Key Takeaways
- Skill Progression Roadmap: Learn the physiological mechanics of dependence (Module 1, ~15 mins) and progress to identifying clinical indicators for professional care (Module 2, ~20 mins).
- Essential Resources: Discover how Medication-Assisted Treatment (MAT) and integrated dual diagnosis care provide the necessary tools for safe withdrawal.
- Competency Checklist: Use our self-assessment criteria to determine when you are ready to transition from evaluating your symptoms to seeking medically-supervised detox.
Understanding Drug Withdrawal Physiology
How Substance Dependence Alters Brain Chemistry
What you’ll learn: In this section, you’ll learn how ongoing substance use causes the brain to adapt, leading to deep changes in brain chemistry, and we will address the critical question: is it safe to detox from drugs at home? You’ll know you’ve understood the concept when you can clearly describe how these changes drive both dependence and the difficult symptoms of withdrawal.

When you use substances regularly, your brain tries to keep balance by adjusting how it works. Think of your nervous system like a computer’s operating system. If you constantly run a program that slows the system down, the computer compensates by speeding up its baseline processes. In technical terms, introducing substances rewires your base_code.sys. Removing them abruptly is like forcing a system shutdown without saving, or pressing Ctrl + Alt + Delete while the system is overwhelmed.
For example, with alcohol or benzodiazepines, the brain reduces its own calming signals because it expects these drugs to provide that effect. If the substance suddenly stops, the brain is left in a state of overactivity, which can lead to symptoms like anxiety, restlessness, or even seizures.4, 6 With opioids, the brain’s own pain-relief system slows down, so when opioids are removed, the body can feel pain and distress more intensely.3
This process is at the heart of why so many people ask, is it safe to detox from drugs at home? The answer is complex because these brain changes mean that withdrawal is not just uncomfortable—it can be medically dangerous, especially without professional support.2, 8
- Practice This: Create a simple chart showing how one type of substance affects brain chemical signals over time and what happens when the substance is removed.
- Skill checkpoint: You’re ready for the next level when you can explain the difference between physical dependence and psychological reliance in terms of brain chemistry.
Withdrawal as a Neurological Crisis
What you’ll learn: How drug withdrawal can escalate into a neurological crisis, and how to recognize when symptoms move beyond discomfort to medical danger. You’ll know you’ve understood this topic when you can describe why withdrawal is not just a physical event, but a significant risk to brain and body health.
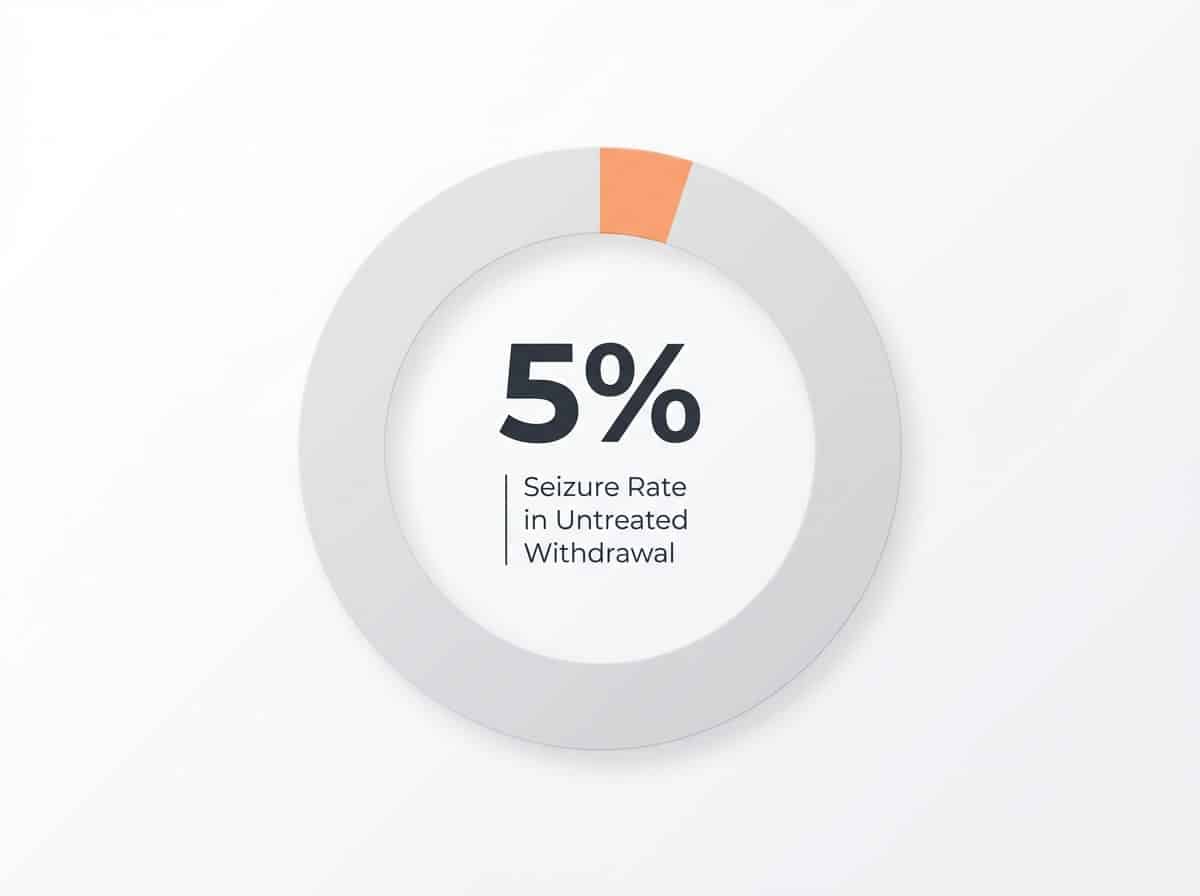
When the brain loses the stabilizing effect of a substance it has adapted to, nerve cells can become hyperactive. For certain substances—especially alcohol and benzodiazepines—this sudden shift can trigger seizures, hallucinations, or even delirium tremens, a severe syndrome that is fatal in up to 25% of untreated cases.5
“Withdrawal is not merely the absence of a substance; it is a profound neurological rebound that requires careful, clinical stabilization to prevent lasting harm.”
