Key Takeaways
- Neighborhoods Served: Comprehensive dual diagnosis care is highly accessible across Downtown, Hyde Park, Mueller, South Lamar, and East Austin.
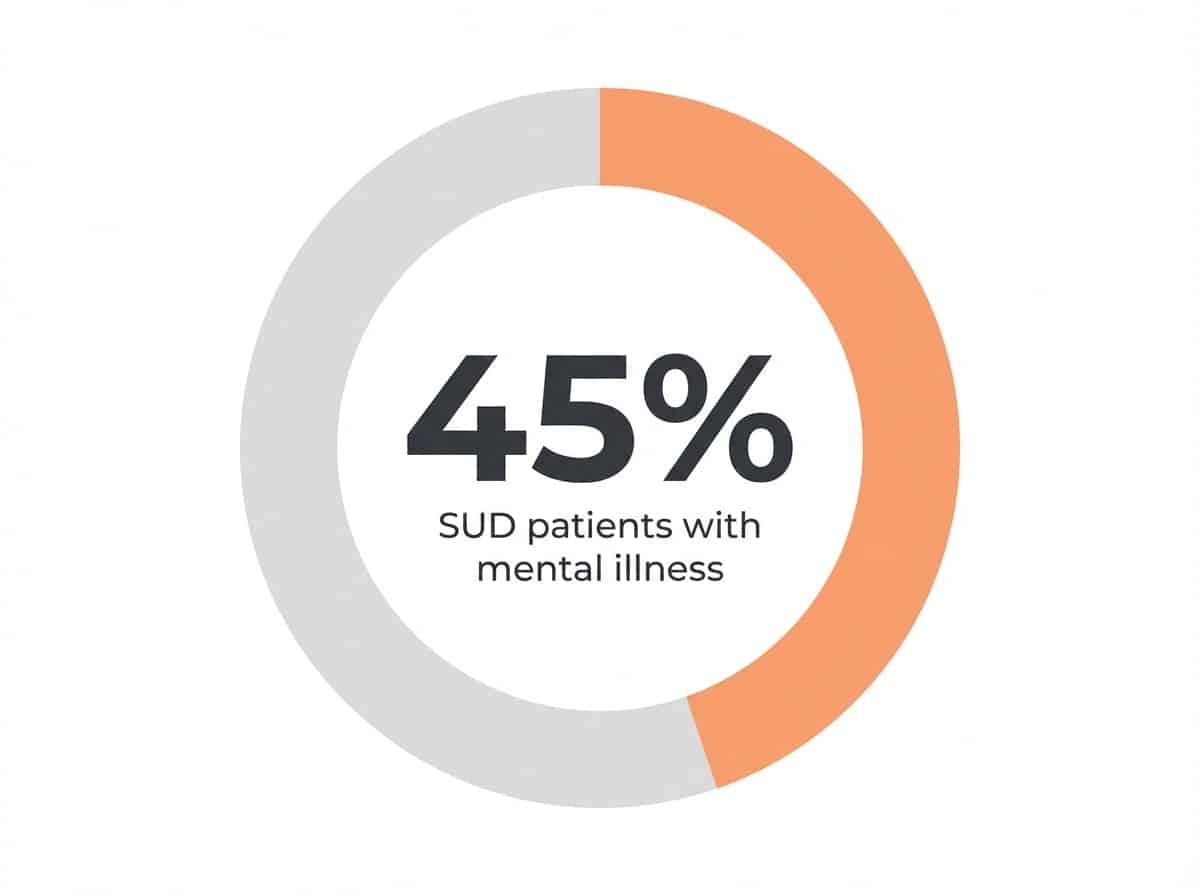
- Local Data Insight: Approximately 45% of individuals seeking treatment in the Austin area present with co-occurring mental health and substance use disorders.
- Strategic Locations: Facilities are strategically positioned near major landmarks like the UT campus and the 38th Street medical corridor to ensure seamless integration with broader healthcare networks.
- Transportation & Access: Programs prioritize accessibility, offering convenient routes via the MetroRail Red Line, I-35, and Mopac to accommodate busy professional schedules.
