Key Takeaways
- Neighborhoods Served: Comprehensive care is accessible across Southtown, Stone Oak, Alamo Heights, Harlandale, and the West Side.
- City-Specific Data: Currently, only 27.5% of San Antonio Medicaid patients remain engaged in treatment at the six-month mark, highlighting the need for integrated care models.
- Local Landmarks: Facilities are strategically located near recognizable points like the San Antonio River Walk and the Pearl District to ensure discrete, convenient access.
- Transportation & Access: Clinics prioritize placement along major commuter routes, including Loop 410 and near VIA Centro Plaza, to minimize logistical barriers for working professionals.
Medication-Assisted Treatment at a Methadone Clinic San Antonio
San Antonio’s Evolving Opioid Treatment Landscape
San Antonio’s opioid treatment landscape is shaped by both its unique geography and the evolving needs of its residents. With neighborhoods like Southtown, Alamo Heights, the West Side, Stone Oak, and King William facing distinct patterns of substance use, the presence of a methadone clinic San Antonio remains a vital anchor in the community’s response. The city’s proximity to historic sites, such as the Alamo and San Pedro Springs Park, underscores how these challenges affect every corner of the metro area—from the arts districts near the River Walk to the busy medical corridor by the South Texas Medical Center.
The urgency of local action became clear in November 2024, when the San Antonio City Council formally declared overdoses a public health crisis, prompting a coordinated response among providers, public agencies, and neighborhood organizations8. Recent expansions in Medicaid coverage and flexible take-home dosing regulations have improved accessibility, especially for those commuting from areas like the Pearl District or the Loop 410 corridor2.
Despite these gains, the city still faces low treatment retention rates—just 27.5% of Medicaid patients remain in care after six months10. Testimonies from residents in Monte Vista and Dignowity Hill reflect both the hope and challenge of recovery.
