Key Takeaways
- Federal Protections: Laws like MHPAEA and the ACA ensure that insurance plans must cover substance use disorder treatment comparably to medical care.
- Know Your Plan: Review your Summary of Benefits to understand coverage for detox, residential care, and medication-assisted treatment (MAT).
- Match Care Levels: Use the ASAM Criteria to determine if you need outpatient support or 24-hour residential care based on your specific situation.
- Advocate for Yourself: If coverage is denied, you have the right to appeal, and many facilities can assist with the authorization process.
How Insurance Coverage Works for a Rehab That Takes Insurance
Federal Laws That Protect Your Access
Federal protections ensure that individuals seeking a rehab that takes insurance are not left to navigate coverage alone. The Mental Health Parity and Addiction Equity Act (MHPAEA) is a cornerstone law that requires most insurance plans to offer mental health and substance use disorder (SUD) benefits equal to those for medical and surgical care. This means your plan cannot set higher copays or stricter visit limits for addiction care compared to other health conditions.2
The Affordable Care Act (ACA) builds on this by making SUD services an “essential health benefit”—mandating that all marketplace and Medicaid expansion plans must include coverage for addiction treatment. Because of MHPAEA and the ACA, people can seek help at a rehab that takes insurance with greater confidence that necessary services—like detox, counseling, and aftercare—are covered.3
“These laws also protect you from being denied coverage solely because you are seeking help for a substance use concern. However, while federal law sets the foundation, the details of your benefits… will depend on your specific plan and state regulations.”
When you consider a rehab that takes insurance, understanding these federal protections can empower your journey. For example, if you face a denial, you have appeal rights grounded in these laws. Having this legal safety net helps more people access care, addressing the fact that over 95% of those needing addiction treatment never receive it.3
Next, we’ll explore what your insurance plan actually covers and how to interpret those details for your own needs.
What Your Plan Actually Covers
Understanding the scope of your insurance plan is key when considering care at a rehab that takes insurance. Most major insurance providers—such as Aetna, Blue Cross Blue Shield, Cigna, and UnitedHealthcare—include substance use disorder (SUD) treatment as an essential health benefit, as required by federal law. However, the specifics of what your plan actually covers can differ significantly.3
