Key Takeaways: Your Decision Guide
- Prioritize Trauma-Informed Care: Look for programs where staff are trained in de-escalation and emotional safety, as this is critical for women’s inpatient rehab success.
- Verify Accreditation: Ensure the facility is accredited by The Joint Commission to guarantee safety and quality standards.
- Plan for 90 Days: Research indicates that a stay of at least 90 days significantly improves long-term abstinence and family reunification rates.
- Check Integrated Care: Confirm the program treats co-occurring disorders (mental health and substance use) simultaneously for the best outcomes.
Why Women Need Specialized Women’s Inpatient Rehab
Trauma-Informed Care as Foundation
A trauma-informed approach is essential in any women’s inpatient rehab, serving as a foundation for both safety and meaningful healing. Trauma-informed care recognizes that many women entering treatment have experienced significant events such as childhood trauma or intimate partner violence, which can deeply impact recovery journeys.
Programs grounded in this model offer an environment that prioritizes trust, empowerment, and emotional safety—key factors in sustained engagement and positive outcomes. To help you evaluate whether a women’s inpatient rehab truly prioritizes trauma-informed care, consider this quick checklist:
- Are all staff trained in trauma awareness and de-escalation techniques?
- Does the program foster nonjudgmental, supportive interactions?
- Is there flexibility to accommodate individual emotional needs?
- Are group sessions structured to avoid confrontation and promote connection?
- Does the facility offer specialized therapies for trauma, such as EMDR or trauma-focused cognitive behavioral therapy?
Research consistently shows that when women’s specific needs are addressed from the start—including trauma histories—treatment engagement, retention, and recovery outcomes improve dramatically.10
In fact, women-focused programs that emphasize supportive group dynamics lead to better long-term reductions in substance use compared to mixed-gender settings.9 This approach works best when a woman’s sense of safety and agency are central throughout her stay, enabling her to build trust and begin genuine healing. As you continue exploring options, it’s also important to understand how women’s inpatient rehab addresses co-occurring disorders, which often overlap with trauma experiences.
Addressing Co-Occurring Disorders
When considering women’s inpatient rehab, addressing co-occurring disorders—meaning the presence of both substance use and mental health conditions—is essential to long-term wellness. Women in treatment are significantly more likely than men to experience challenges such as depression, anxiety, post-traumatic stress, or eating disorders alongside substance use. Without a coordinated approach, these issues can fuel each other and complicate recovery.
Use this practical tool for assessing a program’s readiness to treat co-occurring disorders:
- Are all clients screened for mental health needs upon admission?
- Does the team include licensed mental health professionals?
- Are integrated treatment plans created for both substance use and mental health?
- Is there access to evidence-based therapies like cognitive behavioral therapy (CBT) or dialectical behavior therapy (DBT)?
- Does aftercare planning include ongoing support for both sets of challenges?
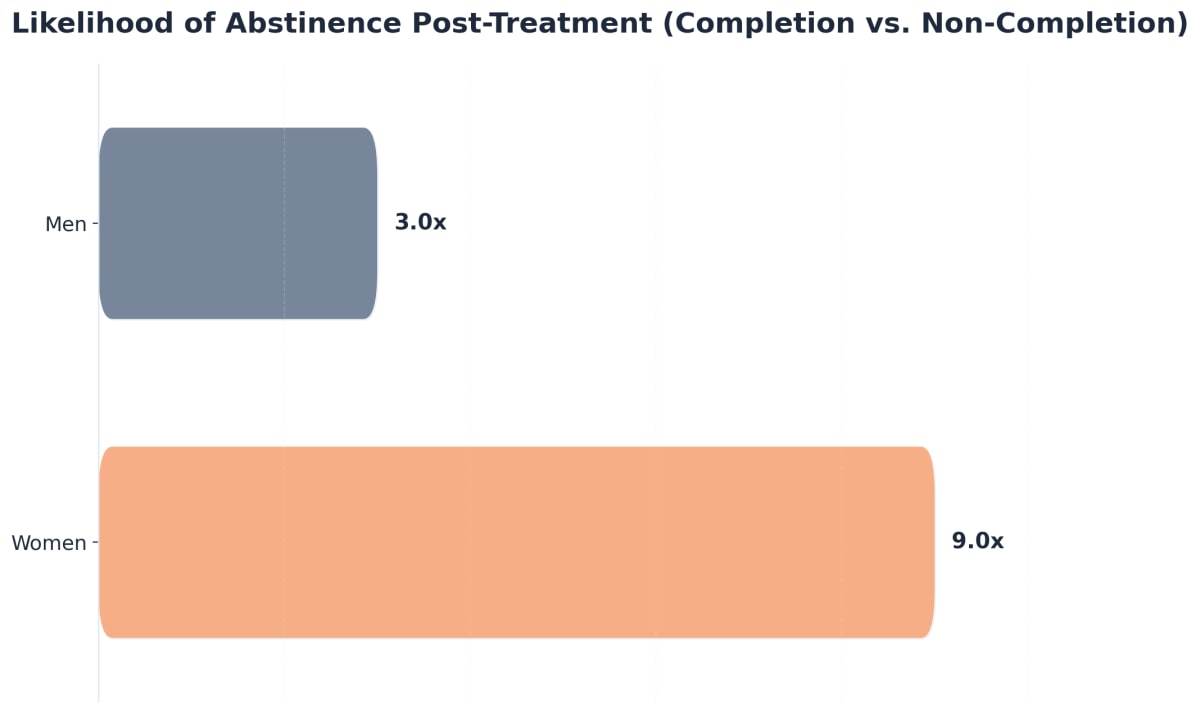