“The new clinic near Mission Concepción helped me keep my job and rebuild trust with my family.”
As the city continues adapting its approach, the next section will explore how pharmacological interventions function within a comprehensive recovery framework.
How Methadone Functions in Recovery
Methadone remains a central element of medication-assisted treatment (MAT) in San Antonio’s efforts to address opioid use disorder. As a full mu-opioid receptor agonist, methadone prevents withdrawal symptoms and stabilizes brain chemistry, reducing cravings without inducing euphoria when used as prescribed9. This pharmacological profile allows patients across neighborhoods like Southtown, Stone Oak, the West Side, and Alamo Heights to regain daily stability, maintain employment, and re-engage with community life.
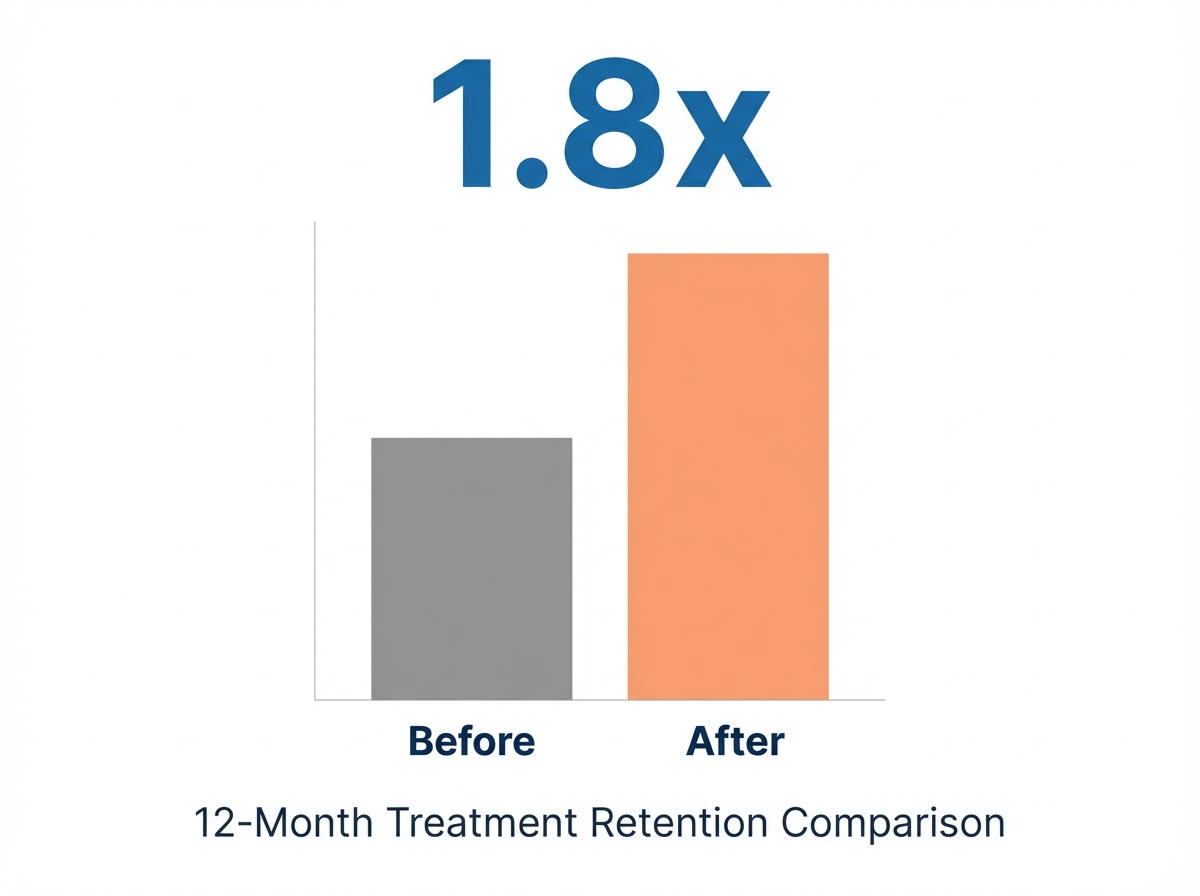
The effectiveness of this intervention is supported by robust data. Patients receiving treatment at a methadone clinic San Antonio are approximately 1.8 times more likely to remain in care at the one-year mark than those using alternative medications3. Such improvements are particularly meaningful in high-traffic corridors near the Medical Center or along Loop 410, where work and family responsibilities often compete with the demands of recovery.
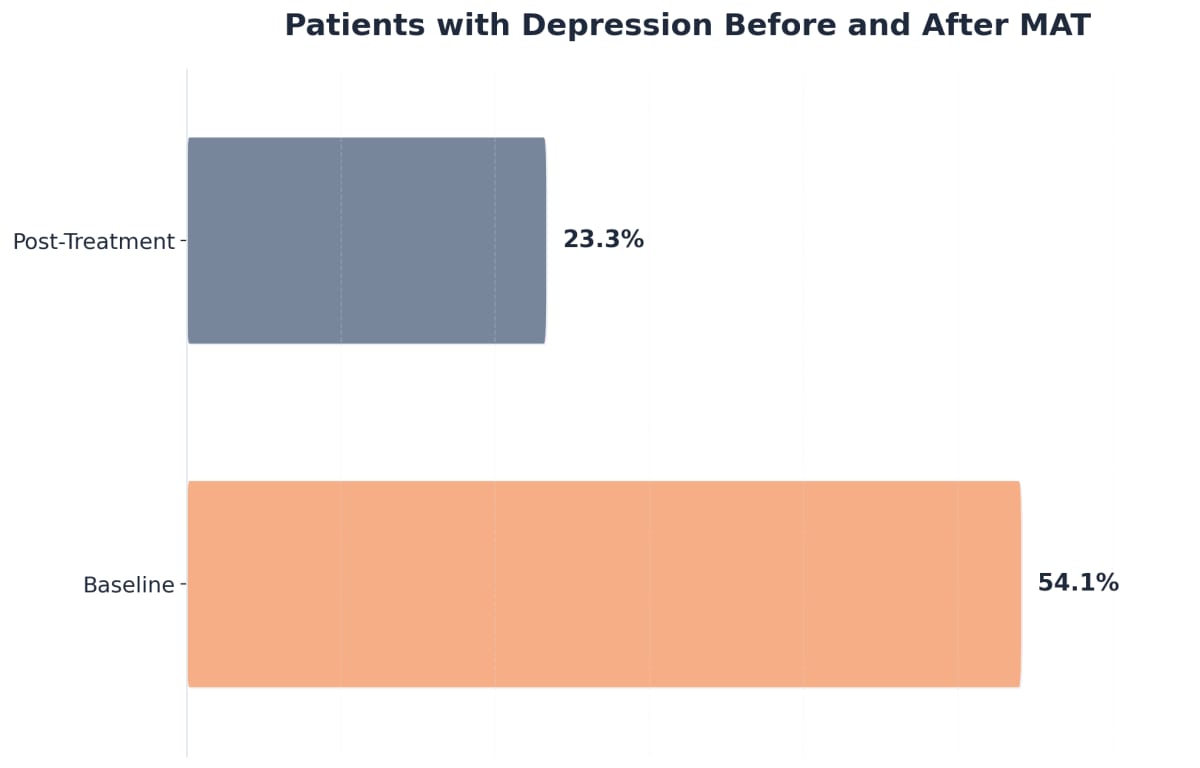
| Clinical Metric | Intake Baseline | Six-Month Mark | Overall Improvement |
|---|---|---|---|
| Heroin Utilization | 52.1% | 20.4% | -31.7% |
| Depressive Symptoms | 54.1% | 23.3% | -30.8% |
“Sticking with treatment helped me keep my apartment and reconnect with my son.”
Despite these successes, retention remains a challenge—underscoring the need for integrated approaches, which the next section will explore.
Why Integrated Dual Diagnosis Care Matters at a Methadone Clinic San Antonio
Co-Occurring Disorders and Treatment Outcomes