Start by reviewing your plan’s Summary of Benefits and Coverage (SBC). This document outlines what types of addiction care are covered, such as detoxification, inpatient residential treatment, outpatient therapy, and medication-assisted treatment (MAT). Many plans also cover continuing care, which research shows can increase long-term recovery rates by up to 70% at one year compared to only 20% without ongoing support.6
There are a few key questions to ask as you review your insurance:
- Which services are covered (detox, residential, outpatient, MAT, aftercare)?
- What are the requirements for prior authorization or referrals?
- Are there annual or lifetime visit limits?
- Which providers and facilities are considered in-network?
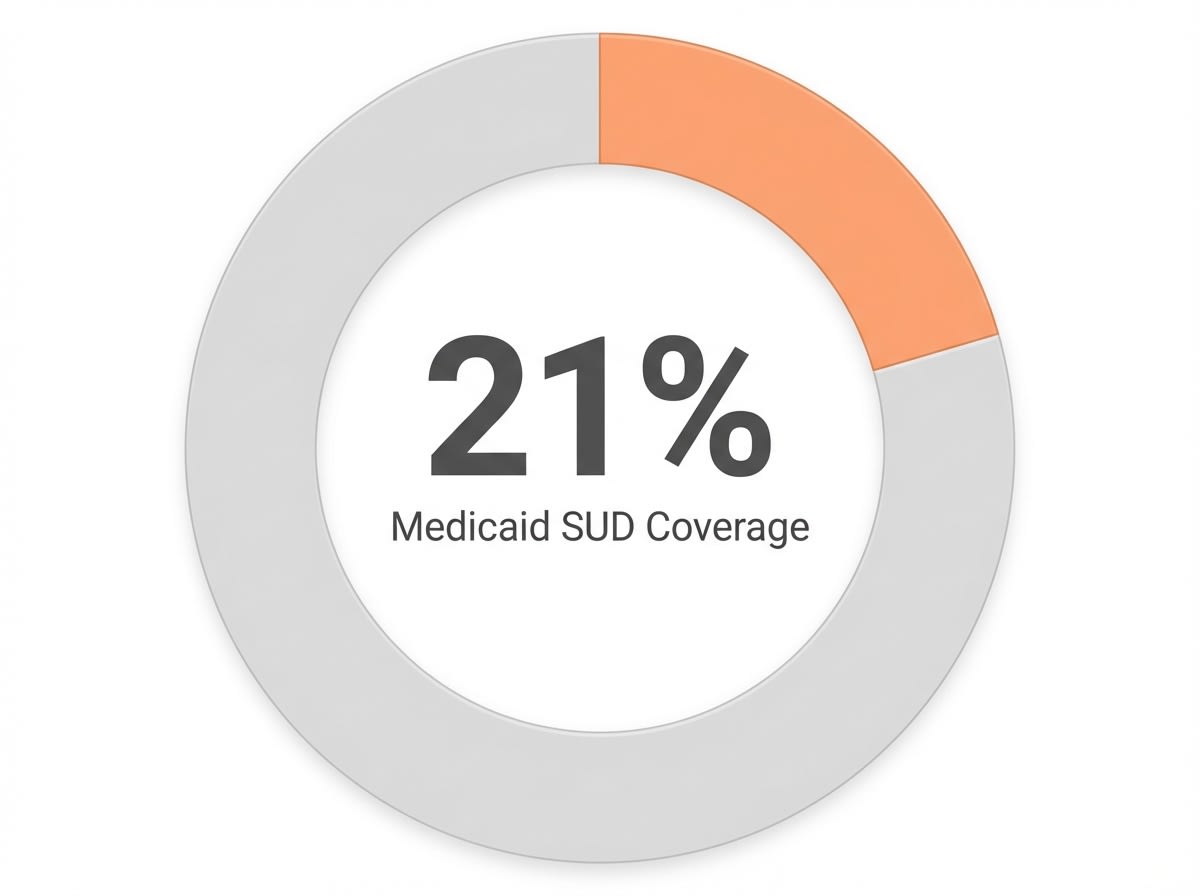
This approach is ideal for individuals who want to maximize their benefits and avoid surprise bills. Remember that some plans require pre-authorization for certain services or may only cover in-network providers, so it’s important to verify these details. If you have Medicaid, know that it covers a broad range of SUD treatments, and 21% of adults covered by Medicaid have a diagnosed substance use disorder.1
Next, we’ll look at how to match the right level of care to your unique needs using nationally recognized criteria.
Matching Your Needs to the Right Level of Care
Understanding ASAM Treatment Levels
To find the most appropriate care at a rehab that takes insurance, it’s helpful to understand the American Society of Addiction Medicine (ASAM) treatment levels. The ASAM Criteria is a nationally recognized system that guides providers and individuals in matching substance use disorder (SUD) severity with the right intensity of support.9
| ASAM Level | Service Type | Description |
|---|---|---|
| Level 1 | Outpatient Services | Typically weekly therapy or counseling sessions. |
| Level 2 | Intensive Outpatient / Partial Hospitalization | Structured programs several days per week, but you return home at night. |
| Level 3 | Residential / Inpatient Services | 24-hour care in a live-in setting for those with greater needs. |
| Level 4 | Medically Managed Intensive Inpatient | Hospital-based care for severe symptoms or medical complications. |
Each level is further tailored using six assessment dimensions, including withdrawal risk, emotional health, readiness to change, and recovery environment. This approach works best when you want treatment that adapts to your changing needs over time, such as stepping up care during crisis or stepping down as you stabilize.9
Most insurance plans use the ASAM Criteria to approve and authorize treatment, so familiarity with these levels can help you communicate effectively with both providers and your insurer. The goal is to ensure you receive the safest and most effective support for your current situation.
Next, discover how to assess your personal needs and start the process of choosing the right starting point on the ASAM continuum.
