Key Takeaways: Is MAT Treatment Right for You?
- Decision Guide: If you have struggled with opioid use disorder and find that cravings or withdrawal symptoms interrupt your daily life, MAT treatment offers a stabilized path forward. It is particularly effective if you need to balance recovery with work and family obligations.
- Success Metrics: The most successful outcomes rely on three factors: consistent medication adherence (daily or monthly), engagement in behavioral therapy, and retention in the program for at least six months.
- Immediate Action: If you are currently using substances, contact a provider to discuss induction. If you have already detoxed (7-10 days opioid-free), ask specifically about naltrexone options.
Understanding MAT Treatment Fundamentals
What MAT Treatment Combines for Recovery
A successful recovery journey using MAT treatment involves significantly more than just taking a prescription. MAT treatment is intentionally designed as a holistic approach, combining FDA-approved medications—such as methadone, buprenorphine, or naltrexone—with tailored behavioral therapies and counseling. This blend is critical: while medications stabilize brain chemistry to reduce cravings and withdrawal symptoms, counseling addresses the emotional, social, and psychological challenges that often accompany substance use disorders.
To determine if a program offers high-quality care, use this Recovery Planning Checklist to evaluate potential providers:
- Medication Match: Is there an FDA-approved medication prescribed specifically for your biological needs?
- Therapeutic Support: Are regular counseling or behavioral therapy sessions integrated into the schedule?
- Personalization: Is the plan individualized for your unique life circumstances, such as work hours or childcare?
- Care Coordination: Does your care team actively coordinate between medical doctors and mental health providers?
Each component in MAT treatment plays a distinct role. Medications work on the brain’s receptors to decrease the urge to use substances, while therapy sessions help build coping skills, strengthen motivation, and address triggers. Research consistently shows that this combined approach is far more effective than medication or therapy alone3. Major health organizations, including the National Institute on Drug Abuse, recognize that MAT treatment offers the greatest chance for sustained recovery because it addresses both the biological and behavioral aspects of substance use1.
By taking a comprehensive approach, MAT treatment supports individuals in building a healthier, more stable future. The next section explores how this integrated strategy directly addresses the challenges of addiction.
How MAT Treatment Addresses Addiction
To understand how MAT treatment addresses addiction, it helps to use a practical assessment tool: the Addiction Impact Worksheet. This concept encourages you to map out how substance use affects your daily life—physically, emotionally, and socially. By identifying specific areas impacted by addiction, you can better grasp how MAT treatment intervenes on multiple levels.
MAT treatment works by targeting both the biological and behavioral drivers of addiction. Medications such as methadone, buprenorphine, or naltrexone stabilize brain chemistry, reduce the euphoric effects of substances, and ease withdrawal symptoms. This allows you to regain control over cravings and physical dependence, creating a foundation for recovery. Simultaneously, behavioral therapies offered through MAT treatment help address underlying patterns, coping mechanisms, and triggers that may have contributed to substance use.
“People who receive MAT treatment experience significantly lower rates of relapse and overdose, with mortality reduced by as much as 50% compared to those without medication support.”8
Recent CDC data also shows overdose deaths declined by 26.2% from 2023 to 2024, a shift attributed largely to improved access to MAT treatment6. As the next section will show, the choice of medication—whether methadone, buprenorphine, or naltrexone—plays a key role in shaping each person’s experience with MAT treatment.
FDA-Approved Medications in MAT Treatment
Methadone and Buprenorphine Options
When exploring FDA-approved medications for opioid use disorder within MAT treatment, methadone and buprenorphine stand out for their proven effectiveness. However, they function differently and have different requirements. Use the table below to compare which option aligns best with your lifestyle.
| Feature | Methadone | Buprenorphine |
|---|---|---|
| Dosing Schedule | Usually requires daily, in-person visits to a certified clinic. | Often available via outpatient prescription for home use. |
| Mechanism | Full opioid agonist (fully activates receptors). | Partial agonist (activates receptors to a lesser degree). |
| Safety Profile | Effective but requires close monitoring for safety. | Lower risk of misuse and overdose potential (ceiling effect). |
| Best For | Individuals needing high structure and supervision. | Individuals needing flexibility (work/family balance). |
Both medications have demonstrated substantial benefits: studies show that individuals using methadone or buprenorphine as part of MAT treatment experience around a 50% reduction in mortality compared to those not receiving medication8. Treatment retention is also closely linked to proper dosing—retention rates improve when methadone doses exceed 60 mg or buprenorphine is given at 12–16 mg daily9.