Co-occurring mental health conditions, such as anxiety, depression, PTSD, and bipolar disorder, significantly shape treatment outcomes for individuals receiving care at a methadone clinic San Antonio. In neighborhoods like Tobin Hill, Harlandale, Stone Oak, and the Deco District, professionals regularly encounter patients whose substance use disorder is intertwined with mental health challenges. These intersections are not merely clinical abstractions—they’re realities affecting daily functioning, engagement, and the likelihood of sustained recovery.
Research demonstrates that when standard medication-assisted treatment is combined with integrated cognitive behavioral therapy, patients with both opioid use disorder and a co-occurring mental health condition experience significantly better outcomes than with medication alone7. For example, a recent analysis found that integrated approaches led to lower rates of positive drug screens among patients with PTSD and opioid use disorder, compared to those who received only standard care.
- Enhanced Stability: Simultaneous treatment of mental health and substance use reduces the risk of relapse.
- Improved Retention: Patients receiving comprehensive care are more likely to stay engaged beyond the critical six-month mark.
- Better Quality of Life: Integrated models support employment retention and family reunification.
Despite these promising results, San Antonio still faces retention obstacles. Only 27.5% of Medicaid patients remain engaged in treatment at six months, and rates are even lower among those with co-occurring disorders10. Addressing co-occurring disorders is a priority for neighborhood providers, especially in areas impacted by heavy traffic, limited parking, or safety concerns around the San Antonio River Walk.
Evidence-Based Approaches Beyond Medication
Locally, evidence-based care at a methadone clinic San Antonio extends well beyond medication, especially in areas like Southtown, the Deco District, Alamo Heights, and the Medical Center. Near landmarks such as the Pearl and Mission Concepción, clinics have adopted a range of integrated therapies—mindfulness-based relapse prevention, trauma-informed counseling, and structured group interventions—that reflect the city’s unique mix of patient needs and neighborhood environments.