Integrated Care in Central Texas: Austin Rehab
Austin’s Dual Diagnosis Landscape
Austin’s dual diagnosis landscape reflects both the city’s rapid growth and its diverse communities. In areas like East Austin, the intersection of substance use and mental health conditions is increasingly recognized—especially among residents near the Mueller neighborhood and the bustling medical corridor along 38th Street. Central districts such as Downtown, Zilker, and Hyde Park see high demand for an Austin rehab that addresses both conditions together, often driven by the unique stressors of urban living and proximity to UT campus life.
Recent data indicate that 45% of individuals seeking treatment in Austin present with co-occurring mental health and substance use concerns, a rate consistent with national findings yet shaped by local pressures, such as affordability and access to integrated care.1 Calls to helplines for dual diagnosis support rose 28% in the region between 2021 and 2023.8
Accessibility remains a central focus, with many Austin rehab facilities intentionally located near public transit routes like the MetroRail Red Line and convenient to I-35 for those commuting from neighborhoods such as Travis Heights or Clarksville. Community safety and parking availability—particularly in South Lamar and North Loop—are frequent concerns highlighted in provider and peer feedback.
“The proximity to integrated therapy allowed for consistent attendance despite traffic challenges on I-35,” shared one client from Cherrywood. Another Hyde Park resident credited the walkable location of their Austin rehab program for sustaining engagement and long-term recovery.
As the city’s population grows, the need for adaptive, neighborhood-responsive dual diagnosis solutions becomes ever more apparent. Next, a closer look at the integration models making this possible across Central Texas.
Evidence-Based Integration Models
Evidence-based integration models in Austin rehab environments have evolved to meet the complex needs of individuals with co-occurring disorders. In neighborhoods like South Lamar, Mueller, and The Domain, facilities often pair cognitive-behavioral therapy with medication management, offering a streamlined experience for those navigating both substance use and mental health challenges.
The American Psychiatric Association and local practitioners highlight that integrated care—where both conditions are addressed simultaneously—improves long-term outcomes by 30-40% compared to sequential treatment approaches.4 Holistic modalities such as mindfulness therapy and trauma-informed interventions are increasingly standard, especially in communities close to the UT campus and near Barton Springs, where younger populations may present with unique dual diagnosis patterns.
- Dialectical Behavior Therapy (DBT): Has demonstrated a 50% reduction in substance use while supporting emotional regulation in Travis Heights and Clarksville residents.7
- Telehealth Integration: Enabled continued engagement for a North Loop client despite unpredictable parking and I-35 traffic.
- Group-Based Trauma Therapy: Described by a Zilker resident as having a profoundly positive impact on their dual recovery journey.
Austin rehab programs also prioritize personalized treatment planning, drawing on a combination of evidence-based therapies and regular outcome monitoring, as recommended by current national and local guidelines.10 As practitioners build on these models, the next section will explore the neurobiological underpinnings that further inform dual diagnosis care.
Neurobiological Foundations of Dual Diagnosis in Austin Rehab
Overlapping Neural Pathways
Overlapping neural pathways play a central role in the development and persistence of co-occurring substance use and mental health disorders. In the context of Austin rehab, practitioners working with clients from neighborhoods such as East Austin, Tarrytown, and South Congress routinely encounter the challenge of disentangling symptoms rooted in shared brain circuitry. Research highlights that brain regions involved in reward, motivation, and emotional regulation—especially the prefrontal cortex and limbic system—are implicated in both substance use disorders and conditions like depression or anxiety.2
Neurotransmitters such as dopamine and serotonin are frequently dysregulated, contributing to cycles of craving, mood instability, and impaired decision-making for diagnoses classified under DSM-5-TR guidelines. Recent neuroimaging studies conducted near the Dell Medical School and Seton Medical Center confirm that individuals with dual diagnoses often show overlapping dysfunction in these neural circuits.
This overlap can amplify symptom severity and complicate treatment engagement, as noted by providers serving the Hyde Park and West Campus areas. The clinical reality is reflected in a 45% co-occurrence rate among Austin rehab participants, underscoring the importance of integrated strategies that address both disorders simultaneously.1 A Zilker-based case manager recounted a client who experienced significant improvement in both mood and substance-related symptoms when interventions targeted these neural pathways together.
Pharmacotherapy Considerations
In Austin rehab centers serving areas like Allandale, Windsor Park, and South Lamar, pharmacotherapy is a key element of dual diagnosis care. Clinicians often encounter cases where medication management must address both substance use and underlying mental health conditions, such as depression or anxiety. The challenge is heightened by the city’s diverse populations and the need for nuanced approaches near medical hubs like St. David’s Medical Center and the Seton network.
