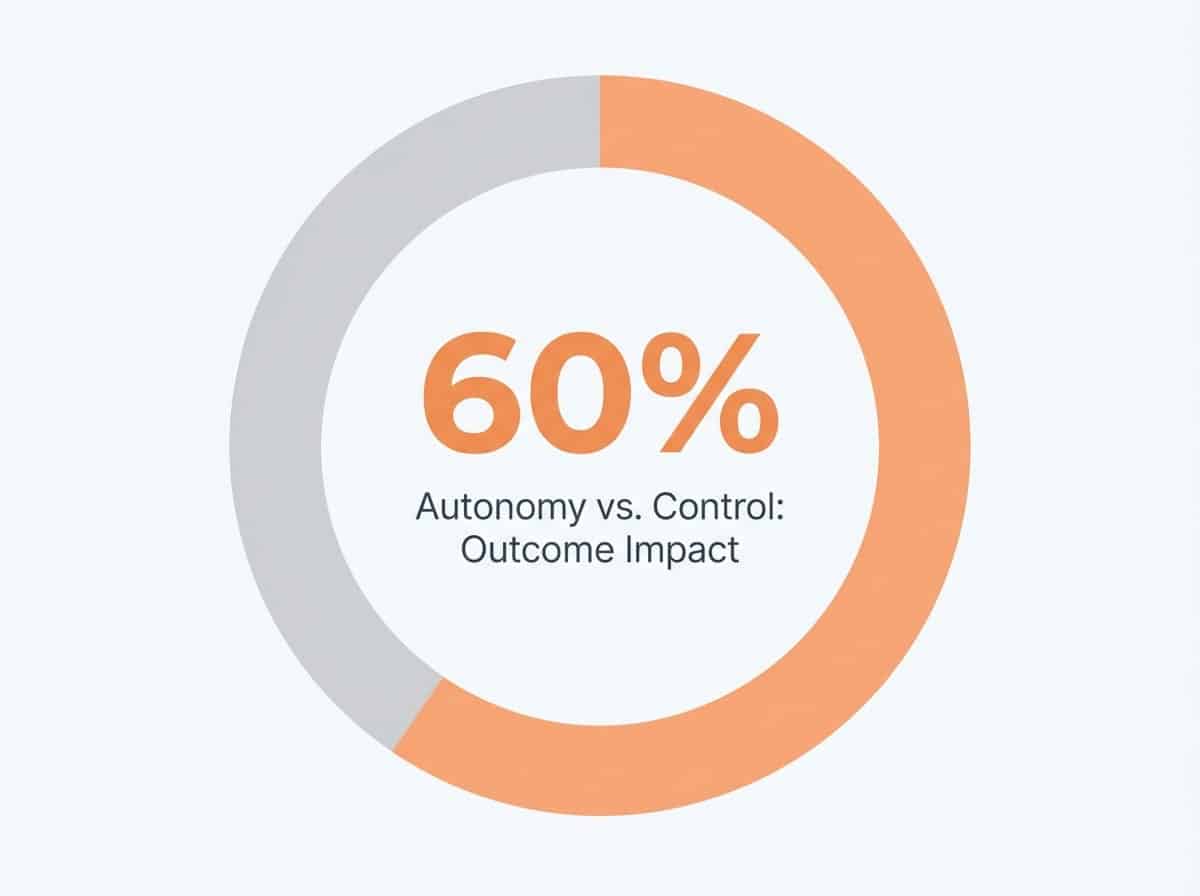
| Autonomy-Supportive Strategies | Fosters trust, dignity, and open dialogue | Produces 60% better outcomes |
Evidence highlights that autonomy-supportive strategies produce 60% better outcomes than controlling approaches, because they honor a person’s sense of agency and dignity.4 The urge to take charge often comes from a place of fear or desperation, but it rarely leads to lasting change.
Control tactics might get a short-term reaction, such as a promise to consider help, but this is usually temporary and not rooted in true readiness for recovery. Those who feel forced may agree to treatment just to appease family, then withdraw the moment pressure eases. If you’re searching for how to help someone who refuses rehab San Antonio, try to resist the urge to issue ultimatums.
Support works best when it’s patient and non-coercive. Real change is most likely when your loved one feels empowered, not controlled. The next section explores practical strategies—like the right timing, language, and healthy boundaries—that actually open the door to change.