The body’s stress response surges, leading to rapid heart rate, dangerously high blood pressure, and confusion, all signs that the nervous system is overwhelmed.4, 8 This is why the question is it safe to detox from drugs at home deserves serious consideration. What starts as anxiety or insomnia can quickly become life-threatening if the nervous system destabilizes.
Medical supervision can spot these shifts early and intervene before a crisis develops, dramatically reducing complications and improving long-term outcomes.2, 8
- Practice This: Write a list of symptoms that might signal a neurological emergency during withdrawal, such as seizures or severe confusion.
- Skill checkpoint: You’re ready for the next level when you can explain why sudden withdrawal from certain substances can be so dangerous—and how timely medical care can prevent tragedy.
Medical Risks of Unsupervised Detoxification: Is It Safe to Detox from Drugs at Home?
Life-Threatening Complications by Substance Class
What you’ll learn: You’ll learn to identify which classes of substances carry the highest risk for life-threatening complications when someone attempts detox outside of a medical setting. You’ll know you’ve mastered this material when you can explain why each type of drug presents unique dangers and describe the specific emergencies that may develop.
Central nervous system depressants—such as alcohol and benzodiazepines—are linked with the most critical withdrawal risks. Abrupt cessation of alcohol can result in seizures, hallucinations, or delirium tremens, a condition with a high mortality rate if not promptly treated.5 Benzodiazepine withdrawal can similarly provoke seizures and severe agitation, especially after long-term use, making unsupervised detox highly unsafe.6, 8
Opioid withdrawal, while rarely fatal, can still be medically complicated. Symptoms like relentless vomiting, diarrhea, and dehydration can lead to dangerous electrolyte imbalances or cardiac issues, particularly for those with pre-existing health concerns.2, 3 Stimulant withdrawal (from substances like cocaine or methamphetamine) is less likely to cause physical crises, but severe depression and suicidal thoughts are common, requiring close psychiatric supervision.7, 8
These risks explain why the question is it safe to detox from drugs at home must be taken seriously. Medical professionals universally recommend supervised detox for anyone dependent on depressants or opioids, as evidence shows that at-home attempts lead to a tenfold increase in relapse within one month and a much higher risk of emergency complications.4, 9
| Substance Class | Primary Medical Risks During Withdrawal | Recommended Intervention |
|---|---|---|
| Central Nervous System Depressants (Alcohol, Benzodiazepines) | Seizures, hallucinations, delirium tremens, severe agitation. | 24/7 Medically-supervised detox with tapering protocols. |
| Opioids (Heroin, Fentanyl, Prescription Painkillers) | Severe dehydration, electrolyte imbalance, cardiac stress, intense cravings. | Medication-Assisted Treatment (MAT) to stabilize physical symptoms. |
| Stimulants (Cocaine, Methamphetamine) | Severe depression, suicidal ideation, extreme fatigue. | Psychiatric supervision and integrated mental health care. |
- Practice This: Review the table above and match each substance group to its primary medical risk during withdrawal.