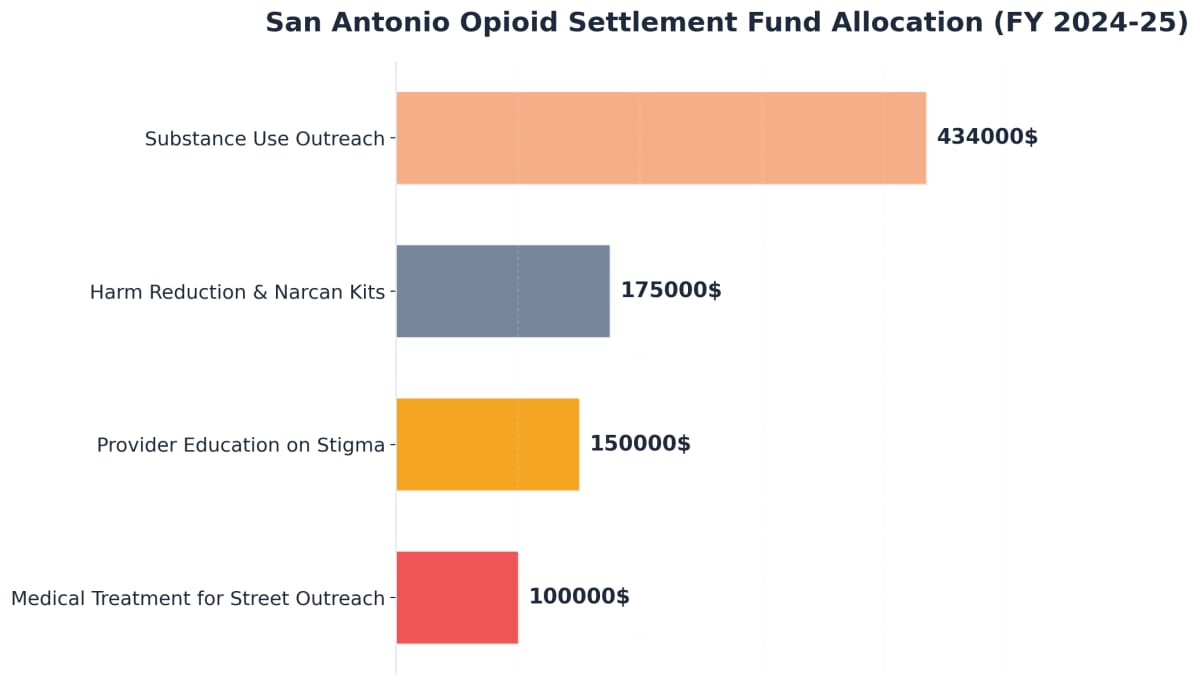
San Antonio’s recent allocation of $909,000 in opioid settlement funds has enabled expanded outreach, street-based medical services, and stigma-reduction education tailored to high-need areas like the West Side and Harlandale4. In practice, this means mobile counseling units now visit neighborhoods close to VIA Centro Plaza and the Loop, making services more accessible for those facing transportation or parking barriers.
For clinical administrators managing these integrated programs, optimizing the electronic health record (EHR) system is crucial for tracking outcomes. Staff often use specific keystrokes like Ctrl + Shift + M to quickly pull up MAT billing templates. Below is an example of a standard JSON configuration used by local facilities for tracking dual-diagnosis patient metrics:
{
"patient_tracking": {
"mat_status": "active",
"dual_diagnosis": true,
"therapy_modalities": ["CBT", "EMDR"],
"neighborhood_zone": "Southtown"
}
}By focusing on comprehensive, neighborhood-informed strategies, providers are improving engagement and retention—key outcomes echoed in research linking integrated behavioral health to better long-term progress7. Next, the discussion will address the retention challenges that remain, and how local solutions are being developed to sustain recovery in San Antonio.
Retention Challenges and Comprehensive Solutions
Understanding Low Retention Patterns
Understanding retention challenges in San Antonio’s opioid treatment system requires examining the city’s unique mix of neighborhoods, local infrastructure, and patient needs. Despite expanded access to medication-assisted treatment, just 27.5% of Medicaid patients remain engaged in care at six months—a pattern seen in clinics serving diverse areas like Harlandale, Stone Oak, the West Side, and Southtown10. Factors contributing to early disengagement often include transportation obstacles, unpredictable work schedules, and limited parking—especially in high-traffic corridors near the Medical Center or along Loop 410.