Evidence-Based Strategies: How to Help Someone Who Refuses Rehab San Antonio
Motivational Language and Timing Principles
When it feels like nothing you say makes a difference, shifting how and when you talk to your loved one can bring hope back to the conversation. The words you choose and the timing of your approach really matter—especially when learning how to help someone who refuses rehab San Antonio.
Instead of trying to convince, focus on listening and reflecting their feelings. Simple phrases like, “I’m here when you’re ready,” or, “I can see this is hard for you,” lower defenses and show respect for their autonomy. This isn’t about ignoring your own needs; it’s about making space for honest dialogue without pressure or judgment.
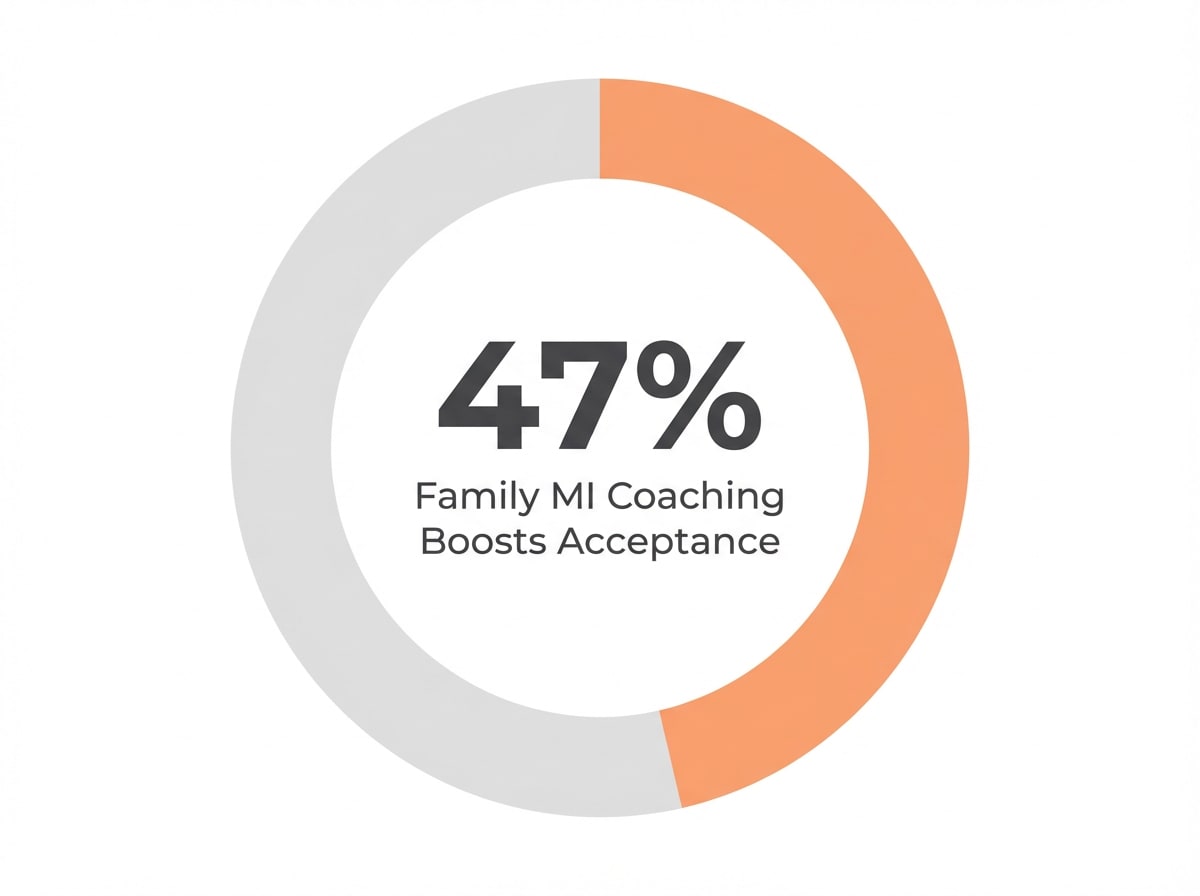
Motivational language, rooted in asking open-ended questions and expressing empathy, has been shown to increase treatment acceptance by up to 47% when families receive coaching in these skills.2 Try to avoid statements that sound like ultimatums or accusations. Instead, highlight positive changes you’ve noticed, or gently ask what worries them most about treatment.
If your loved one opens up, resist the urge to jump in with solutions. Sometimes, just feeling heard is enough to start breaking down resistance. Timing is just as important as language. Bringing up treatment when emotions are running high—right after a conflict or during a crisis—rarely leads to real progress.