Self-Assessment: Where Should You Start?
A simple self-assessment can help you determine your best starting point when considering a rehab that takes insurance. Begin by reflecting on a few key questions:
- Have you had difficulty stopping substance use on your own, even after multiple attempts?
- Are you experiencing withdrawal symptoms or health complications when not using?
- Has substance use affected your work, relationships, or safety?
- Do you have a supportive home environment, or do you feel at risk for relapse at home?
If you answer yes to several of these, a higher level of care—such as residential or intensive outpatient—may provide the structure and medical oversight you need. This method works when safety, stability, or physical health are top concerns. If your symptoms are less severe and you have strong support at home, outpatient services might be a good fit.
Research shows that matching treatment intensity to personal needs improves outcomes and helps reduce relapse risk. Keep in mind, over 95% of people who could benefit from addiction care do not receive it, often due to uncertainty about where to start. A rehab that takes insurance will usually guide you through a professional assessment, using tools like the ASAM Criteria, to tailor your care plan.3,9
Next, explore which evidence-based therapies are most often supported by insurance and how they contribute to lasting recovery.
Evidence-Based Therapies a Rehab That Takes Insurance Supports
Medication-Assisted Treatment Effectiveness
Medication-assisted treatment (MAT) is a cornerstone of evidence-based care at any rehab that takes insurance. MAT uses FDA-approved medications like buprenorphine, methadone, and naltrexone, paired with counseling and behavioral therapies, to address opioid and alcohol use disorders. This approach has been shown to significantly improve treatment retention and reduce the risk of overdose.
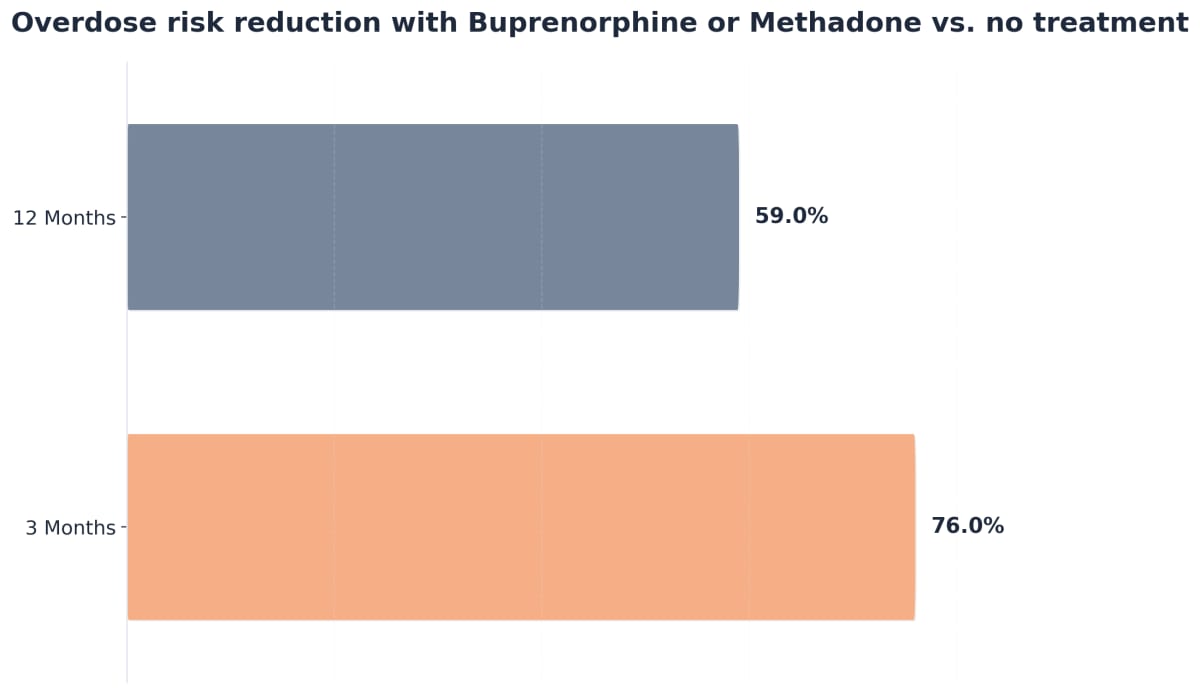
“Research highlights that treatment with buprenorphine or methadone leads to a 76% reduction in overdose risk at three months, and this benefit remains strong at 59% even at twelve months.”4
These medications help manage cravings and withdrawal symptoms, making it more likely for individuals to stay engaged in recovery. Importantly, a rehab that takes insurance can often provide MAT as part of a comprehensive treatment plan, which is especially valuable for people who have experienced repeated relapses or have co-occurring health concerns.