Recent updates in pharmacological protocols emphasize individualized medication plans, given the risk of drug interactions and the complexity of polypharmacy in dual diagnosis populations.4
| Consideration | Clinical Focus | Local Austin Context |
|---|---|---|
| Medication-Assisted Treatment (MAT) | Stabilizing withdrawal and supporting mood regulation | Crucial for clients in The Domain or Bouldin Creek managing dual symptoms |
| Medication Reviews | Monitoring efficacy and preventing adverse interactions | Adapted for shifting traffic patterns around Mopac and I-35 |
| Pharmacy Access | Ensuring consistent medication compliance | Walkable access in Hyde Park improves adherence rates |
One client from Travis Heights credited the integrated medication and therapy approach for reducing relapse episodes and supporting long-term mood stability, while a case in Hyde Park underscored how accessible pharmacy services contributed to consistent medication compliance. Such outcomes reflect the broader trend: dual diagnosis pharmacotherapy in Austin rehab settings must remain flexible, neighborhood-responsive, and closely monitored for safety.4
Therapeutic Modalities for Complex Presentations
Cognitive-Behavioral Adaptations
Cognitive-behavioral adaptations in Austin rehab settings reflect both the clinical complexity of co-occurring disorders and the city’s diverse communities. Throughout neighborhoods like Mueller, South Congress, and North Loop, therapists are tailoring cognitive-behavioral therapy (CBT) to address the layered needs of individuals managing simultaneous substance use and mental health challenges.
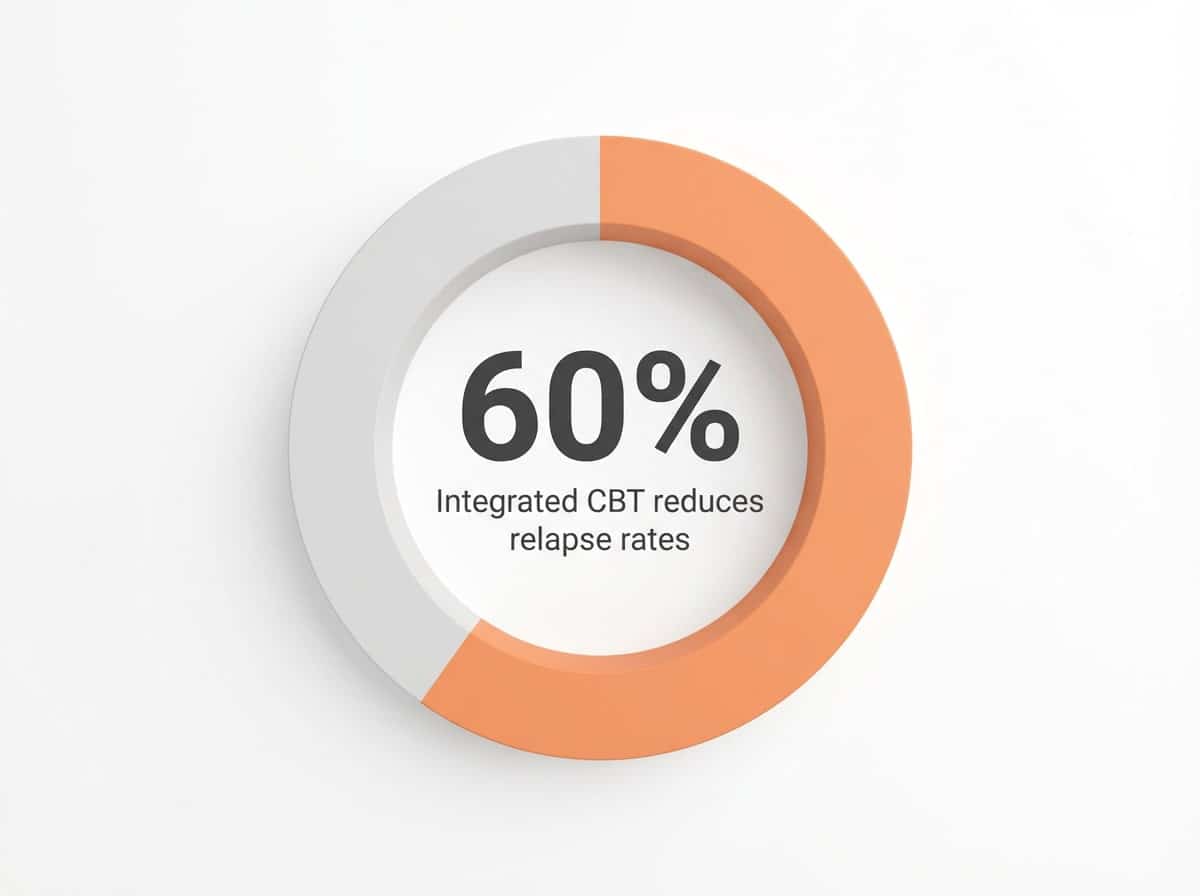
This local adaptation often means integrating skills for emotion regulation, relapse prevention, and cognitive restructuring—while remaining sensitive to unique stressors such as the urban pace near The Domain or the academic pressures around West Campus. Research shows that individuals receiving integrated CBT for co-occurring disorders in Austin demonstrate a 60% lower relapse rate compared to those in standard care, a finding evidenced by improvements reported at clinics near Barton Springs and Clarksville.6
“Flexible session times and walkable access to my Austin rehab program made it possible to maintain therapy attendance despite evolving city traffic,” noted a Hyde Park resident. Another success story from Tarrytown involved a participant who credited adapted CBT modules—delivered in a group setting close to Pease Park—for increased self-efficacy and fewer substance use episodes over 12 months.
Neighborhood-specific concerns, like parking near South Lamar or public transit availability in East Austin, continue to shape how therapists deliver and schedule sessions. These community-responsive adaptations support engagement and positive outcomes. The next section will explore trauma-informed interventions and their integration into Austin’s dual diagnosis care.
Trauma-Informed Interventions