- Skill checkpoint: You’re ready for the next section when you can confidently articulate the distinct dangers associated with depressant versus stimulant withdrawal.
The Kindling Effect and Progressive Severity
What you’ll learn: You’ll learn what the kindling effect is, why it makes each withdrawal episode riskier, and how it can turn repeated at-home detox attempts into a medical emergency. You’ll know you’ve understood this concept when you can explain why withdrawal becomes more severe and dangerous with every recurrence.
The kindling effect refers to the process where repeated cycles of withdrawal sensitize the brain’s nervous system, causing each subsequent withdrawal to be more intense and hazardous. Imagine a spark starting a small fire—the first withdrawal might bring mild tremors or anxiety. But with each new attempt, the “fire” grows; symptoms like seizures, hallucinations, and delirium tremens become more likely, even if previous detoxes were less severe.4
Attempt 1: Mild Anxiety
↓
Attempt 2: Tremors & Insomnia
↓
Attempt 3: Seizures & Delirium
(The Kindling Effect: Sensitization of the Nervous System Over Time)
When evaluating is it safe to detox from drugs at home, the kindling effect is a primary reason the answer is often no. Attempting detox at home not only exposes you to immediate medical dangers, but also sets the stage for this sensitization process to take hold. Medical research shows that individuals who go through repeated unsupervised withdrawals are far more likely to experience severe neurological crises.4
- Practice This: Write a brief case summary describing how an individual’s withdrawal symptoms changed after multiple attempts to detox without medical support.
- Skill checkpoint: You’re ready for the next level when you can clearly explain how the kindling effect increases both the severity and unpredictability of withdrawal episodes.
Evidence-Based Protocols for Safe Detox
Medication-Assisted Treatment During Withdrawal
What you’ll learn: You’ll gain an understanding of how medication-assisted treatment (MAT) works during withdrawal, why it is considered a cornerstone of safe detox, and what makes it more effective than attempting to detox without medical support. You’ll know you’ve learned the essentials when you can describe the main types of medications used for withdrawal management.
Medication-assisted treatment during withdrawal is designed to reduce the intensity of symptoms and lower the risk of medical emergencies. For example, clinicians may prescribe specific medications to ease cravings, stabilize mood, and prevent seizures—making the process much safer than at-home detox efforts. For opioid withdrawal, medications like buprenorphine or methadone can address both physical discomfort and cravings, dramatically increasing the odds of completing detox and staying in recovery.10
Deep Dive: How MAT Stabilizes the Brain
Medication-Assisted Treatment works by occupying the same receptors in the brain that the substance previously activated, but without producing the harmful highs and lows. This allows the nervous system to gradually return to a baseline state, significantly reducing the shock of withdrawal and minimizing cravings.
For alcohol or benzodiazepine withdrawal, carefully monitored use of medications (in a controlled, tapering protocol) can prevent seizures and delirium tremens, which are potentially fatal complications.5, 6 Evidence shows that professional intervention can boost long-term recovery rates by up to 40% compared to those who attempt withdrawal alone.4, 9
This is one reason the question is it safe to detox from drugs at home has a clear answer from most medical professionals: true safety and best outcomes require structured, evidence-based protocols, not willpower alone.
- Practice This: Create a chart listing the most common MAT medications by substance type, and note their primary purpose in withdrawal management.
