Key Takeaways: Your Recovery Decision Guide
- Assess Your Needs: If you require 24/7 medical supervision, prioritize residential care; if you must maintain employment, look for Intensive Outpatient Programs (IOP).
- Check Your Coverage: Verify if your insurance plan (HMO vs. PPO) covers dual diagnosis treatment to minimize out-of-pocket costs.
- Immediate Action: If you or a loved one is in crisis, call the local 988 lifeline immediately for diversion to behavioral health services rather than law enforcement.
Understanding Austin’s Addiction Crisis
Opioid Epidemic in Travis County
The search for effective rehab Austin solutions has become increasingly critical as the city faces an alarming opioid crisis. Neighborhoods like East Riverside, South Congress, and Rundberg Lane are feeling the impact most acutely. Recent data paints a stark picture of the urgency required in Travis County:
- 158% surge in fatal opioid overdoses from 2020 to 2023.
- 686% increase in overdose deaths driven specifically by Fentanyl1.
- 250 lives lost in just the first half of 2023 alone1.
Austin’s unique blend of urban growth and social challenges—from the bustling nightlife around 6th Street to the community hubs in Hyde Park—creates a dynamic environment where both risk and opportunity for intervention coexist. While the city’s accessible roadways, such as I-35 and MoPac, allow residents from neighborhoods like Mueller and Zilker to reach life-saving services, barriers such as transportation and stigma persist.
Residents who have participated in rehab Austin programs often share stories of renewed hope, especially those from South Austin who found support and recovery after losing loved ones to opioid addiction. With such a visible crisis, the community response is growing stronger, bringing together families and support networks from across the city1.
Next, we’ll examine how co-occurring mental health conditions complicate the opioid epidemic and why integrated care is essential for lasting recovery.
Co-Occurring Disorders and Mental Health
Co-occurring mental health conditions—like anxiety, depression, and trauma-related disorders—are deeply intertwined with substance use challenges across Austin. In neighborhoods such as Cherrywood, Brentwood, and Allandale, care providers frequently see how untreated depression or anxiety can intensify substance use, while ongoing use can worsen mental health symptoms.

Research indicates that approximately 21.2 million adults in the U.S. experience both a mental health and substance use disorder, reinforcing the need for rehab Austin treatment centers that address both simultaneously3. Austin’s local response has grown stronger with expanded options for integrated care:
- Crisis Diversion: The 988 Suicide & Crisis Lifeline diverts over 80% of calls away from police, connecting residents in Clarksville and North Loop directly to behavioral health services2.
- Trauma-Informed Standards: Treatment protocols now regularly account for trauma histories, which are high-risk factors for substance use6.
Residents who have attended rehab Austin programs in areas like Barton Hills share stories of progress after finally receiving care for both depression and substance use, rather than just one or the other. The city’s network of support continues to expand, offering hope for those facing the dual challenges of mental health and substance use.
Evidence-Based Rehab Austin Treatment Approaches
Integrated Dual Diagnosis Treatment
Integrated dual diagnosis treatment is essential for people in Austin who face both substance use and mental health challenges. In neighborhoods like North Loop, Hyde Park, and South Congress, residents often experience how depression, anxiety, or trauma can complicate recovery. Rehab Austin programs that offer integrated care address both conditions at the same time, using a team-based approach that blends behavioral therapies, medication support, and trauma-informed counseling.
Evidence shows that this model leads to far better outcomes than treating each issue separately. A multi-center study found an 88% reduction in intoxication rates among individuals who received dual diagnosis treatment within 6 to 12 months after leaving care, with over two-thirds maintaining remission3. Austin’s leading centers often utilize the following therapies:
| Therapy Type | Primary Focus | Key Statistic |
|---|---|---|
| Cognitive Behavioral Therapy (CBT) | Identifying and changing negative thought patterns. | Widely effective for anxiety and depression. |
| Dialectical Behavior Therapy (DBT) | Emotional regulation and distress tolerance. | Shown to keep 64% of participants in treatment vs. 27% standard4. |
| EMDR | Processing traumatic memories. | Critical for PTSD-related substance use. |
Residents from Zilker and Crestview who have attended these programs frequently share that a focus on both their mental health and recovery journey made long-term healing possible. With local access near MoPac and easy parking at many facilities, integrated dual diagnosis treatment is increasingly accessible to people throughout the city.