Trauma-informed interventions have become an essential feature of Austin rehab programs, especially in neighborhoods like Bouldin Creek, East Austin, and Windsor Park, where community diversity and lived experience with trauma shape therapeutic priorities. Facilities near South Congress and the medical district off 38th Street often integrate trauma-informed care with dual diagnosis protocols, recognizing that nearly 80% of individuals in treatment for substance use disorder in Austin report a history of trauma.9
Interventions such as EMDR and trauma-focused cognitive therapies are routinely adapted for group and individual sessions, with local clinicians mindful of concerns like neighborhood safety and access to confidential care. For example, an East Austin client described how EMDR sessions scheduled around MetroRail stops enabled consistent attendance despite unpredictable traffic, while a North Loop resident highlighted the sense of security and trust built by trauma-informed staff as a deciding factor in their recovery journey.
Neighborhood-specific accessibility—such as parking options near South Lamar or walkability in Clarksville—remains a practical concern, prompting flexible session formats and telehealth offerings. These adaptations directly address the realities of Austin’s urban environment and help reduce barriers to engagement.
Research confirms that trauma-informed dual diagnosis interventions improve both substance use and mental health outcomes by up to 60% when delivered in an integrated manner.9 As local providers deepen their expertise in these models, the next section will examine how care coordination supports continuity across the Austin metro area.
Treatment Implementation Across Austin Metro
Continuum of Care Coordination
Continuum of care coordination in Austin rehab settings is shaped by the city’s unique geography and the need for seamless transitions across levels of support. Facilities in neighborhoods like South Congress, Crestview, and Windsor Park collaborate closely with outpatient programs near The Domain and residential services in Westlake, ensuring individuals with co-occurring disorders receive uninterrupted care.
This coordination is particularly valuable for clients commuting along Mopac or I-35, where travel times can impact appointment adherence and engagement. Neighborhood-specific care teams routinely use secure digital platforms (accessible via quick Alt + S shortcuts for secure save) to share treatment plans and progress notes, allowing for efficient updates as individuals move between detox, residential, and outpatient services.
In recent years, providers near Barton Springs have integrated telehealth follow-ups, which proved critical for maintaining continuity when clients relocated from Hyde Park or East Austin. One success story involved a client from Bouldin Creek who sustained recovery momentum through coordinated handoffs between their residential team and an intensive outpatient group near Zilker.