- Skill checkpoint: You’re ready for the next section when you can explain how MAT lowers both immediate and long-term risks of withdrawal.
Integrated Care for Co-Occurring Conditions
What you’ll learn: You’ll discover why integrated care—addressing both substance withdrawal and mental health conditions at the same time—is essential for safe detox and sustainable recovery. You’ll know you’ve learned the concept when you can explain how simultaneous treatment of co-occurring disorders improves immediate safety and long-term outcomes.
For many individuals, substance use does not exist in isolation; anxiety, depression, PTSD, or bipolar disorder are often present alongside dependency. Attempting detox without professional support leaves these mental health needs unaddressed, increasing the risk of severe psychological distress, relapse, or even self-harm during withdrawal.3, 8 In fact, studies show that up to 75% of people seeking addiction treatment have at least one co-occurring mental health condition.20
When considering is it safe to detox from drugs at home, the presence of co-occurring disorders makes professional care mandatory. Integrated care means that during medically-supervised detox, clinicians monitor for both physical withdrawal symptoms and mental health crises, adjusting treatment plans accordingly. This approach might include counseling, medication management for mood or anxiety, and trauma-informed support.
Evidence-based protocols demonstrate that managing both substance withdrawal and co-occurring disorders together dramatically improves safety and recovery rates compared to focusing on addiction alone.3, 8 For example, a person with depression may receive antidepressant support alongside detox medications, reducing the risk of suicidal thoughts that can emerge as substances leave the system.
- Practice This: Write a brief summary of how an integrated care plan might look for someone with both opioid use disorder and anxiety during detox.
- Skill checkpoint: You’re ready for the next section when you can describe how treating mental health and substance withdrawal together reduces both medical dangers and the likelihood of relapse.
Clinical Indicators for Medically-Supervised Detox: Is It Safe to Detox from Drugs at Home?
Recognizing when withdrawal symptoms require professional medical oversight can be lifesaving. Many individuals wonder, is it safe to detox from drugs at home, but certain clinical indicators signal the absolute need for medically-supervised detox to ensure safety and comfort during this critical phase of recovery. At Ripple Ranch Recovery Center in Spring Branch, Texas, comprehensive assessments help determine when medically-supervised detox becomes essential for individuals with substance use disorders, particularly those with co-occurring mental health conditions.
Track 1: Personal Application. If you are evaluating your own symptoms, note any history of severe withdrawal. Track 2: Clinical Understanding. For those supporting a loved one, observe behavioral shifts that indicate escalating physical distress.
Individuals who have been using alcohol heavily for an extended period require medically-supervised detox as an essential first step. Alcohol withdrawal can produce life-threatening complications including seizures, delirium tremens, and severe cardiovascular instability. These symptoms typically emerge 6-48 hours after the last drink and can escalate rapidly without proper medical intervention.
The unpredictability of alcohol withdrawal makes professional monitoring non-negotiable for anyone with a history of heavy drinking. Ripple Ranch’s medically-supervised detox program provides 24/7 clinical oversight on their 20+ acre facility, ensuring individuals receive immediate intervention when complications arise. Benzodiazepine dependence presents similar risks requiring medically-supervised detox. Individuals who have been taking medications like Xanax, Valium, or Ativan regularly face dangerous withdrawal symptoms including seizures and severe anxiety when stopping abruptly.
Medically-supervised detox allows for a carefully controlled tapering protocol that minimizes these risks while keeping individuals comfortable throughout the process. This controlled approach is particularly important for those managing co-occurring anxiety disorders alongside benzodiazepine dependence. Opioid withdrawal, while typically not life-threatening, can be extraordinarily uncomfortable and often leads to relapse without proper support.
Individuals dependent on heroin, fentanyl, or prescription painkillers benefit significantly from medically-supervised detox that provides access to medications reducing withdrawal symptoms. Ripple Ranch’s medication-assisted treatment options during medically-supervised detox dramatically increase the likelihood of completing detox successfully and transitioning into comprehensive residential treatment.