MAT is not a one-size-fits-all solution, but it fits well when someone has not succeeded with abstinence-based programs or needs medical support to stabilize. Recent changes in federal law have also expanded access—more healthcare providers can now prescribe buprenorphine, increasing availability for those seeking help. Opting for MAT through a rehab that takes insurance can offer a safer, more supported path to long-term recovery.4
Next, explore how therapies like Cognitive-Behavioral Therapy and other proven approaches can further strengthen your recovery journey.
Proven Therapeutic Approaches That Work
Many people exploring a rehab that takes insurance benefit most from therapies that have a strong track record for supporting recovery. Among these, Cognitive-Behavioral Therapy (CBT) stands out as one of the most widely researched and effective options. CBT helps people identify unhelpful thought patterns and learn practical skills to manage cravings, reduce stress, and build healthier routines.5,10
| Therapy | Core Focus | Key Outcome |
|---|---|---|
| Cognitive-Behavioral Therapy (CBT) | Identifying unhelpful thought patterns and building practical coping skills. | 58% of patients fare better than those in other treatment conditions. |
| Dialectical Behavior Therapy (DBT) | Mindfulness, emotion regulation, and distress tolerance. | 64% retention rate in treatment compared to 27% with standard care. |
Dialectical Behavior Therapy (DBT) is another evidence-based approach increasingly offered at rehab that takes insurance. DBT combines cognitive-behavioral techniques with mindfulness and emotion regulation strategies. This method is particularly helpful for those dealing with intense emotions, self-harm urges, or co-occurring mental health challenges.
These therapies are most effective when tailored to individual needs and delivered by experienced clinicians. Many insurance plans now recognize their value and routinely cover CBT and DBT as part of a complete care plan at rehab that takes insurance.
Next, discover how to navigate barriers—such as stigma or insurance authorizations—so you can access the care you deserve.
Navigating Barriers to Insurance-Covered Care
Overcoming Stigma and Authorization Hurdles
Facing stigma and insurance authorization requirements can be two of the toughest barriers for those seeking care at a rehab that takes insurance. While insurance coverage opens the door to treatment, nearly 10.4% of people who need help never reach out because they fear judgment from their communities or even their own support networks. This stigma often stems from widespread misconceptions about substance use disorder, making many people worry about being treated differently or losing privacy.8
You can take practical steps to protect yourself and advocate for your needs:
- Know Your Privacy Rights: Federal laws like HIPAA safeguard your health information.
- Ask Questions: When talking to your insurer or a treatment provider, you have the right to ask how your privacy will be maintained.
- Enlist Support: Bring a trusted friend or advocate into discussions with insurance companies, especially when tackling prior authorization forms or appeals.
When it comes to navigating insurance authorizations, persistence pays off. Many people feel discouraged if their first request for coverage is delayed or denied, but federal parity laws require insurers to treat substance use disorder care the same as other medical conditions. If you receive a denial, you can appeal, and many rehab that takes insurance programs will help guide you through this process.2
By addressing stigma and understanding your rights, you can move forward with more confidence. Next, let’s look at how to evaluate and choose the most effective treatment center for your needs.
Evaluating Treatment Centers Effectively
When evaluating a rehab that takes insurance, it helps to use a structured approach to ensure the center aligns with your recovery needs and insurance requirements. Start by creating a checklist that includes:
- Confirmation of in-network status.