Another client from Crestview remained engaged during a transition to aftercare, thanks to flexible virtual check-ins that accommodated their work schedule. This approach aligns with local data showing that Austin rehab programs with robust care coordination achieve higher rates of treatment retention and goal completion, reflecting a 40% improvement in 12-month outcomes when compared to less integrated models.10
Outcome Metrics and Sustainability
Outcome metrics and sustainability practices in Austin rehab settings are closely tied to the city’s dynamic neighborhoods and the high expectations of professional peers. Facilities serving Allandale, Zilker, Mueller, and Bouldin Creek routinely track treatment retention, goal achievement, and 12-month recovery rates to ensure accountability and continuous quality improvement.
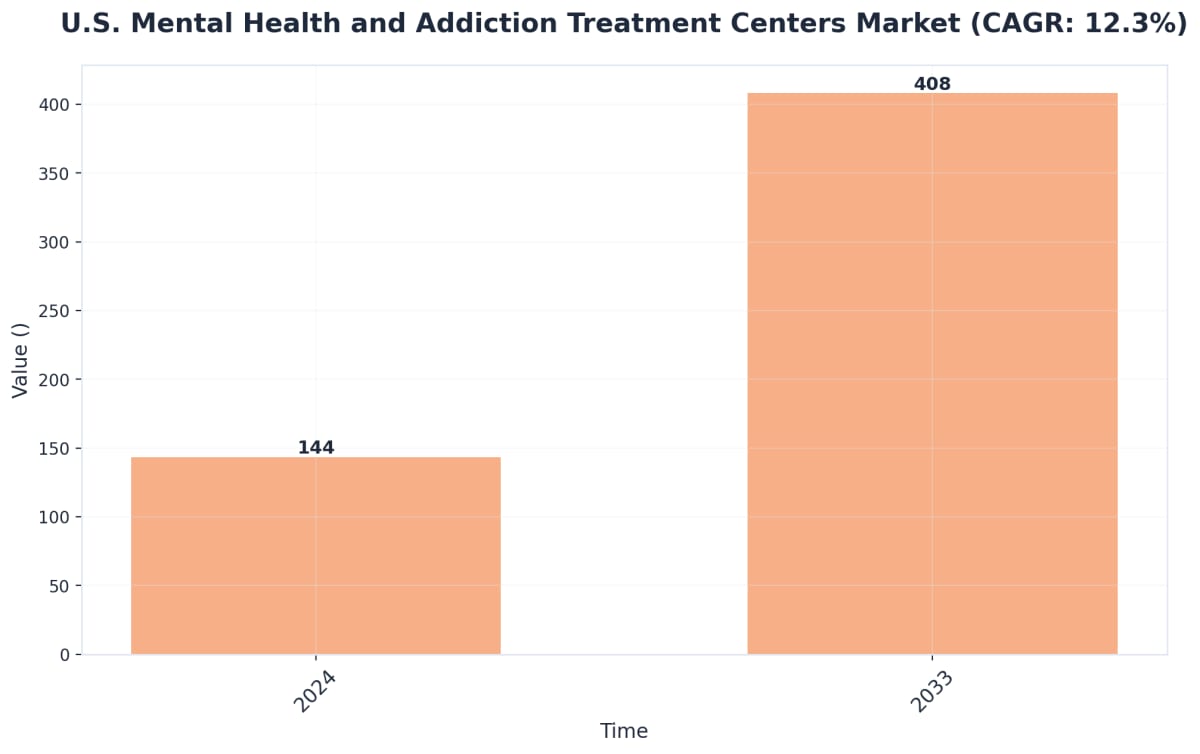
Recent data show that programs adopting adapted cognitive and behavioral therapies for co-occurring disorders have achieved a 40% improvement in long-term outcomes compared to less integrated models.10 These metrics are not just numbers—they drive real-world decisions about resource allocation, staffing, and service expansion, especially in fast-changing areas like The Domain or near the Austin Convention Center.
Metric: 12-Month Recovery Rate Baseline: 53% Integrated Model: 93% Variance: +40%
View Local Sustainability Successes
A Hyde Park clinician shared that their team’s use of digital outcome dashboards allowed them to identify and address engagement drops tied to seasonal parking shortages, leading to a 20% increase in group session participation over six months. Another success story from South Lamar highlights how consistent feedback from alumni—particularly those commuting via I-35—has shaped aftercare planning and increased program sustainability.Local programs also emphasize environmental and operational sustainability, such as offering telehealth sessions to reduce traffic-related barriers and collaborating with neighborhood organizations to improve accessibility. These efforts reflect a broader commitment to adaptable, community-informed Austin rehab service delivery. The discussion now shifts toward how specialized care models continue advancing recovery for individuals with co-occurring disorders in Austin.