Research shows that integrated care, where substance use and mental health are addressed together, leads to higher engagement and better recovery outcomes for women.10 For example, women who complete at least 90 days of treatment double their chances of family reunification and sustained recovery.3 This approach is ideal for those who recognize symptoms of depression, anxiety, or trauma in addition to substance use concerns. By ensuring a women’s inpatient rehab addresses co-occurring disorders from day one, women build a stronger foundation for lasting change.
Next, it’s helpful to know what program quality and accreditation look like when selecting a treatment center.
Essential Criteria for Women’s Inpatient Rehab Selection
Accreditation and Quality Standards
To ensure the best possible recovery environment, verifying a women’s inpatient rehab facility’s accreditation and quality standards is essential. Accreditation by organizations such as The Joint Commission signals that a program meets rigorous benchmarks for person-centered care, safe rehabilitation practices, and cultural competence with special populations.2
A practical checklist for evaluating accreditation and quality includes:
- Is the facility accredited by The Joint Commission or a similar recognized body?
- Are staff credentials and professional training standards clearly documented?
- Does the program have established policies for client safety, privacy, and rights?
- Are care plans coordinated across medical, psychiatric, and counseling services?
- Is there a process for ongoing quality improvement and feedback from past clients?
Research highlights that accredited women’s inpatient rehab programs are committed to providing safe and effective care, using evidence-based interventions, and maintaining qualified staff.2 Opt for this framework when you want confidence in the facility’s commitment to ethical practices, coordinated treatment, and long-term recovery outcomes. Ensuring accreditation also means the program is evaluated regularly for compliance with ever-evolving standards, giving families and clients peace of mind during a challenging transition.
Next, understanding how well a facility integrates evidence-based therapies will help you assess the overall strength of its treatment model.
Evidence-Based Therapy Integration
When selecting a women’s inpatient rehab, it’s important to ensure the program uses evidence-based therapies—those proven by research to support recovery. Evidence-based therapies include approaches like cognitive behavioral therapy (CBT), motivational interviewing, and trauma-focused interventions. These methods help women build coping skills, process past experiences, and set realistic goals for long-term health.
Programs that prioritize evidence-based care also adapt their approach to address women’s unique needs, such as trauma history, co-occurring mental health conditions, and family responsibilities.10 To evaluate a facility’s integration of evidence-based therapies, use this quick assessment:
- Are clinical staff trained and certified in delivering CBT and other evidence-based modalities?
- Does the program regularly update its treatment protocols to reflect current research?
- Are therapy sessions individualized based on each woman’s personal history and preferences?
- Is progress measured with validated tools and adjusted as needed?
- Does the center offer group therapies designed specifically for women?
This strategy suits organizations that understand the value of tailored, research-backed care. Effective women’s inpatient rehab programs will not only provide these therapies but also demonstrate how they personalize care to support each woman’s journey. Recent research confirms that when women participate in programs with evidence-based therapy integration, they experience higher engagement, retention, and long-term recovery rates.6
Next, reviewing the range of treatment models and approaches will clarify which program best fits your unique needs.