Medication-Assisted Treatment Options
Medication-assisted treatment (MAT) is a cornerstone of evidence-based care at many rehab Austin facilities, especially for those working to overcome opioid dependence. In neighborhoods like East Riverside, Windsor Park, and Clarksville, residents have seen firsthand how MAT helps reduce cravings and stabilize recovery. MAT combines FDA-approved medications with counseling and behavioral therapies.
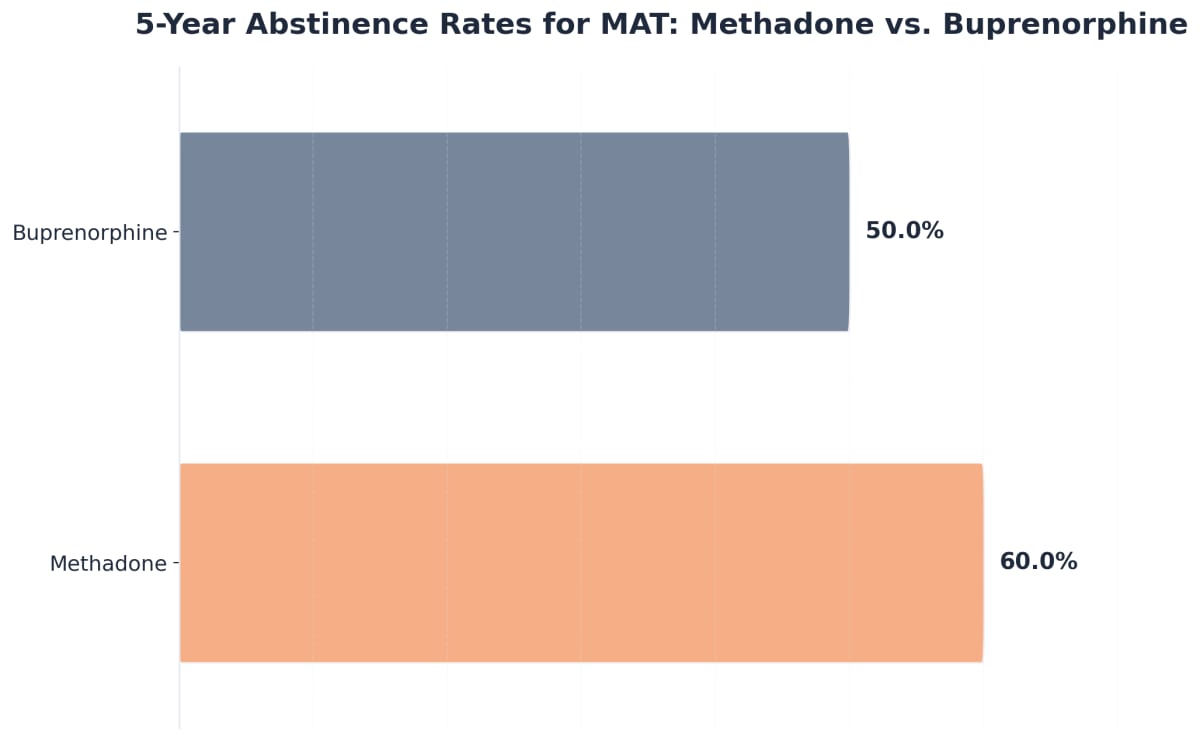
Long-term research demonstrates high efficacy rates for these interventions:
- Methadone: Approximately 60% of patients remain abstinent from opioids after five years5.