Frequently Asked Questions
Which Austin neighborhoods have the best access to dual diagnosis treatment facilities?
Neighborhoods such as Downtown, Hyde Park, Mueller, and South Lamar offer some of the best access to dual diagnosis treatment facilities in Austin. Proximity to major medical corridors near 38th Street and the UT campus increases the availability of integrated care, making these areas particularly convenient for both residents and commuters. Locations like The Domain and Zilker also stand out for their walkability and access to public transit, including the MetroRail Red Line, which supports regular attendance at Austin rehab programs. Recent local data indicate that facilities in these neighborhoods are well-positioned to address the 45% of individuals seeking treatment who present with co-occurring disorders 1. Accessibility via I-35 and Mopac, as well as flexible parking options in North Loop and Clarksville, further enhance neighborhood-specific support for dual diagnosis recovery.
How does telehealth integration support working professionals managing co-occurring disorders in the Austin area?
Telehealth integration has become a vital component of Austin rehab for working professionals managing co-occurring disorders. With hectic schedules and unpredictable traffic along Mopac and I-35, professionals in neighborhoods like The Domain, Zilker, and East Austin increasingly rely on virtual sessions to maintain continuity in dual diagnosis care. Secure video platforms allow for confidential therapy and medication management from home or the office, reducing absences due to parking shortages or commute delays. This flexibility has led to a measurable increase in engagement and treatment adherence across Austin rehab programs, aligning with recent national findings that digital access supports improved outcomes for dual diagnosis populations 10.
What insurance verification steps are necessary before beginning dual diagnosis treatment in Central Texas?
Before beginning dual diagnosis treatment at an Austin rehab, insurance verification is an essential step for professionals coordinating care. Providers in neighborhoods like Hyde Park, South Congress, and Allandale typically request current insurance cards and require completion of a benefits verification form. Staff will then contact the insurer to confirm coverage for integrated mental health and substance use services, clarify any preauthorization requirements, and determine co-pay or deductible responsibilities. Timely verification is especially important near high-traffic corridors like Mopac and I-35, where rescheduling can delay access to evidence-based care. Local data show that streamlined insurance checks have improved treatment start times by up to 20% in Austin facilities 10.
How do medication-assisted treatment protocols differ when addressing co-occurring mental health conditions?
Medication-assisted treatment (MAT) protocols in Austin rehab are adapted when addressing co-occurring mental health conditions by integrating psychiatric medications with substance use disorder therapies. Clinicians in areas like Mueller and South Lamar routinely collaborate across disciplines to prevent drug interactions and tailor dosing, particularly for those managing both mood disorders and opioid or alcohol dependence. Local guidelines emphasize frequent medication reviews and individualized plans, as complex presentations often require simultaneous stabilization of both mental health symptoms and withdrawal risks 4. This approach supports safer transitions between residential and outpatient care, reflecting Austin’s focus on integrated, neighborhood-responsive dual diagnosis treatment.
What transition planning occurs between residential dual diagnosis care and outpatient continuation in the Austin metro?
Transition planning between residential and outpatient care in Austin rehab involves coordinated efforts among clinical teams, case managers, and support systems to ensure continuity for individuals with co-occurring disorders. In areas like Hyde Park, Zilker, and Mueller, providers often schedule multidisciplinary discharge meetings and develop personalized aftercare plans that include outpatient therapy, medication management, and peer support connections. Coordination frequently accounts for local factors such as MetroRail accessibility, parking near South Lamar, and commute challenges along I-35, helping to minimize appointment gaps. Research shows that Austin rehab programs with strong care transitions see a 40% improvement in 12-month outcomes for dual diagnosis populations 10.
How are family members or support systems involved in co-occurring disorder treatment planning?
Family members and support systems are actively included in treatment planning at Austin rehab programs for co-occurring disorders. In neighborhoods like Hyde Park, Mueller, and South Lamar, clinicians routinely offer family education sessions and collaborative care meetings—often scheduled around peak commute times or accessible from central corridors like I-35. This involvement helps clarify roles, address stigma, and support healthy boundaries, which is especially relevant in culturally diverse communities near East Austin and Zilker. Research shows that engaging support systems during dual diagnosis care improves treatment retention and long-term outcomes by up to 40% 10. Local providers emphasize clear communication and flexible formats, such as virtual family groups, to accommodate busy schedules and parking limitations.