This approach works best when treatment is tailored to your daily life, preferences, and medical needs. Next, we’ll look at naltrexone and emerging extended-release options.
Naltrexone and Extended-Release Formulas
When considering FDA-approved options beyond methadone and buprenorphine, naltrexone and extended-release formulations provide important choices within MAT treatment. To guide decision-making, use this Readiness and Lifestyle Match Checklist:
- Detox Status: Have you completed detox and remained opioid-free for at least 7–10 days? (Required for Naltrexone)
- Medication Preference: Is a non-opioid medication preferable for your personal or professional reasons? (Naltrexone)
- Schedule Constraints: Would fewer clinic visits fit better with your work or family schedule? (Extended-release injectables)
- Privacy Needs: Are you seeking a discreet, maintenance-focused approach with less risk of daily dose interruption? (Extended-release options)
Naltrexone works differently than other MAT treatment medications. As an opioid antagonist, it blocks opioid receptors in the brain, preventing the effects of opioids if used. Naltrexone is offered as a daily pill or a monthly injection, with the extended-release injectable (Vivitrol) providing steady protection for up to four weeks. This approach is ideal for people who have completed detox and want a medication without any opioid activity5.
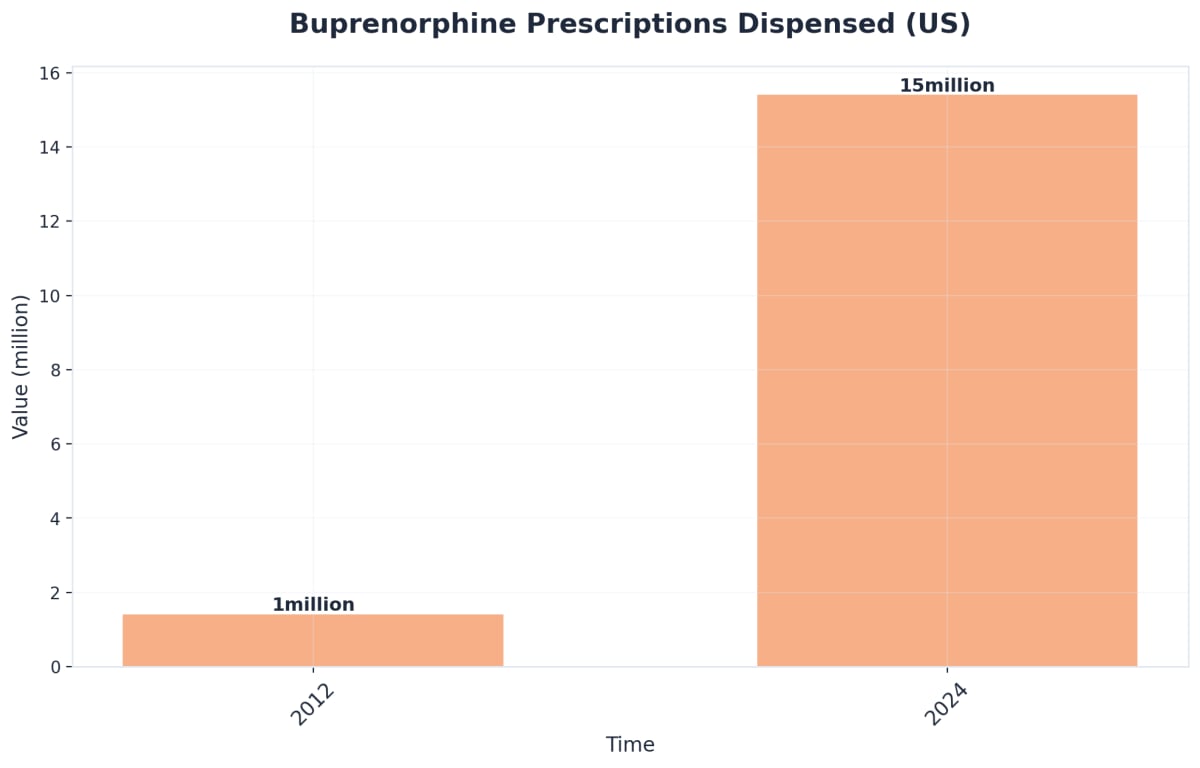
Emerging extended-release formulas—including monthly and weekly buprenorphine injections (Brixadi, Sublocade)—are transforming MAT treatment by improving adherence and reducing the risk of missed doses. Recent studies show that monthly injectable buprenorphine offers the highest probability of treatment retention and opioid abstinence compared to daily oral options10. Consider this route if convenience, privacy, and consistent medication levels are priorities.