Personal health history also influences whether medically-supervised detox is necessary. Individuals with cardiovascular disease, diabetes, liver disease, or other chronic medical conditions face additional risks during withdrawal, as the physiological stress can exacerbate these issues. Medical supervision ensures that healthcare providers can monitor vital signs, adjust medications, and respond immediately to any complications that arise during the detoxification process.
Co-occurring psychiatric conditions requiring ongoing medication management strongly indicate the need for medically-supervised detox. Individuals managing depression, anxiety, PTSD, or bipolar disorder alongside addiction benefit from coordinated care that ensures psychiatric medications are appropriately adjusted while they safely withdraw from substances. This dual diagnosis consideration is central to Ripple Ranch’s treatment philosophy, where integrated care addresses both substance use disorders and mental health conditions simultaneously.
Specialized Dual Diagnosis Detox Services
When clinical indicators reveal the complex interplay between substance dependence and co-occurring mental health conditions, specialized dual diagnosis detox becomes essential for addressing your complete clinical picture. If you are asking yourself is it safe to detox from drugs at home while managing a mental health condition, specialized dual diagnosis detox becomes essential. Ripple Ranch Recovery’s integrated dual diagnosis program provides comprehensive treatment that simultaneously manages withdrawal symptoms while stabilizing conditions like depression, anxiety, PTSD, and bipolar disorder through evidence-based protocols designed specifically for co-occurring disorders.
The program recognizes that your psychiatric condition and addiction influence each other in complex ways, requiring coordinated intervention from the start. During detox, emotional and cognitive symptoms can intensify, while withdrawal can mimic or worsen existing behavioral health challenges. Ripple Ranch’s specialized team includes both addiction medicine specialists and psychiatric professionals who work together to adjust medications and interventions as your body and mind respond to treatment.
They utilize evidence-based therapies including Cognitive Behavioral Therapy (CBT), Dialectical Behavior Therapy (DBT), and Eye Movement Desensitization and Reprocessing (EMDR) alongside medication management capabilities. The therapeutic environment at Ripple Ranch’s Texas facility creates space for comprehensive assessment and integrated care that prevents the fragmented treatment that occurs when addiction and psychological services operate separately.
Their trauma-informed approach combines psychiatric support with holistic treatments including yoga, meditation, and nutrition therapy, addressing both immediate stabilization needs and underlying trauma patterns. This integrated methodology has demonstrated measurable results, with 93% treatment goal achievement and 89% patient satisfaction rates reflecting the effectiveness of their whole-person approach.
Through their partnership with Continuum Outpatient Center, Ripple Ranch ensures continuity of care extends beyond initial stabilization, providing seamless transition support as you progress through your recovery journey. When you’re experiencing co-occurring disorders, this specialized dual diagnosis detox ensures both conditions receive appropriate clinical attention from the beginning, establishing a stronger foundation for sustainable long-term wellness.
Frequently Asked Questions
What happens if withdrawal symptoms become severe after starting detox at home?
If withdrawal symptoms become severe after starting detox at home—such as seizures, hallucinations, chest pain, confusion, or uncontrollable vomiting—it is crucial to seek emergency medical help immediately. Severe symptoms often signal that the body and brain are overwhelmed, and complications like seizures or delirium tremens can be life-threatening without prompt intervention 58. Medical professionals use evidence-based protocols to stabilize vital signs, prevent further complications, and manage both physical and mental health crises. Attempting to “wait it out” at home is extremely dangerous; research shows that people detoxing at home have a tenfold increased risk of relapse and medical emergencies compared to those under supervision 49.
How does medically-supervised detox address co-occurring mental health conditions during withdrawal?
Medically-supervised detox is uniquely equipped to address both substance withdrawal and co-occurring mental health conditions. During withdrawal, medical teams can monitor for mood swings, anxiety, depression, or trauma symptoms and adjust care plans in real time. This often includes medication management for both withdrawal and psychiatric symptoms, as well as counseling or therapeutic support to stabilize mental health. Research shows that up to 75% of those seeking addiction treatment have at least one co-occurring mental health disorder, making integrated care essential for safety and relapse prevention 320. This approach greatly reduces the risk of psychological crises during detox and improves long-term recovery outcomes.
Can someone transition directly from detox into ongoing treatment programs?