- Availability of evidence-based therapies (MAT, CBT, DBT).
- Staff qualifications and facility accreditation.
- Support for co-occurring mental health conditions.
According to research, about 45% of adults with substance use disorder also have a mental health diagnosis, highlighting the importance of integrated care. Ask each rehab that takes insurance about their continuing care services, since ongoing support can increase one-year abstinence rates from 20% to 70%.6,7
Request to review sample schedules and therapy options to make sure the center’s offerings are a good fit for your goals. It’s also helpful to inquire how the facility helps with insurance authorizations or appeals. This strategy suits people who value transparency and wish to minimize surprises during treatment. Finally, consider visiting the facility or speaking with alumni—firsthand accounts provide valuable insights that brochures cannot. By carefully comparing these factors, you can confidently choose a rehab that takes insurance that supports your unique journey.
Up next, get answers to common questions about insurance approvals, switching care levels, and protecting your privacy.
Frequently Asked Questions
What happens if my insurance denies authorization for San Antonio rehab that takes insurance?
If your insurance denies authorization for a San Antonio rehab that takes insurance, you still have a path forward. Federal parity laws require insurers to treat substance use disorder care the same as any other medical condition, giving you the right to appeal a denial. Start by requesting a written explanation of the denial from your insurance company and review it with the rehab that takes insurance staff, who often help with the appeals process. Persistence is key—many approvals are granted after a first appeal. If needed, enlist a trusted advocate to help communicate with your insurer. Your determination can make a difference in accessing the care you deserve.2
Can I switch between levels of care at a San Antonio rehab that takes insurance without restarting the approval process?
Yes, in many cases, you can transition between levels of care at a San Antonio rehab that takes insurance without having to restart the entire approval process. Most insurance companies use the ASAM Criteria to determine medical necessity for each level—so if your clinical needs change, your care team can submit updated documentation to request a shift in your treatment intensity. This process is designed to support continuity and ensure you receive the right care at the right time. While an additional review may be required, you typically won’t need to start from scratch. Always check with your provider for specifics about your plan.9
How do I verify if a San Antonio rehab that takes insurance also treats co-occurring mental health conditions?
To verify if a San Antonio rehab that takes insurance also treats co-occurring mental health conditions, start by asking the facility about their approach to integrated care. Look for programs that mention dual diagnosis or integrated treatment, as about 45% of people with a substance use disorder also have a mental health diagnosis. Request information about the availability of licensed mental health professionals and specific therapies like Cognitive-Behavioral Therapy or Dialectical Behavior Therapy, which are proven to help with both concerns. A quality rehab that takes insurance will be transparent about their ability to support co-occurring conditions and should provide examples of how these services are offered.7
Will my employer find out if I use my work insurance for a San Antonio rehab that takes insurance?
If you use your work insurance for a San Antonio rehab that takes insurance, your employer will not automatically be notified about the specific services you seek. Federal privacy laws, such as HIPAA, strictly protect your health information, including details about substance use disorder treatment. While your employer may see general insurance cost data or overall coverage usage, they do not receive information about your diagnosis or the type of care you access at a rehab that takes insurance. If you need to request time off, you may choose how much to share. Always ask your treatment provider or human resources about your confidentiality rights.2
How long does it typically take to get insurance approval for a San Antonio rehab that takes insurance?
The time it takes to get insurance approval for a San Antonio rehab that takes insurance can vary based on your specific plan and the type of care needed. In many cases, approval for in-network, medically necessary treatment is granted within a few days—especially if your provider submits all required documentation up front. Some insurance companies may require additional clinical information or a prior authorization review, which can extend the process by several days. Parity laws require insurers to process substance use care approvals as promptly as other medical conditions. To speed things along, work closely with your rehab that takes insurance and ask them to handle paperwork and follow up with your insurer.2
What should I do if the San Antonio rehab that takes insurance is out of my network?