- Buprenorphine: Approximately 50% of patients remain abstinent from opioids after five years5.
Access to MAT in Austin is expanding, with many centers located near major roads like I-35 and close to neighborhoods such as Tarrytown and South Lamar. Many clinics offer flexible scheduling and accessible parking, which helps residents overcome common barriers. One Windsor Park resident shared, “After starting MAT, I was finally able to keep a steady job and reconnect with my family.”
Levels of Care and Program Flexibility
Residential vs. Outpatient Programs
Residential and outpatient programs each play a key role in the landscape of rehab Austin, offering varying levels of structure and flexibility. In areas like Westlake, South Lamar, and the vibrant Mueller district, individuals often weigh the benefits of 24/7 residential care against the adaptability of outpatient options.
| Feature | Residential Rehab | Outpatient / IOP |
|---|---|---|
| Environment | Immersive, 24/7 support, often near nature (e.g., Lady Bird Lake). | Home-based, attending clinics in areas like Cherrywood or Tarrytown. |
| Best For | Severe addiction, medical detox needs, removing triggers. | Balancing work/school, supportive home environments. |
| Outcome Data | High success for acute stabilization. | Outcomes equivalent to residential for many participants8. |
One resident from South Lamar shared, “The outpatient program gave me the support I needed while letting me keep my job and be there for my kids.” Another, from Mueller, appreciated the ease of parking and access to public transit, making appointments less stressful. Choosing between these levels of care often depends on personal needs, safety, and life circumstances.
Telehealth and Professional Options
Telehealth and professional support options have transformed access to rehab Austin services, especially for residents in neighborhoods like North Burnet, Windsor Park, and Travis Heights. Virtual care makes it possible for people across the city to participate in individual therapy, group counseling, and medication management from the comfort of home.

This flexibility reduces common barriers such as:
- Traffic congestion on I-35.
- Parking costs and availability near Downtown.
- Scheduling conflicts with work or childcare.
Research shows that telehealth treatment for substance use is just as effective as in-person care for most services, including intensive outpatient programs and individual counseling7. Providers in Austin have embraced these advances, often blending telehealth with periodic in-person sessions to strengthen therapeutic relationships. One Travis Heights resident noted, “Virtual therapy made it possible to stay connected to my counselor, even on days when I couldn’t leave home.”
Choosing the Right Rehab Austin Facility
Trauma-Informed and Holistic Care
Trauma-informed and holistic care are foundational in choosing a rehab Austin facility, especially for residents in neighborhoods like Bouldin Creek, Windsor Park, and the Red River Cultural District. Many Austin centers are located near familiar landmarks like Zilker Park and the Texas State Capitol, offering environments that feel safe and welcoming.
Trauma-informed care recognizes that a significant number of individuals seeking support have lived through difficult experiences—such as violence, loss, or chronic stress. Research confirms that trauma survivors are at higher risk for substance use disorders, depression, and anxiety, making this approach vital for lasting recovery6. Holistic programs often integrate the following wellness activities:
- Mindfulness & Yoga: Helping residents in Hyde Park find calm.
- Nutrition Support: Improving mood and physical healing.
- Nature Therapy: Utilizing spaces like Lady Bird Lake for connection.
Austin’s facilities often offer flexible schedules, accessible parking, and options for family involvement, making participation easier for those commuting from places like North Loop or The Domain. Trauma-informed and holistic care approaches are recommended by national best-practices guidelines for their effectiveness in supporting lasting change6.
Insurance Coverage and Accessibility
Insurance coverage and accessibility are crucial concerns for many Austin residents as they seek rehab Austin services. In neighborhoods like Oak Hill, Cherrywood, and North Burnet, individuals often encounter obstacles related to insurance approvals or limited provider networks. Despite federal and Texas mental health parity laws, research shows that insurance companies still apply more restrictive standards to substance use treatment compared to other types of medical care9.