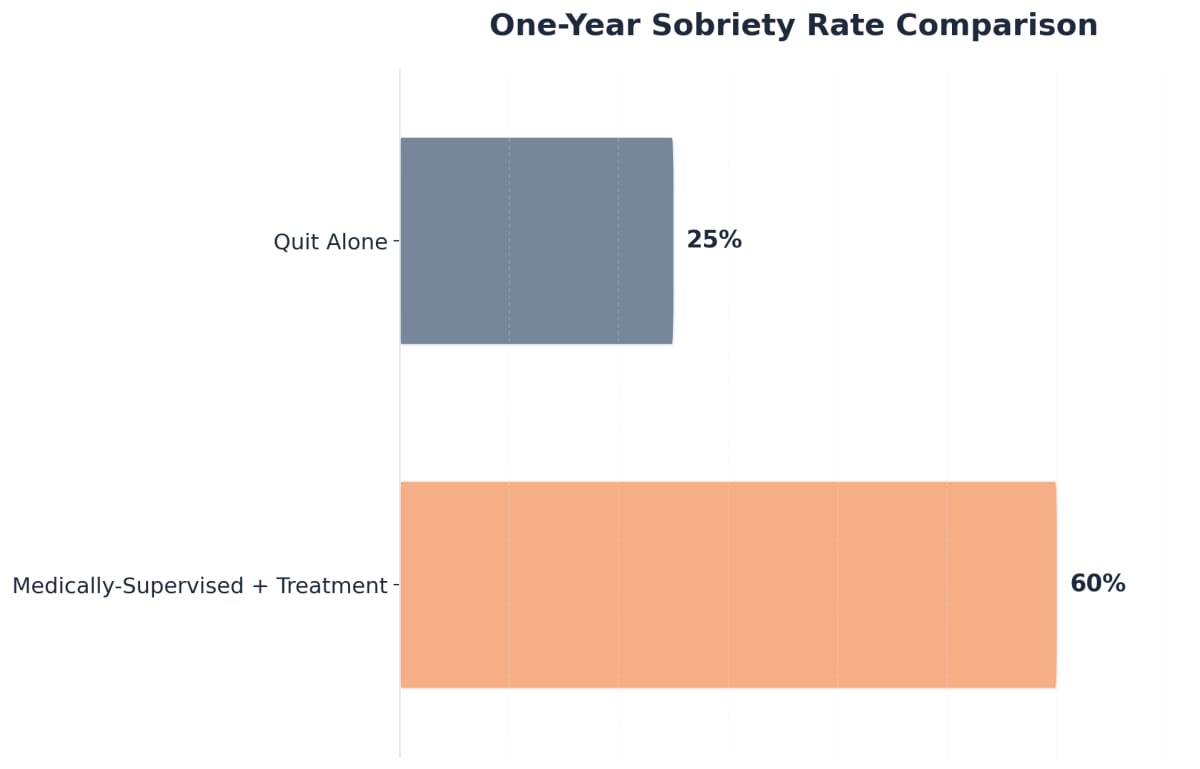
Yes, transitioning directly from medically-supervised detox into ongoing treatment programs is not only possible, but it is also recommended for sustained recovery. Detox serves as the critical first step—stabilizing the body and mind so that you are ready to engage in therapy, medication management, or holistic care tailored for your needs. Research shows that individuals who move from detox straight into structured treatment are far more likely to maintain sobriety over the long term, with up to 60% remaining sober at one year compared to just 25% who attempt recovery alone 49. This seamless transition can help you build on the momentum of detox and access the comprehensive support needed for lasting change.
What role does insurance play in accessing medically-supervised detox services?
Insurance plays a significant role in making medically-supervised detox more accessible for many individuals. Most health insurance plans—including employer-based, private, and government-funded options—cover at least part of the costs associated with detoxification and related addiction treatment services 1. This coverage often includes not only the initial medical management of withdrawal, but also integrated support for co-occurring mental health conditions, which are common among those seeking help 320. Before beginning detox, it’s helpful to check with your insurance provider to understand specific coverage, required authorizations, and any network restrictions. Access to medically-supervised detox through insurance can remove crucial barriers, encouraging safer, evidence-based recovery rather than risking the dangers of unsupervised withdrawal at home.