Waiting for a moment of calm, or choosing a time when your loved one is more open, can make all the difference.4 These small shifts are not quick fixes, but they set the stage for trust and future change. Next, see how setting boundaries—without ultimatums—can further support your loved one’s journey.
Setting Boundaries Without Ultimatums
Setting boundaries is one of the hardest steps when you’re trying to figure out how to help someone who refuses rehab San Antonio. It often means drawing a line between what you can and cannot accept, not to punish your loved one, but to protect your own well-being and keep the relationship grounded in respect.
The exhaustion and guilt you may feel are real, especially if you worry that having limits will make things worse. But research shows the opposite—healthy boundaries actually lower resentment and build trust over time.5 Boundaries are not about controlling someone else’s choices. Instead, they’re about being clear on what you’ll do if certain behaviors continue.
For example, you might say, “I care about you, but I can’t cover for you at work if you’re using,” or “You’re always welcome here, but not when you’ve been drinking.” Statements like these focus on your own needs rather than making threats. Unlike ultimatums, which often come from fear or frustration, boundaries come from a place of love and self-respect.
Families who set boundaries without giving ultimatums see a 38% increase in treatment engagement compared to those who use threats or control tactics.9 If your loved one pushes back or tests your limits, remember that this reaction is common. Consistency is key—even if it feels uncomfortable at first.
Over time, your loved one may begin to understand that your boundaries are about caring for both of you, not about abandoning them. If you’re struggling with what boundaries look like in your situation, there are professionals who can help you practice and adjust as needed.4 Establishing boundaries is an act of hope, not defeat. Next, we’ll talk about when it’s time to seek outside support and how expert guidance can change the path forward.
When to Involve Professional Guidance
Signs That Specialized Intervention Is Needed
Knowing when to seek outside help can feel overwhelming, especially if you’ve tried every supportive approach and your loved one still refuses treatment. Sometimes, the signs that specialized intervention is needed aren’t dramatic—they build up slowly, leaving you feeling anxious, exhausted, or even hopeless.
Common Red Flags Requiring Professional Help
Escalating substance use, repeated crises (like medical emergencies or legal trouble), or a pattern of broken promises about change are strong indicators that outside intervention is necessary.
If your loved one’s behavior puts their safety at immediate risk, or if mental health symptoms like depression or paranoia make conversations impossible, these are strong signals that professional support is necessary.5 You might also notice your own boundaries aren’t working, or that family life has become dominated by chaos, fear, or secrecy.
In these moments, reaching out for guidance is not admitting defeat—it’s recognizing that some situations are simply too big to handle alone. Family-guided interventions led by professionals result in 40% higher treatment engagement rates, showing that expert support can make a real difference.5
If you’re wondering how to help someone who refuses rehab San Antonio, remember: asking for help is a sign of strength, not failure. Next, see how expertise in dual diagnosis care can transform these challenging situations.
How Dual Diagnosis Expertise Changes Outcomes
When a loved one faces both substance use and a mental health challenge, the path to recovery often feels steeper and more unpredictable. In these moments, dual diagnosis expertise makes a real difference. Instead of treating mental health and substance use as separate issues, specialized care addresses both together—helping to unravel the cycle of fear, shame, and avoidance that keeps people stuck.
Only 13% of people with co-occurring disorders actually receive this kind of integrated treatment, but when they do, engagement rises by more than 50%.7 For families exhausted by setbacks or refusals, dual diagnosis professionals offer more than a treatment plan. They bring understanding of how depression, anxiety, trauma, and substance use often reinforce each other.
This approach isn’t about pushing someone into change; it’s about creating the safety and trust needed for small steps forward. Techniques such as motivational interviewing and trauma-informed care help lower defenses, making it safer for your loved one to consider help—even if they’ve said no a hundred times before.
If you’re searching for how to help someone who refuses rehab San Antonio, know that dual diagnosis programs can turn even the hardest resistance into hope. The next section highlights how families are supported throughout this journey, before, during, and after treatment.
Frequently Asked Questions
What if my loved one agrees to treatment but then backs out at the last minute?
It’s common for a loved one to agree to treatment and then back out just before taking that final step. This can leave you feeling defeated, angry, or even questioning what went wrong. Know that this kind of last-minute withdrawal usually isn’t about a lack of love or effort—it often means your loved one is overwhelmed by fear, shame, or uncertainty about change 5. Many people experience what’s called “motivational ambivalence,” where the desire for help collides with the anxiety of letting go of old habits 6.