Evaluating Treatment Models and Approaches
Medication-Assisted Treatment Options
Medication-assisted treatment (MAT) is an important option to consider when evaluating a women’s inpatient rehab. MAT combines FDA-approved medications—such as buprenorphine, methadone, or naltrexone—with counseling and behavioral therapies, creating a whole-person approach to substance use disorder treatment. This integrated strategy helps normalize brain chemistry, reduce cravings, and support sustained recovery, particularly for women facing opioid or alcohol use disorders.7
To determine if a women’s inpatient rehab offers robust MAT options, use this practical assessment:
- Are medical providers certified to prescribe and monitor MAT?
- Does the program educate clients on the benefits and risks of each medication?
- Is MAT integrated with trauma-informed counseling and mental health support?
- Are individualized plans developed based on each woman’s clinical needs and preferences?
- Does the facility offer ongoing monitoring and aftercare for those continuing MAT after discharge?
MAT has been shown to increase retention in treatment and decrease the risk of overdose, especially when combined with evidence-based therapy and support groups.8 This approach works best when a woman prefers a medication-supported path or has not responded to abstinence-only models. As you weigh treatment models, knowing how a center supports MAT can help you find a facility that aligns with your recovery goals.
Up next, you’ll learn how holistic and whole-person integration further enhances the effectiveness of treatment.
Holistic and Whole-Person Integration
Holistic and whole-person integration in women’s inpatient rehab is about supporting every aspect of a woman’s wellbeing—physical, emotional, mental, and social. The most effective programs move beyond symptom management by weaving together therapies that reflect this multidimensional view of recovery.
Here’s a quick assessment tool to help you evaluate holistic integration:
- Are services coordinated for medical, mental health, nutritional, and wellness needs?
- Does the program offer complementary therapies such as yoga, meditation, or expressive arts?
- Are family and social supports engaged in treatment planning?
- Is there a focus on building life skills, such as stress management and communication?
- Does aftercare include ongoing support for wellness and relapse prevention?
Research highlights that addressing the full spectrum of a woman’s life circumstances—trauma history, parenting roles, social networks, and physical health—leads to better engagement and more sustainable recovery outcomes in women’s inpatient rehab.10 For example, programs that combine traditional counseling with stress reduction, peer support, and healthy lifestyle coaching are especially effective for women balancing family and work demands.
This solution fits individuals who want to rebuild not just sobriety, but also self-esteem, relationships, and overall quality of life. By seeking a facility that truly embraces holistic and whole-person integration, women can nurture strengths that last well beyond discharge.
Next, understanding insurance coverage and barriers to access will ensure you can move forward with confidence.
Navigating Insurance and Access Barriers
Finding the right treatment often depends on understanding what insurance coverage is available and how to access the care needed. Many people face confusion about which services their plans cover, what facilities accept their insurance, and how to navigate pre-authorization requirements. These administrative hurdles can feel overwhelming, especially when someone is ready to seek help and wants to move forward quickly. The frustration of encountering bureaucratic obstacles at such a vulnerable moment adds an emotional burden to an already challenging situation.

Insurance coverage for substance use treatment varies significantly depending on the type of plan, the provider network, and the specific services required. Most private insurance plans cover some level of treatment, including detoxification, residential programs, outpatient therapy, and medication-assisted treatment, typically covering 60-80% of treatment costs after the deductible is met.
However, the extent of coverage and out-of-pocket costs can differ substantially. Some plans require pre-authorization before treatment begins, which means the insurance company must approve the services in advance—a process that typically involves a 24-48 hour review period where the insurer evaluates medical necessity documentation submitted by the treatment facility.
According to recent data, approximately 85% of private insurance plans now include some form of substance use disorder coverage, though the specific benefits vary widely.
To help you visualize the potential financial landscape, the table below outlines common coverage scenarios for women’s inpatient rehab:
| Coverage Type | Typical Coverage Level | Common Requirements |
|---|---|---|
| In-Network PPO | 80-100% after deductible | Pre-authorization, Medical Necessity Review |
| Out-of-Network PPO | 50-70% after deductible | Higher deductibles, Upfront payment often required |
| HMO Plans | 100% (In-network only) | Strict referral process, No out-of-network coverage |
| Medicaid/State | 100% (Approved facilities) | Waitlists common, Limited facility choice |
Understanding insurance benefits requires asking specific questions about coverage limits, network providers, and any requirements for continued care. Many treatment facilities have admissions coordinators who can verify insurance benefits and explain what costs the plan will cover. These professionals serve as valuable resources, helping to clarify confusing policy language and identify potential financial responsibilities before treatment starts.