The complexity of co-occurring mental health conditions adds another layer to retention difficulties. Providers across neighborhoods report that patients with both opioid use disorder and conditions like anxiety or PTSD are less likely to stay in treatment without integrated behavioral health support7, 10. This is not simply a matter of clinical severity; it reflects a gap between the services offered at a typical methadone clinic San Antonio and the comprehensive care that many patients require.
Local testimonials echo these realities. A client from Dignowity Hill shared that balancing work, childcare, and daily appointments downtown made it hard to maintain consistency. In Monte Vista, another participant cited anxiety about public transit and parking as a primary barrier to ongoing involvement. These patterns point to the need for innovative, neighborhood-informed strategies.
Building Sustainable Recovery Systems
Efforts to build truly sustainable recovery systems in San Antonio begin at the neighborhood level, with coordinated solutions that address the city’s distinct challenges. In areas like the West Side, Stone Oak, Harlandale, and Southtown, providers are moving beyond a one-size-fits-all model and actively collaborating with local organizations, transit partners, and community advocates to reduce transportation and scheduling barriers.
A significant investment in outreach—supported by $909,000 in opioid settlement funds—has enabled the deployment of street-based medical services and mobile counseling units in neighborhoods near the River Walk and the Medical Center4. This outreach brings essential services closer to residents who might otherwise forgo care due to parking limitations or safety concerns.
View Transportation and Logistics Strategies
Coordinating care along Loop 410 and near VIA Centro Plaza requires strategic scheduling. Facilities often implement staggered appointment blocks and telehealth options to accommodate peak traffic hours, ensuring professionals can maintain their treatment regimens without compromising workplace responsibilities.
These efforts are supported by evidence showing that integrated, accessible care at a methadone clinic San Antonio improves retention and outcomes, especially when behavioral health and substance use services are coordinated7. By prioritizing local voices and flexible resources, the city is laying the groundwork for a more resilient recovery system.
Accessing Services Across Greater San Antonio
Neighborhoods and Service Availability
Service availability at a methadone clinic San Antonio reflects both the city’s size and the diversity of its neighborhoods. In areas like Southtown, Stone Oak, Harlandale, and Alamo Heights, clinics are strategically located to offer accessible care for individuals seeking medication-assisted treatment. Near major corridors such as Loop 410 and the Medical Center, clinics are especially convenient for those commuting from the North Side or the Loop.
The proximity to landmarks like the Pearl and VIA Centro Plaza means residents of Tobin Hill and the West Side can access services without lengthy travel or significant parking concerns—a vital factor given the city’s busy traffic patterns and reports of limited public transit in certain neighborhoods. Recent data show that only 27.5% of Medicaid patients in San Antonio remain in treatment at six months, with accessibility and safety among the most commonly cited barriers to ongoing care10.
Local testimonials highlight solutions emerging in the community: a Harlandale resident shared how clinic hours near the River Walk made it possible to keep appointments after work, while a Stone Oak peer described group support as essential for maintaining stability. For professionals and providers, understanding these neighborhood-specific dynamics is key to driving sustainable engagement and improved outcomes.
Insurance Coverage and Policy Changes
Insurance coverage and policy changes have had a direct impact on access to care at any methadone clinic San Antonio. Since the Consolidated Appropriations Act of 2024, Medicaid in San Antonio now covers all FDA-approved medications for opioid use disorder, including methadone, with expanded billing options for both supervised and take-home doses6. This policy shift is particularly relevant for neighborhoods like Harlandale, Southtown, and Alamo Heights, where access to affordable coverage remains a deciding factor for ongoing treatment.
The elimination of the Data 2000 waiver has also expanded the pool of prescribers, making it easier for residents in areas such as the Medical Center and West Side to find qualified providers6. Permanent take-home dose flexibilities, now embedded in local Medicaid billing, mean that stable patients—especially those working or living near Loop 410 or VIA Centro Plaza—can reduce daily clinic visits and better manage work and family obligations2.