Evidence Supporting MAT Treatment Success
Mortality Reduction and Health Outcomes
A practical way to understand the impact of MAT treatment is by using a Health Outcomes Tracker, which allows individuals and families to monitor key improvements such as fewer emergency room visits, better physical health, and increased stability in daily life. MAT treatment stands out for its ability to reduce the risk of overdose and death. In fact, people who receive MAT treatment with methadone or buprenorphine experience approximately a 50% reduction in mortality compared to those who do not receive medication support8.
Recent national data reinforce these findings. Between 2023 and 2024, overdose deaths in the United States dropped by 26.2%, with expanded access to MAT treatment cited as a major factor in this positive trend6. The World Health Organization also recommends opioid agonist maintenance treatment—such as methadone and buprenorphine—as the intervention with the strongest evidence for reducing both mortality and serious health complications associated with opioid use7.
Beyond survival, MAT treatment is linked to lower rates of infectious disease transmission, improved mental health, and greater social stability. These benefits are especially important for individuals balancing work, family, and community responsibilities. The next section will explore how treatment retention and long-term engagement in MAT treatment play a crucial role in supporting lasting recovery.
Treatment Retention and Long-Term Results
A practical tool for evaluating success in MAT treatment is the Recovery Engagement Checklist. Ask yourself: Are you attending scheduled appointments consistently? Have you maintained medication adherence for three months or more? Are you experiencing fewer cravings and improved quality of life? Higher engagement and longer retention in MAT treatment are closely linked to better long-term recovery outcomes.

Research shows that individuals who remain in MAT treatment for at least six months are much more likely to avoid relapse and sustain improvements in health and daily functioning8. In fact, staying engaged in MAT treatment is associated with a significant reduction in illicit opioid use, lower risk of returning to substance use, and improved social stability. A notable finding is that treatment retention rates increase when methadone doses exceed 60 mg or buprenorphine is prescribed at 12–16 mg daily, highlighting the importance of individualized dosing9.
Newer extended-release buprenorphine injections also demonstrate the highest probability of treatment retention and opioid abstinence, offering another option for those who benefit from less frequent dosing10. This path makes sense for people seeking lasting change, especially when balancing work, family, and personal responsibilities. Sustained engagement in MAT treatment offers a strong foundation for rebuilding life over the long term.
Accessing MAT Treatment and Overcoming Barriers
Insurance Coverage and Policy Reforms
Navigating insurance coverage and recent policy reforms is crucial for expanding access to MAT treatment. Use this Coverage Readiness Checklist to prepare for conversations with your provider and insurer:
- Formulary Check: Does your insurance (private or public) explicitly cover all FDA-approved MAT treatment medications?
- Authorization Status: Are you aware of any prior authorization requirements that might delay your start date?
- Advocacy Support: Has your provider offered to assist with appeals or paperwork if access is delayed?
- Comprehensive Benefits: Do your benefits include both medication and counseling support?
Despite significant progress, insurance-related barriers remain a major challenge. Currently, 40% of people with private insurance face prior authorization steps before they can begin MAT treatment, which can delay or even prevent timely care8. Additionally, only 23% of publicly funded treatment programs offer any FDA-approved MAT treatment medications, highlighting persistent gaps in access8. Fortunately, momentum for reform is growing. Major insurers are starting to reduce or eliminate prior authorization requirements, and new federal guidelines are pushing for more streamlined access.
People benefit most when insurance plans automatically cover MAT treatment medications and behavioral therapies, without unnecessary administrative hurdles. Successful policy changes—such as removing prior authorization—have already contributed to increased treatment uptake and a notable decline in overdose deaths across the United States6.