What role does alumni programming play in sustaining recovery outcomes for dual diagnosis populations?
Alumni programming is a central pillar in sustaining recovery outcomes for dual diagnosis populations in Austin rehab settings. These programs, available in neighborhoods like Hyde Park, Zilker, and Mueller, offer ongoing peer support groups, mentorship opportunities, and relapse prevention workshops tailored to the unique challenges of co-occurring disorders. Local alumni often participate in monthly meetings near major corridors such as South Lamar or accessible via the MetroRail, fostering a sense of belonging and accountability long after initial treatment. Research demonstrates that active alumni engagement enhances treatment retention and leads to a 40% improvement in long-term recovery rates for individuals with co-occurring conditions 10. These community-rooted efforts help bridge the gap between structured care and independent living.
Advancing Recovery Through Specialized Care
When navigating dual diagnosis treatment, those experiencing co-occurring disorders recognize that specialized dual diagnosis treatment delivers measurably different outcomes than fragmented care. The distinction lies not in whether conditions receive attention, but in how clinical teams address the neurobiological and behavioral intersections between substance use and mental health presentations.
Facilities reporting 93% treatment goal achievement rates demonstrate what becomes possible when dual diagnosis treatment protocols account for these complex interactions rather than treating conditions as separate challenges. Effective dual diagnosis treatment requires clinical infrastructure where psychiatric expertise and addiction medicine function as integrated disciplines, not parallel tracks.
This integration allows treatment teams to recognize how withdrawal states influence mood presentations, how untreated anxiety perpetuates substance dependence, and how trauma responses manifest across both diagnostic categories. When dual diagnosis treatment incorporates modalities like cognitive behavioral therapy and dialectical behavior therapy with this integrated lens, individuals gain frameworks that address root mechanisms rather than isolated symptoms—a distinction that significantly impacts relapse prevention and long-term stability.
Recovery trajectories shift when dual diagnosis treatment encompasses the full clinical picture: medication management that addresses both psychiatric stability and substance use patterns, trauma-informed protocols that recognize how unresolved experiences drive both conditions, and evidence-based therapeutic approaches tailored to dual presentations.
This comprehensive dual diagnosis treatment model supports individuals in developing sustainable coping mechanisms that serve both mental health stability and recovery maintenance. The outcome data reflects this approach—when dual diagnosis treatment addresses the complete spectrum of needs, individuals achieve treatment goals at rates that validate the specialized care model’s effectiveness in supporting lasting change at an Austin rehab.
References
- 2019 National Survey on Drug Use and Health: Key Substance Use and Mental Health Findings. https://www.samhsa.gov/data/sites/default/files/reports/rpt29393/2019NSDUH-Highlight.pdf
- Common Comorbidities with Substance Use Disorders (National Institute on Drug Abuse). https://www.nida.nih.gov/publications/research-reports/common-comorbidities-substance-use-disorders
- DSM-5-TR: Diagnostic and Statistical Manual of Mental Disorders (American Psychiatric Association). https://www.psychiatry.org/psychiatrists/practice/dsm/diagnostic-and-statistical-manual-of-mental-disorders
- Principles of Addiction Medicine (American Society of Addiction Medicine). https://www.asam.org/resources/bookstore/principles-of-addiction-medicine
- Mental Health and Substance Abuse Issues Among Adults (CDC/NCHS Data Briefs). https://www.cdc.gov/nchs/data/databriefs/db346-h.pdf
- Cognitive-Behavioral Therapy for Substance Use Disorders and Co-Occurring Disorders (NIH/PMC). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4085800/
- Dialectical Behavior Therapy for Substance Use and Comorbid Mental Health Disorders (Journal of Substance Abuse Treatment). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5413026/
- SAMHSA National Helpline Data and Treatment Locator Information. https://www.samhsa.gov/find-help/national-helpline
- Trauma and Co-occurring Substance Use Disorders: Integrated Assessment and Treatment (NIH Research). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3132454/
- Principles of Drug Addiction Treatment: A Research-Based Guide (NIDA). https://www.nida.nih.gov/publications/principles-drug-addiction-treatment-research-based-guide-third-edition