For those without insurance or with limited coverage, alternative pathways to treatment exist. State-funded programs, community health centers, and nonprofit organizations often provide services on a sliding fee scale based on income. Some facilities offer payment plans or financial assistance programs for individuals who qualify. Medicaid expansion in many states has also increased access to substance use treatment services for eligible individuals.
Geographic location can present additional access barriers. Rural areas often have fewer treatment facilities, longer waitlists, and limited transportation options. Telehealth services have expanded significantly in recent years, offering virtual counseling, medication management, and support group participation. These remote options help bridge geographic gaps and provide flexibility for people balancing treatment with work or family responsibilities.
Waitlists at quality treatment facilities can extend for weeks or months, creating risk during a critical window when someone is ready for help. During waiting periods, connecting with support groups, establishing care with a primary care physician, or beginning outpatient counseling can provide interim support. Some facilities maintain cancellation lists that allow for earlier admission when openings become available unexpectedly.
Navigating these systems requires persistence and advocacy. Family members, healthcare providers, and patient advocates can assist in identifying resources, understanding insurance benefits, and overcoming logistical challenges. The effort invested in understanding coverage options and access pathways ultimately leads to more informed decisions about treatment and better preparation for the recovery journey ahead.
Frequently Asked Questions
How long should I plan to stay in a women’s inpatient rehab program?
The recommended length of stay in a women’s inpatient rehab program often ranges from 30 to 90 days, with research showing the strongest long-term outcomes for women who complete at least 90 days of treatment 3. Longer stays are linked to higher rates of abstinence and double the likelihood of family reunification, compared to shorter programs 3. However, the ideal duration depends on individual needs, co-occurring mental health conditions, and personal recovery goals. Clinical teams typically reassess progress and adjust the length of stay to support the best possible outcomes for each woman. Many programs offer step-down options, such as outpatient care, to help sustain recovery after discharge.
Can I bring my children with me to a women’s inpatient rehab?
Some women’s inpatient rehab programs do allow mothers to bring their children, but policies vary widely between facilities. Programs that accommodate children typically offer on-site childcare, family housing, or parenting support to help women focus on recovery while maintaining their parental responsibilities. However, space and resources can be limited, and certain programs may restrict children’s ages or require additional screening for safety and suitability. Research highlights that lack of childcare and fear of family separation are major barriers preventing many women from seeking treatment 4. If bringing your child is essential, ask the admissions team about specific arrangements and available support services before enrolling in a women’s inpatient rehab.
What happens if I need to leave treatment early for a family emergency?
If you need to leave a women’s inpatient rehab program early due to a family emergency, the care team will work closely with you to support a safe transition. Most facilities prioritize your wellbeing by creating an individualized discharge plan, connecting you with outpatient resources or telehealth counseling for continued care, and providing relapse prevention strategies. This approach helps minimize disruption and encourages ongoing engagement in recovery, even when life circumstances require a pause in residential treatment 10. If possible, communicate your needs with staff as early as you can—many programs are experienced in helping women navigate unexpected challenges and can offer guidance on returning to treatment when you’re ready.
Will my insurance cover the full duration of women’s inpatient rehab treatment?
Insurance coverage for the full duration of women’s inpatient rehab treatment depends on your specific plan and whether the care is deemed medically necessary. Federal and state regulations require most insurance policies to cover inpatient substance use disorder treatment on par with medical and surgical care, meaning insurers typically cannot deny coverage or charge higher premiums solely because of a substance use disorder diagnosis 5. However, approval for extended stays often requires documentation of ongoing medical necessity, and some plans may have limits or require periodic reviews. To avoid gaps in coverage, contact your insurer and the admissions team at your chosen women’s inpatient rehab to clarify authorization processes and any documentation requirements.
How do women-only programs differ from mixed-gender treatment settings?