Telehealth and Flexible Care Options
Telehealth and flexible care options have become essential for expanding access to MAT treatment, especially for people facing transportation challenges, busy schedules, or living in rural areas. A practical decision tool is the Access Fit Assessment:
- Provider Availability: Is it hard to find a local MAT treatment provider within a reasonable distance?
- Logistical Hurdles: Are work, childcare, or travel concerns making in-person visits difficult?
- Consistency Check: Would virtual appointments make it easier to stay consistent with your care plan?
- Scheduling Needs: Do you need evening or weekend scheduling to maintain employment?
Telehealth allows individuals to receive MAT treatment—including medical assessments, medication management, and counseling—remotely using secure video or phone platforms. This flexibility has led to a 15% higher rate of medication adherence in virtual MAT programs compared to traditional clinic visits, according to a 2022 meta-analysis10. Flexible options, such as evening telehealth visits and medication pickup at local pharmacies, make it easier for individuals to fit treatment into their daily lives.
For people in rural communities, telehealth overcomes long travel times that often exceed 45 minutes each way, addressing one of the biggest barriers to starting and continuing MAT treatment. Opt for this framework when your schedule or location limits your ability to attend frequent in-person appointments.
Frequently Asked Questions
Can I receive MAT treatment while continuing to work or care for my family?
Yes, you can receive MAT treatment while continuing to work or care for your family. MAT treatment is intentionally designed to fit around daily responsibilities, offering flexible options such as outpatient appointments, telehealth visits, and even extended-release medications that require less frequent dosing. Many individuals manage their jobs, parenting duties, and other commitments while in MAT treatment, thanks to these adaptable care models. Research shows that increasing access to telehealth and flexible scheduling supports better treatment adherence—up to 15% higher in virtual MAT programs compared to traditional in-person visits10. With support from your care team, MAT treatment can become a steady part of your routine, helping you maintain both your recovery and your life responsibilities.
How do I choose between methadone, buprenorphine, and naltrexone for MAT treatment?
Choosing between methadone, buprenorphine, and naltrexone for MAT treatment depends on your health history, daily routine, and recovery goals. Methadone is effective if you can visit a clinic daily and benefit from close supervision. Buprenorphine often suits those seeking flexibility, as it can be prescribed for home use or through telehealth, and has a lower risk of misuse. Naltrexone is a good option if you’ve already completed detox and want a non-opioid medication, but starting it requires you to be opioid-free for 7–10 days5. Each MAT treatment option is equally valid when matched to your unique needs.
Will my insurance require prior authorization before I can start MAT treatment?
Many insurance plans still require prior authorization before starting MAT treatment, which can delay access to vital care. Currently, about 40% of people with private insurance face these extra approval steps, even when their doctor recommends MAT treatment8. This process may involve your provider submitting forms and waiting for insurer approval before medication is covered. However, some insurers are working to remove these barriers, and recent policy reforms are making it easier for more people to access MAT treatment without delays. If you run into obstacles, ask your provider for help with paperwork and appeals—persistent advocacy often makes a difference8.
How long will I need to stay on MAT treatment before I can stop taking medication?
The length of time someone stays on MAT treatment varies widely and is highly individual. Some people may benefit from MAT treatment for several months, while others find long-term or even lifelong medication support is the best way to maintain recovery and reduce relapse risk. Research shows that remaining on MAT treatment for at least six months greatly increases the chances of achieving stability and avoiding relapse8. Decisions about when to taper or stop medication should always be made in partnership with your healthcare provider, based on your progress, life circumstances, and ongoing needs. There is no one-size-fits-all answer—successful MAT treatment is about what supports your health and long-term recovery.
Does MAT treatment address co-occurring mental health conditions like anxiety or PTSD?
Yes, MAT treatment can address co-occurring mental health conditions such as anxiety or PTSD. Most MAT treatment programs integrate behavioral therapies and counseling alongside medication, which means individuals receive support for both substance use and mental health challenges. These services are often tailored to meet each person’s unique needs, so issues like anxiety, depression, or trauma can be addressed in the same care plan. According to national guidelines, combining medication with evidence-based behavioral therapies is key to effective MAT treatment for those with complex needs, including co-occurring disorders1. It’s important to discuss your mental health history with your provider to ensure your MAT treatment plan includes the right supports.
What happens if I experience a setback or return to substance use while on MAT treatment?