To navigate these challenges, consider the following steps:
- Verify Benefits: Contact your provider to check for “behavioral health” coverage.
- Ask for Help: Utilize the insurance navigation assistance provided by many Austin facilities.
- Check Logistics: Ensure the facility is accessible via major routes like MoPac or has telehealth options.
Community advocacy in Austin continues to push for more equitable access, especially for residents in underserved neighborhoods. Research emphasizes that closing insurance gaps and increasing local provider availability are essential steps toward effective and timely treatment9.
Frequently Asked Questions
How long does rehab Austin treatment typically last?
The length of rehab Austin treatment depends on individual needs and the type of program chosen. Most residential rehab Austin programs in the city typically last 28 to 90 days. Outpatient programs can be shorter or may extend over several months, offering flexibility for those balancing work or family responsibilities. Research highlights that ongoing support and engagement, such as participating in aftercare or alumni networks, significantly improve long-term recovery outcomes10. Austin facilities in neighborhoods like Mueller and South Lamar work with each person to create a plan that fits their goals, supporting sustained progress even after formal treatment ends.
Can I continue working while attending rehab Austin programs?
Yes, many rehab Austin programs make it possible for you to continue working while receiving care. Outpatient options, including intensive outpatient programs (IOPs) and telehealth services, are especially popular in neighborhoods like South Lamar, Cherrywood, and North Burnet. These programs offer flexible scheduling, allowing you to attend therapy or group sessions outside of traditional work hours. Research shows that telehealth and outpatient treatments deliver outcomes equivalent to in-person care, helping people balance recovery and employment responsibilities7, 8. Local residents often share that maintaining a job during treatment provides a sense of stability and normalcy throughout their rehab Austin journey.
What neighborhoods in Austin do treatment centers serve?
Austin treatment centers serve a wide network of neighborhoods, making rehab Austin accessible for residents across the city. Facilities are located in areas such as Downtown, Mueller, South Lamar, Windsor Park, and North Burnet, with additional options in Bouldin Creek and Cherrywood. Many centers are just minutes from community landmarks like Lady Bird Lake or close to The Domain, offering convenience and familiarity. Whether you live near bustling South Congress or the quieter streets of Allandale, you’ll find programs designed to meet your needs. This wide coverage helps reduce transportation barriers and ensures more equitable access to care for people throughout Austin1, 7.
Will my insurance cover rehab Austin services?
Many Austin residents ask if their insurance will cover rehab Austin services. Most private insurance plans and Medicaid are required by law to cover substance use disorder treatment, but the extent of coverage can vary by plan and provider. Research shows that, despite parity laws, insurance companies sometimes impose stricter limits or extra steps for approval of rehab Austin care compared to other medical services, leading to delays or denials for some individuals9. It’s helpful to contact your provider directly and work with the rehab Austin center’s insurance team to understand your specific benefits and any required paperwork. Local facilities often offer assistance with insurance navigation, making the process less stressful.
What happens after I complete my rehab Austin program?
After completing your rehab Austin program, your journey continues with support designed to help you maintain long-term recovery. Many Austin centers offer aftercare services such as alumni groups, peer support meetings, and ongoing counseling. Research highlights that staying engaged in recovery support programs, like those found in local neighborhoods or through virtual options, significantly reduces relapse risk and promotes sustained wellness10. Alumni from areas like Mueller and South Lamar often share that regular check-ins and community activities make it easier to stay connected and motivated. Your care team will help you create a personalized aftercare plan, ensuring you have tools and resources as you move forward.
How do I know if I need residential or outpatient rehab Austin treatment?
Deciding between residential and outpatient rehab Austin treatment depends on several personal factors, including the severity of substance use, mental health needs, and your home environment. Residential programs offer 24/7 support and a structured setting, which may be best if you have intense cravings, need distance from triggers, or require medical supervision. Outpatient rehab Austin treatment can be just as effective for many people, especially if you have a supportive home life and need to balance work or family responsibilities. Research shows that intensive outpatient programs in Austin provide outcomes equivalent to residential care for many participants8. Consulting with a local treatment professional can help you choose the approach that fits your needs best.