If the San Antonio rehab that takes insurance is out of your network, start by contacting your insurance company to ask about any available out-of-network benefits. Some plans may cover a portion of out-of-network treatment, but you might be responsible for higher deductibles or coinsurance. You can also request a “network gap exception” if the rehab provides specialized services not offered by in-network facilities—federal parity laws require insurers to ensure access to essential substance use disorder care. Ask the rehab’s admissions team if they can help with an exception request or provide documentation for medical necessity. Always review your policy, appeal if needed, and consider other in-network options as a backup.2
Does insurance cover continuing care after completing treatment at a San Antonio rehab that takes insurance?
Yes, most insurance plans do cover continuing care after completing treatment at a San Antonio rehab that takes insurance. Continuing care—sometimes called aftercare or ongoing support—may include follow-up counseling, support groups, outpatient therapy, or relapse prevention services. Research demonstrates that adding continuing care to your recovery plan can increase one-year abstinence rates from around 20% to as high as 70%. Coverage details can vary by insurance plan, so it’s wise to check which services are included and if prior authorization is needed. Your rehab that takes insurance can help you understand your specific benefits and coordinate ongoing care.6
Your Path Forward: Taking Action Today
Recovery from substance use disorder is possible, and it begins with a single, courageous decision. Whether someone is struggling with alcohol, opioids, stimulants, or other substances, professional treatment provides the foundation for lasting change. The journey may feel overwhelming, but research shows that approximately 75% of individuals who complete treatment programs achieve significant improvement in their quality of life, with many maintaining long-term recovery when engaged in ongoing support.

Taking that first step means reaching out for help. This might involve calling a treatment center, speaking with a healthcare provider, or confiding in a trusted family member. Many facilities offer free assessments to help determine the most appropriate level of care—these typically include a confidential conversation with a trained counselor who evaluates substance use history, conducts a mental health screening, and reviews medical needs to recommend whether residential treatment, outpatient programs, or medication-assisted treatment would be most effective.
Once someone takes that brave step toward recovery, the support of loved ones becomes invaluable in sustaining that momentum. For those supporting a loved one, remember that compassion and understanding create space for healing. Avoid judgment and instead offer practical assistance—researching treatment options, making phone calls, or simply being present during difficult moments.
The path forward doesn’t require perfection. It requires willingness. Recovery is a process of growth, learning, and rediscovery—whether that means returning to work with renewed focus, reconnecting with children after months or years of distance, or rediscovering hobbies and passions that substance use had overshadowed. With evidence-based treatment and ongoing support, individuals can reclaim their health, rebuild relationships, and create meaningful, fulfilling lives beyond substance use. For immediate help, the SAMHSA National Helpline (1-800-662-4357) provides free, confidential support 24/7 to connect individuals with local treatment resources.
Contact rippleranch.com today to learn how our evidence-based treatment approaches can help you reclaim your health, restore your relationships, and build the fulfilling life you deserve.
References
- How Medicaid Helps People with Substance Use Disorders. https://ccf.georgetown.edu/2025/02/19/how-medicaid-helps-people-with-substance-use-disorders/
- The Mental Health Parity and Addiction Equity Act (MHPAEA). https://www.cms.gov/marketplace/private-health-insurance/mental-health-parity-addiction-equity
- Mental health & substance abuse coverage. https://www.healthcare.gov/coverage/mental-health-substance-abuse-coverage/
- Comparative Effectiveness of Different Treatment Pathways for Opioid Use Disorder. https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2760032
- Cognitive Behavioral Interventions for Alcohol and Drug Use Disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC5714654/
- Impact of Continuing Care on Recovery From Substance Use Disorder. https://pmc.ncbi.nlm.nih.gov/articles/PMC7813220/
- Common Comorbidities with Substance Use Disorders Research. https://www.ncbi.nlm.nih.gov/books/NBK571451/
- Stigma and Discrimination. https://nida.nih.gov/research-topics/stigma-discrimination
- The ASAM Criteria, Fourth Edition. https://www.asam.org/asam-criteria
- Dialectical Behavior Therapy for Substance Abusers. https://pmc.ncbi.nlm.nih.gov/articles/PMC2386852/