Experiencing a setback or returning to substance use while on MAT treatment is not uncommon, and it does not mean that recovery is out of reach. MAT treatment is designed to support individuals through ups and downs, recognizing that recovery is a process. If a setback occurs, the best step is to reach out to your care team—they can adjust your medication, increase support through counseling, or help you identify new strategies for managing triggers. Research shows that staying engaged in MAT treatment, even after a setback, significantly increases the chances of long-term stability and reduced relapse risk8. Compassion, honesty, and continued connection with your care providers are essential for moving forward.
Are newer extended-release MAT treatment options more effective than daily medications?
Newer extended-release MAT treatment options, such as monthly or weekly buprenorphine injections, have shown promising results compared to daily oral medications. Research indicates that these long-acting formulations offer the highest probability of treatment retention and opioid abstinence, while their safety profiles remain similar to daily medications10. For many, the convenience of less frequent dosing and reduced risk of missed doses make extended-release MAT treatment an appealing choice. This approach works best for individuals seeking consistency and privacy, or for those who have struggled with keeping up with daily medication schedules. Discussing all MAT treatment options with your care team can help determine which is most effective for your needs.
Your Path Forward with MAT Treatment
Taking the first step toward medication-assisted treatment represents a meaningful commitment to recovery. This evidence-based approach combines FDA-approved medications with counseling and behavioral therapies, creating a comprehensive support system designed around individual needs. Research demonstrates that MAT reduces opioid overdose deaths by approximately 50% and significantly improves treatment retention rates. According to the Substance Abuse and Mental Health Services Administration, patients receiving MAT are 75% more likely to remain in treatment compared to those receiving behavioral therapy alone. This pathway addresses both the physical and psychological aspects of recovery—for instance, medications like buprenorphine reduce cravings and withdrawal symptoms while concurrent cognitive-behavioral therapy helps identify triggers and develop healthier coping strategies.
Starting MAT treatment begins with a thorough assessment by qualified healthcare providers who understand the complexities of substance use disorders. They’ll work with you to determine which medication option—whether buprenorphine, methadone, or naltrexone—best aligns with your specific situation. Throughout this journey, regular monitoring and adjustments ensure the treatment remains effective as circumstances evolve.
Remember that MAT treatment isn’t a one-size-fits-all solution. Success looks different for everyone, and progress happens at its own pace. The combination of medication support and therapeutic interventions provides stability while building essential coping skills. With professional guidance and personal commitment, MAT treatment offers a proven foundation for lasting recovery and renewed hope for the future.
References
- Medications for Opioid Use Disorder – National Institute on Drug Abuse. https://nida.nih.gov/research-topics/medications-opioid-use-disorder
- SAMHSA – Substance Abuse and Mental Health Services Administration. https://www.samhsa.gov
- Medication-Assisted Treatment Improves Outcomes – Pew Charitable Trusts. https://www.pew.org/en/research-and-analysis/fact-sheets/2016/11/medication-assisted-treatment-improves-outcomes-for-patients-with-opioid-use-disorder
- Progress Under Threat: The Future of Overdose Prevention – Brookings Institution. https://www.brookings.edu/articles/progress-under-threat-the-future-of-overdose-prevention-in-the-united-states/
- Information about Medications for Opioid Use Disorder (MOUD) – FDA. https://www.fda.gov/drugs/information-drug-class/information-about-medications-opioid-use-disorder-moud
- Drug Overdose Deaths in the United States, 2023–2024 – CDC. https://www.cdc.gov/nchs/products/databriefs/db549.htm
- WHO Updates Guidelines on Opioid Dependence Treatment and Overdose Prevention – World Health Organization. https://www.who.int/news/item/09-02-2025-who-updates-guidelines-on-opioid-dependence-treatment-and-overdose-prevention
- Medication-Assisted Treatment: Evidence and Policy Recommendations – AMA/AAPM&R. https://www.aapmr.org/docs/default-source/advocacy/pain-management/ama-aapm-r-mat-one-pager.pdf
- The Effectiveness of Medication-Based Treatment for Opioid Use Disorder – NIH/NCBI. https://www.ncbi.nlm.nih.gov/books/NBK541393/
- Effectiveness and Safety of Therapies for Opioid Use Disorder: Buprenorphine Long-Acting Injectable – NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC12884343/