Women-only programs in women’s inpatient rehab are designed to create a safe, supportive environment where women can address sensitive issues—such as trauma, relationships, and motherhood—without the presence of men. These settings typically foster open communication, trust, and shared understanding among peers with similar experiences. Research shows that while both women-only and mixed-gender treatment can be effective during the program itself, women-focused groups often lead to greater long-term reductions in substance use and higher satisfaction at follow-up 9. This difference is especially meaningful for women with trauma histories or those who feel more comfortable discussing personal topics in a single-gender setting. Mixed-gender settings may work well for individuals who prefer a broader social dynamic, but women’s inpatient rehab programs offer unique benefits tailored to women’s needs.
What support is available after completing a women’s inpatient rehab program?
After completing a women’s inpatient rehab program, ongoing support is available to help women maintain recovery and navigate daily life. Most programs provide a personalized aftercare plan, which may include outpatient therapy, support groups such as 12-step or women-focused meetings, and access to case management services for help with employment or housing. Participation in mutual-help groups and continued therapy are strong predictors of lasting recovery for women 4. Some treatment centers, including Ripple Ranch Recovery Center and Continuum Outpatient Center, offer alumni programs, telehealth check-ins, and family support to ease the transition back to home and community. These ongoing connections help reinforce coping skills and provide encouragement when challenges arise.
How can I verify that a women’s inpatient rehab facility is properly licensed and accredited?
To confirm that a women’s inpatient rehab facility is properly licensed and accredited, start by asking the admissions team for proof of state licensing and accreditation by organizations like The Joint Commission. Accredited programs must meet strict standards for safety, staff qualifications, and quality of care, with regular onsite surveys to ensure ongoing compliance 2. You can also verify accreditation status through The Joint Commission’s online directory or your state’s health department website. Choosing a licensed and accredited women’s inpatient rehab provides added assurance of ethical practices, effective treatment, and protection of your rights as a client.
Your Path Forward: Taking the First Step
While insurance and access considerations are important, they shouldn’t delay the decision to seek help. Recovery from substance use disorder begins with a single, courageous decision. While the journey may feel overwhelming, people from all walks of life successfully navigate this path every day, finding healing and rebuilding their lives.
Starting the conversation with a treatment provider can provide clarity about available options and help determine the most appropriate level of care. Many facilities offer free assessments to evaluate individual needs and discuss personalized treatment approaches. These initial consultations create opportunities to ask questions, address concerns, and understand what to expect throughout the recovery process.
For those supporting a loved one struggling with substance use disorder, approaching the conversation with compassion and preparation makes a significant difference. Resources like intervention specialists can guide families through this sensitive process, helping create supportive environments that encourage treatment acceptance.
Whether seeking help for oneself or a family member, reaching out represents an act of strength, not weakness. Despite the barriers that may exist, resources are available to help navigate insurance questions, financial concerns, and access challenges. Treatment programs across the country stand ready to provide evidence-based care tailored to individual circumstances. The first step—calling SAMHSA’s National Helpline at 1-800-662-4357 for free, confidential guidance 24/7, or completing an online inquiry with a treatment provider—opens the door to comprehensive support and lasting transformation.
References
- SAMHSA – Substance Abuse and Mental Health Services Administration. https://www.samhsa.gov
- Behavioral Health Care & Human Services Accreditation Program. https://www.jointcommission.org/en-us/accreditation/behavioral-health-care-and-human-services
- Gender and Use of Substance Abuse Treatment Services – PMC – NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC6470905/
- Barriers to Accessing Addiction Treatment for Women at Risk – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC8893170/
- Mental Health and Substance Use Disorder Coverage – NY DFS. https://www.dfs.ny.gov/consumers/health_insurance/new_york_health_insurance_policies__programs/mh_sud
- Addiction Treatment Methods | Evidence-Based Practices. https://www.naatp.org/treatment-methods-evidence-based-practices
- Substance Use Disorder Treatment Options – SAMHSA. https://www.samhsa.gov/substance-use/treatment/options
- Information about Medications for Opioid Use Disorder (MOUD). https://www.fda.gov/drugs/information-drug-class/information-about-medications-opioid-use-disorder-moud
- The Women’s Recovery Group Study – Stage I trial. https://pmc.ncbi.nlm.nih.gov/articles/PMC3679366/
- TIP 51 Substance Abuse Treatment: Addressing the Specific Needs of Women. https://library.samhsa.gov/sites/default/files/sma15-4426.pdf