Despite these advances, retention rates for Medicaid patients remain low, with only 27.5% staying engaged in treatment at six months10. As a result, ongoing advocacy for both policy improvements and local outreach remains essential.
Frequently Asked Questions
How do take-home methadone doses work for working professionals?
For working professionals in San Antonio neighborhoods like Stone Oak, Southtown, and near the Medical Center, recent policy changes have made take-home methadone dosing at a methadone clinic San Antonio much more accessible. Stable patients can now receive up to 28 days of unsupervised doses—after as little as 31 days of consistent treatment—reducing the need for daily clinic visits and making it easier to manage work and family obligations2. Providers use objective criteria to assess stability, including attendance, toxicology screens, and social support. This flexibility is especially helpful for those who navigate heavy traffic on Loop 410 or must coordinate care around unpredictable work schedules. Clinics remain vigilant in monitoring adherence, ensuring both safety and ongoing support.
What happens if someone has both PTSD and opioid use disorder?
When someone experiences both PTSD and opioid use disorder, treatment at a methadone clinic San Antonio requires an integrated approach that addresses both conditions together. Research shows that combining medication-assisted treatment with cognitive behavioral therapy results in significantly better outcomes for individuals facing these co-occurring disorders—especially in reducing drug use and improving daily functioning7. In local neighborhoods like Harlandale, Southtown, and near VIA Centro Plaza, clinics are increasingly offering trauma-informed counseling alongside methadone to support this complex patient group. This dual diagnosis strategy can help stabilize symptoms, support retention in care, and improve overall quality of life, even with the city’s retention challenges10.
Which San Antonio neighborhoods have the easiest access to treatment services?
Neighborhoods like Southtown, Stone Oak, Alamo Heights, Harlandale, and areas near the Medical Center offer some of the easiest access to treatment services at a methadone clinic San Antonio. Clinics in these neighborhoods are positioned near major corridors such as Loop 410 and VIA Centro Plaza, providing convenient options for those commuting from the North Side or The Loop. This strategic placement reduces transportation and parking barriers—issues commonly cited by residents in neighborhoods farther from the city center10. Testimonies from Stone Oak and Harlandale highlight how nearby clinics and flexible scheduling support ongoing engagement. Local traffic and safety patterns remain important considerations for accessibility.
How does Texas Medicaid billing work for methadone treatment?
Texas Medicaid covers methadone treatment at any methadone clinic San Antonio by reimbursing both supervised and take-home doses. Providers bill for in-clinic, supervised administration using the UA modifier, while unsupervised take-home doses require the U1 modifier. Medicaid allows up to 30 take-home doses per 30 days, making it easier for patients in neighborhoods like Harlandale, Southtown, and Stone Oak to balance treatment with daily life. This billing structure supports providers citywide, from clinics near the Medical Center to those off Loop 410, and reflects recent federal mandates expanding MAT coverage in San Antonio6.
What factors contribute to someone leaving treatment early?
Several factors common to San Antonio contribute to early departure from a methadone clinic San Antonio. Transportation barriers are significant, especially for those living in neighborhoods like Harlandale or the West Side, where reliable transit or parking near clinics can be limited. Work and family obligations also compete with treatment schedules, particularly for residents commuting along busy routes such as Loop 410 or to the Medical Center. Safety concerns in certain areas and low integration of mental health support for co-occurring disorders further impact retention. Recent data show only 27.5% of Medicaid patients stay engaged in treatment at six months, underscoring these challenges10.
How has the elimination of the Data 2000 waiver changed prescriber availability?
The elimination of the Data 2000 waiver has significantly increased prescriber availability for medication-assisted treatment at every methadone clinic San Antonio. Previously, only providers with a federal waiver could prescribe buprenorphine, limiting access for residents in neighborhoods like Stone Oak, Harlandale, and the West Side. Now, any clinician with a standard DEA registration can prescribe, which has expanded the local pool of providers and reduced wait times for new patients6. This change is especially impactful in areas near the Medical Center and VIA Centro Plaza, where provider shortages once delayed care. Greater prescriber flexibility is helping clinics meet the city’s rising demand for opioid use disorder treatment.