If you’re searching for how to help someone who refuses rehab San Antonio, remember: setbacks are part of the process. Reassure your loved one that your support is still there, and try to keep lines of communication open. Sometimes, it takes several tries before someone feels ready to commit.
How can I tell if resistance is caused by fear versus a genuine lack of readiness for change?
It’s natural to wonder whether your loved one’s resistance is about fear or a true lack of readiness for change. Often, these feelings overlap. Many people push back against treatment because facing the unknown is scary or because they fear judgment and failure 5. Research shows that about 70% of resistance comes from ambivalence—not a total unwillingness, but being stuck between wanting help and being afraid of what recovery might mean 6. Signs of fear-based resistance might include saying, “What if I can’t do it?” or worrying about disappointing others. A genuine lack of readiness may sound more like, “I don’t have a problem,” or “I’m fine the way things are.”
If you’re feeling stuck on how to help someone who refuses rehab San Antonio, keep in mind that patience and open communication can help uncover what’s really behind their hesitation.
Are there insurance coverage options in Texas for dual diagnosis treatment when someone initially refuses?
Yes, there are insurance coverage options in Texas for dual diagnosis treatment—even if your loved one is not ready to start right away. Many insurance plans, including those through the Affordable Care Act and most major employers, are required by law to cover both substance use and mental health services under mental health parity rules 10. This means coverage for integrated treatment is protected, though the exact benefits can vary by plan. In Texas, recent updates have expanded access and lowered some barriers to care for co-occurring disorders 10. If you’re trying to learn how to help someone who refuses rehab San Antonio, you can contact treatment centers or insurance providers directly to ask about pre-approval, coverage, and what steps to take if your loved one changes their mind. Support is available to help families navigate these details, even before treatment begins.
What should I do if my loved one’s substance use is putting them in immediate danger but they still refuse help?
If your loved one’s substance use is putting them in immediate danger but they still refuse help, your fear and exhaustion are understandable. In crisis situations—such as overdose risk, suicidal threats, or severe withdrawal—your first priority is safety. Don’t try to manage this alone. Call emergency services if there’s any risk to life or serious harm. Medical professionals can assess the situation and may initiate protective steps. Texas law allows for emergency evaluation if someone is a danger to themselves or others, though involuntary treatment is a last resort and carries emotional weight 5. Even if your loved one is resistant, your steady support and willingness to involve professionals can make a difference. Remember, learning how to help someone who refuses rehab San Antonio sometimes means acting quickly for safety, while still offering care and hope afterward.
How long should I wait between conversations about treatment before trying again?
It’s understandable to wonder how long you should wait before bringing up treatment again, especially if past conversations haven’t led to change. Research on how to help someone who refuses rehab San Antonio suggests waiting at least a few days to a week between conversations, unless there’s an urgent safety issue 4. Giving your loved one breathing room helps lower defensiveness and shows respect for their autonomy. Use the time in between to check in about everyday things, not just recovery, so your relationship doesn’t become defined by conflict. When you do revisit the topic, pick a calm moment and focus on listening—not persuading. This gentle persistence, paired with patience, is more likely to open the door to change over time.
Can telehealth or virtual support help someone who refuses in-person treatment in San Antonio?
Yes, telehealth and virtual support can be a lifeline for someone who refuses in-person treatment in San Antonio. Many people hesitate to walk into a clinic due to shame, anxiety, or fear of being judged, but connecting with help from home can feel safer and less overwhelming. Virtual therapy, family sessions, and online support groups make it easier for your loved one to take small steps at their own pace. Recent research shows that removing barriers like travel and stigma through telehealth increases treatment initiation by nearly 48%, especially for those who have resisted traditional settings 10. If you’re exploring how to help someone who refuses rehab San Antonio, consider starting with virtual options as a gentle bridge toward change.
What role do peer support specialists play when someone is resistant to professional treatment?
Peer support specialists can be a lifeline when your loved one resists professional treatment. Unlike therapists or doctors, these individuals have walked their own path through recovery. They know firsthand what it feels like to be afraid, angry, or doubtful about getting help. Peer support specialists listen without judgment and share their own stories, which can break down walls that formal authority figures sometimes build up. Research shows that peer support reduces treatment rejection rates and helps people feel understood, not alone 3. For families searching for how to help someone who refuses rehab San Antonio, connecting your loved one with a peer specialist offers hope—a reminder that change is possible, even if it starts small.