How do medical professionals monitor vital signs and adjust treatment during detoxification?
During medically-supervised detoxification, medical professionals closely monitor vital signs such as heart rate, blood pressure, temperature, and oxygen levels. This continuous observation allows them to detect early warning signs of complications, including seizures, delirium, or severe dehydration. Based on these findings, the treatment team can adjust medications in real time—such as increasing fluids, administering anti-seizure drugs, or managing symptoms like anxiety and agitation. This proactive approach reduces risks and improves comfort throughout withdrawal. Research shows that such monitoring and responsive adjustments dramatically lower the likelihood of life-threatening emergencies compared to unsupervised detox 258.
What support is available for family members while someone undergoes medically-supervised detox?
Family members play a vital role in the recovery journey, and medically-supervised detox programs typically offer support resources for loved ones throughout the process. This may include access to family education sessions, counseling, and regular updates from the care team, helping families understand withdrawal, set realistic expectations, and manage stress. Some programs facilitate family support groups or offer referrals to community organizations, such as national helplines, for additional guidance 1. By involving families and providing clear communication, medically-supervised detox helps create a supportive environment, which research shows can improve outcomes for everyone involved 3.
Conclusion
Navigating co-occurring disorders requires specialized care that addresses both addiction and psychiatric conditions simultaneously. When symptoms of depression, anxiety, PTSD, or bipolar disorder intersect with chemical dependency, integrated treatment becomes essential for sustainable recovery. This is where medically-supervised detox provides the critical foundation—offering clinical stability while managing withdrawal symptoms safely under expert care.
At Ripple Ranch Recovery in Spring Branch, Texas, individuals throughout the San Antonio and Austin areas find comprehensive dual diagnosis treatment designed specifically for co-occurring disorders. The facility’s full continuum of care begins with medically-supervised detox and extends through residential treatment, intensive outpatient programs, and aftercare services through their partnership with Continuum Outpatient Center.
This integrated approach recognizes that lasting recovery emerges when both conditions receive equal attention through evidence-based therapies like CBT, DBT, and EMDR, combined with holistic treatments including yoga, meditation, and nutrition therapy—all delivered on a peaceful 20+ acre property that supports healing on multiple levels.
Ultimately, when you ask is it safe to detox from drugs at home, the safest path forward involves comprehensive, medically-supervised care. If you’re experiencing the challenges of dual diagnosis, know that specialized support is available and accessible. Ripple Ranch accepts most major insurance plans and offers telehealth services to ensure treatment fits your circumstances.
Their trauma-informed care model, proven outcome metrics (93% treatment goal achievement), and compassionate clinical team create the environment necessary for transformation. From the initial medically-supervised detox through long-term aftercare, every phase of treatment addresses the whole person. Recovery becomes possible when you receive care that honors both your emotional health and your journey toward freedom from dependency. Reach out today to learn how Ripple Ranch’s integrated dual diagnosis program can support your path to wellness—because you deserve comprehensive care that addresses all aspects of your experience.
References
- National Helpline for Mental Health, Drug, Alcohol Issues – SAMHSA. https://www.samhsa.gov/find-help/helplines/national-helpline
- Physical Detoxification Services for Withdrawal From Specific Substances. https://www.ncbi.nlm.nih.gov/books/NBK64116/
- Clinical Guidelines for Withdrawal Management and Treatment of Substance Use Disorders. https://www.ncbi.nlm.nih.gov/books/NBK310652/
- Complications of Alcohol Withdrawal: Pathophysiological Insights. https://pmc.ncbi.nlm.nih.gov/articles/PMC6761825/
- Alcohol Withdrawal Syndrome – StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK441882/
- Benzodiazepine use, misuse, and abuse: A review. https://pmc.ncbi.nlm.nih.gov/articles/PMC6007645/
- Clinical Management of Psychostimulant Withdrawal. https://pmc.ncbi.nlm.nih.gov/articles/PMC10069411/
- Withdrawal Syndromes – StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK459239/
- NCDAS: Substance Abuse and Addiction Statistics. https://drugabusestatistics.org
- Information about Medications for Opioid Use Disorder (MOUD). https://www.fda.gov/drugs/information-drug-class/information-about-medications-opioid-use-disorder-moud