What role do opioid settlement funds play in expanding local services?
Opioid settlement funds have become a crucial resource for expanding local services at any methadone clinic San Antonio. In fiscal years 2024 and 2025, the city allocated $909,000 from these settlements, targeting medical treatment for street outreach, substance use outreach, harm reduction supplies like Narcan, and stigma-reduction education4. These investments directly benefit neighborhoods such as Harlandale, Southtown, and areas near the Medical Center by increasing the availability of mobile medical teams and outreach workers. As a result, more residents can access support closer to home, even in areas with transportation or parking barriers. Continued use of these funds is expected to address ongoing gaps in care.
Building a Foundation for Long-Term Recovery
As professionals who understand dual diagnosis treatment from both clinical expertise and lived experience, we recognize that sustainable recovery requires comprehensive frameworks addressing the interconnected nature of mental health and substance use challenges. The integrated dual diagnosis treatment model moves beyond traditional single-diagnosis approaches by acknowledging how co-occurring disorders influence and reinforce each other—a reality we’ve witnessed throughout our careers. Effective dual diagnosis treatment demands clinical precision paired with whole-person understanding, creating unique recovery pathways that reflect the complexity inherent in co-occurring disorders.
Evidence-based dual diagnosis treatment protocols form the cornerstone of measurable outcomes, with cognitive behavioral therapy and dialectical behavior therapy providing the therapeutic foundation we know drives results. These modalities work synergistically with medication management at a methadone clinic San Antonio, creating the stability necessary for meaningful progress. Facilities achieving 93% treatment goal achievement rates demonstrate how integrated dual diagnosis treatment approaches outperform fragmented care models—outcomes that validate our understanding of what effective intervention requires.
Beyond clinical interventions, holistic dual diagnosis treatment practices strengthen recovery foundations by addressing physical wellness, spiritual exploration, and community connection—dimensions we understand as critical to long-term sustainability. Mindfulness techniques, nutritional support, and structured routines within dual diagnosis treatment programming help individuals rebuild their relationship with themselves and their environment. The integration of trauma-informed care ensures that underlying experiences contributing to both conditions receive proper attention, while aftercare programming and peer support networks provide ongoing accountability.
References
- Be Well Texas at UT Health San Antonio Major Statewide Expansion. https://news.uthscsa.edu/be-well-texas-at-ut-health-san-antonio-to-lead-major-statewide-expansion-of-opioid-use-disorder-and-recovery-services/
- SAMHSA Methadone Take-Home Flexibilities Extension Guidance. https://www.samhsa.gov/substance-use/treatment/opioid-treatment-program/methadone-guidance
- PMC Effectiveness Methadone versus Buprenorphine Treatment. https://pmc.ncbi.nlm.nih.gov/articles/PMC12182195/
- Be Well Texas San Antonio Targets $909K Opioid Settlement. https://bewelltexas.org/san-antonio-targets-909k-from-opioid-settlement-to-reduce-overdoses/
- PMC Outcomes Medication Assisted Treatment Pilot Program. https://pmc.ncbi.nlm.nih.gov/articles/PMC8722086/
- TMHP Updated Benefit Information MAT Services Texas Medicaid. https://www.tmhp.com/news/2020-02-07-updated-benefit-information-mat-services-texas-medicaid-march-1-2020
- PMC Integrating Treatment Co-Occurring Mental Health Conditions. https://pmc.ncbi.nlm.nih.gov/articles/PMC6799972/
- City of San Antonio Declares Overdoses Public Health Crisis. https://www.sa.gov/Directory/News-Releases/City-of-San-Antonio-Declares-Overdoses-a-Public-Health-Crisis
- NCBI Overview Medications Opioid Use Disorder. https://www.ncbi.nlm.nih.gov/books/NBK574908/
- JAMA Opioid Treatment Programs Medicaid Patient Retention. https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2844211