Compassionate Support Before, During, and After
If you’ve watched someone you love struggle with both substance use and mental health challenges, you know the exhaustion that comes from feeling like you’ve tried everything. You’ve pleaded, reasoned, offered support, and maybe even issued ultimatums—yet nothing seems to break through. The fear, anger, and guilt can be overwhelming, especially when the person you care about continues to resist help for co-occurring disorders. You’re not alone in this, and their resistance doesn’t mean change is impossible.
Understanding why people resist help for co-occurring disorders is the first step toward finding what actually works. Someone might refuse treatment because they’re terrified of facing painful emotions without substances to numb them. They may fear judgment, worry about losing control, or genuinely not recognize how serious things have become.
Perhaps they’ve tried treatment before and it didn’t address their depression alongside their addiction, leaving them feeling like nothing will ever help. When someone is dealing with both mental health symptoms and substance use, the shame and confusion multiply—making resistance feel safer than vulnerability.
What doesn’t work is forcing the issue. Arguing, threatening, or delivering ultimatums when emotions are high typically pushes people further away. Trying to control their choices or “save” them from consequences often backfires, creating more resentment than motivation. When loved ones try to manage someone’s recovery for them, it can actually reinforce the resistance rather than opening the door to help for co-occurring disorders.
What can help is approaching the conversation differently. Setting clear, compassionate boundaries protects your own wellbeing while showing that you care without enabling. Timing matters—choosing calm moments rather than crisis points to express concern makes it easier for them to actually hear you. The language you use matters too: “I’ve noticed you seem really overwhelmed lately, and I’m worried” lands differently than “You need to get help or else.”
Sharing specific observations without judgment, offering to research options together, and emphasizing that treatment for co-occurring disorders addresses both the substance use and the underlying pain can make professional support feel less threatening. You can easily search for resources online using terms like dual diagnosis treatment or press Enter on your provider’s portal to explore telehealth options.
Sometimes, despite your best efforts, professional guidance becomes necessary. If you’re unsure how to start the conversation, when to step back, or how to protect yourself while still offering support, reaching out for family guidance can provide clarity. Ripple Ranch Recovery understands that families need support too—even before a loved one is ready to begin treatment for co-occurring disorders.
Their team can help you navigate these difficult conversations, understand what your loved one might be experiencing, and identify the most effective ways to encourage them toward help without damaging your relationship. At Ripple Ranch Recovery, the approach to treating co-occurring disorders recognizes that mental health and substance use are deeply interconnected.
Their integrated care model addresses anxiety, depression, PTSD, or bipolar disorder alongside addiction—because treating one without the other rarely leads to lasting recovery. Evidence-based therapies like CBT, DBT, and EMDR are combined with holistic support including trauma therapy, mindfulness practices, and medication management when appropriate. This comprehensive approach creates a foundation where healing both conditions simultaneously becomes possible.
Recovery support doesn’t end when primary treatment concludes. Through alumni programs, continued therapy access, and connection to Continuum Outpatient Center, individuals receive ongoing care that adapts as their needs change. This continuum approach acknowledges that managing co-occurring disorders is a long-term journey, not a single event—and that sustained support makes all the difference in navigating real-world challenges while maintaining progress.
If you’re feeling stuck, exhausted, or unsure what to do next, Ripple Ranch Recovery is here to help—even if your loved one isn’t ready to walk through the doors yet. You don’t have to navigate this alone. Reach out today for guidance on how to support someone struggling with co-occurring disorders, protect your own wellbeing, and find hope when everything feels impossible.
References
- SAMHSA National Helpline and Treatment Locator. https://www.samhsa.gov/find-help/treatment
- NIH Research: Family Members Helping Loved Ones with Addiction. https://www.nih.gov/news-events/news-releases/nih-study-shows-family-members-can-help-loved-ones-overcome-opioid-addiction
- American Psychiatric Association: Mental Illness and Substance Use Disorders. https://www.psychiatry.org/patients-families/what-is-mental-illness/mental-illness-substance-use-disorders
- Motivational Interviewing and Treatment Adherence. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5845387/
- National Alliance on Mental Illness (NAMI) Family Support Resources. https://www.nami.org/Get-Involved/Awareness-Events/Mental-Health-Awareness-Month
- Stages of Change Model and Treatment Resistance. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5022106/
- SAMHSA Co-occurring Disorders Information. https://www.samhsa.gov/co-occurring-disorders
- Trauma and Substance Use: Family Dynamics. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5123062/
- Efficacy of Family Intervention Programs for Substance Use. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6581095/
- Systemic Barriers to Substance Abuse Treatment Access. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5123056/