Can family members participate in my rehab Austin recovery process?
Yes, family members are encouraged to participate in your rehab Austin recovery process. Many Austin treatment centers offer dedicated family therapy sessions, educational workshops, and support groups to help loved ones understand the recovery journey and develop healthier communication patterns. Involving family can improve outcomes by creating a strong support network and addressing any challenges at home. Research supports that family involvement in addiction treatment leads to better engagement and long-term recovery success6. Programs in neighborhoods like Windsor Park and South Lamar often invite families to join in-person or virtual sessions, making it convenient for those with busy schedules or transportation needs.
Conclusion
Breaking free from substance use disorders demands courage, commitment, and comprehensive support. While the path forward may feel overwhelming at times, understanding available treatment options and evidence-based resources can make all the difference in achieving lasting wellness.
Whether someone is exploring outpatient counseling, intensive therapy programs, or residential treatment, the most important step is reaching out for help. Research shows that individuals who complete treatment programs have success rates ranging from 40-60%—comparable to other chronic conditions like diabetes and hypertension. Evidence-based approaches combined with compassionate care create the foundation for meaningful, sustainable change.
Every individual’s experience with addiction is unique, which means treatment plans should be tailored to address specific needs, circumstances, and goals. From medically supervised detoxification through ongoing aftercare coordination, a continuum of care ensures that people receive appropriate interventions at each stage of their healing process—building on the assessment strategies, treatment modalities, and support systems discussed throughout this guide.
For those ready to take the next step, concrete resources stand ready to provide guidance and hope. The SAMHSA National Helpline (1-800-662-4357) offers free, confidential, 24/7 information and referrals, while organizations like the National Institute on Drug Abuse (NIDA.nih.gov) provide evidence-based information for individuals and families. No one needs to face these challenges alone. The time to act is now: identify one resource, make one call, take one step forward today. With the right combination of professional treatment, peer connection, and personal determination, individuals can reclaim their lives and build a healthier, more fulfilling future.
References
- 2020-2023 Opioid Overdose Surveillance Report – City of Austin. https://www.austintexas.gov/sites/default/files/files/Health/Epidemiology/Opioids/2020-2023-Overdose-Surveillance-Report.pdf
- Fact Sheet: Spotlight on Austin, Texas Mental Health and Substance Use Crisis Care. https://www.samhsa.gov/sites/default/files/988-austin-fact-sheet.pdf
- The effects of residential dual diagnosis treatment on alcohol abuse – Multi-center Study. https://pmc.ncbi.nlm.nih.gov/articles/PMC5576155/
- Dialectical Behavior Therapy for Substance Abusers – NIH Evidence Review. https://pmc.ncbi.nlm.nih.gov/articles/PMC2797106/
- Long-term Effects of Buprenorphine & Methadone on Opioid Use – Recovery Research Institute. https://www.recoveryanswers.org/research-post/long-term-effects-of-buprenorphine-methadone-on-opioid-use/
- TIP 57 Trauma-Informed Care in Behavioral Health Services – SAMHSA Treatment Improvement Protocol. https://library.samhsa.gov/sites/default/files/sma14-4816.pdf
- Addiction Treatment and Telehealth: Review of Efficacy and Provider Insights During COVID-19. https://pubmed.ncbi.nlm.nih.gov/34644125/
- Substance Abuse Intensive Outpatient Programs: Assessing Effectiveness. https://pmc.ncbi.nlm.nih.gov/articles/PMC4152944/
- Insurance barriers to substance use disorder treatment after ACA and Parity Laws. https://pmc.ncbi.nlm.nih.gov/articles/PMC9948907/
- The Emergence, Role, and Impact of Recovery Support Services. https://pmc.ncbi.nlm.nih.gov/articles/PMC7996242/
