Key Takeaways
- Neighborhoods Served: Comprehensive access across South Congress, Hyde Park, Mueller, East Riverside, and The Domain.
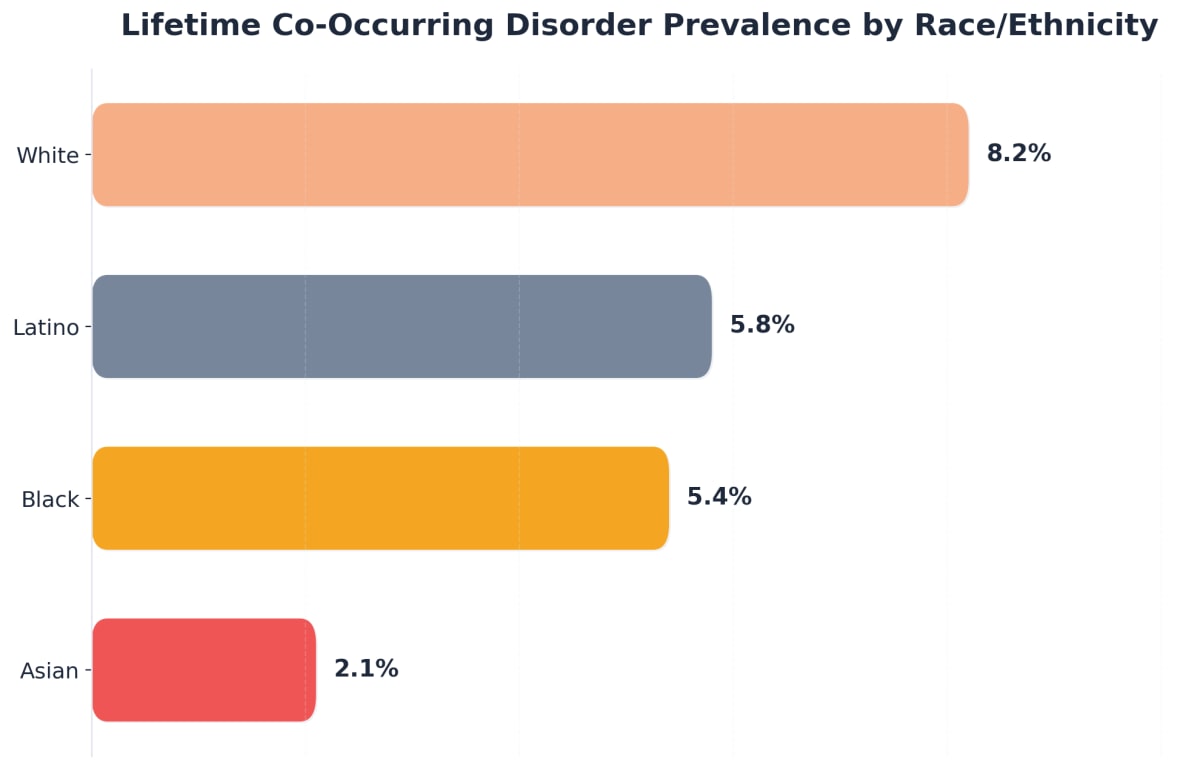
- Local Impact: Approximately 7.3% of Austin residents experience co-occurring disorders, highlighting the need for accessible, specialized care.
- Strategic Locations: Facilities are situated near major landmarks like Sixth Street and Lady Bird Lake for optimal accessibility.
- Transit Integration: Programs are designed around Austin’s infrastructure, offering easy access via I-35, Mopac, and Capital Metro routes.
- Core Service: The intensive outpatient program Austin model provides flexible, evidence-based dual diagnosis treatment tailored for working professionals.
Dual Diagnosis Care and the Intensive Outpatient Program Austin Metro Needs
Bridging Recovery Across Austin Communities
Austin’s approach to dual diagnosis care is as diverse as its neighborhoods—encompassing South Congress, Hyde Park, Mueller, Zilker, and East Riverside. Central locations near Sixth Street or proximity to Lady Bird Lake make it possible for individuals to access services without excessive commute times, even during rush hour on Mopac or I-35. For clinical professionals, referring clients to an intensive outpatient program Austin ensures a continuity of care from the tech corridors of The Domain to the quieter residential streets of Allandale.
Client experiences frequently highlight the importance of this geographic accessibility. When treatment integrates seamlessly into daily life, retention rates improve significantly.
“Austin traffic can be unpredictable, but having my sessions right near campus meant I never missed out. Walking home after group in Zilker was never a worry.” — Program Participant
These narratives reflect the city’s commitment to neighborhood-focused treatment. Services are thoughtfully distributed for accessibility, whether clients arrive by Capital Metro or utilize on-site parking in neighborhoods like Mueller and East Riverside. Recent studies confirm that integrated intensive outpatient programs provide outcomes on par with inpatient care for most individuals with co-occurring disorders, allowing them to stay connected to their home communities while receiving evidence-based support.1
The next section will address why these programs are uniquely suited to meet Austin’s evolving treatment landscape.
Why IOPs Meet Austin’s Treatment Needs
Austin’s rapid population growth and evolving urban landscape have made flexible, community-based care essential for those managing co-occurring disorders. The intensive outpatient program Austin model meets this clinical need by allowing individuals to participate in structured, evidence-based treatment while maintaining their daily responsibilities in neighborhoods like South Lamar, Brentwood, Windsor Park, Travis Heights, and Clarksville.
With Austin’s unpredictable traffic patterns, programs located near landmarks such as Barton Springs, the Texas Capitol, or along accessible corridors like I-35 and Mopac are vital for reducing barriers to attendance. When coordinating care, professionals often utilize specific digital queries—such as typing intensive outpatient program Austin into referral databases—to locate the most geographically appropriate services for their clients.
Research shows that for individuals with co-occurring mental health and substance use conditions, intensive outpatient programs achieve clinical outcomes on par with inpatient care—especially when treatment is integrated and accessible within the community. This alignment is crucial for Austin’s diverse population, where nearly 7.3% of residents are estimated to experience co-occurring disorders in their lifetime.1,4
- East Austin & North Loop: Accessible via public transit, minimizing disruptions to work.
- Riverside Corridor: Offers flexible scheduling for students and young professionals.
- Brentwood & Travis Heights: Walkable locations that foster community integration and reduce isolation.
“Being able to walk to evening sessions after work in Brentwood made all the difference. The program’s location near the hike-and-bike trail in Travis Heights meant I could fit in self-care before group.” — Program Participant
Next, we will examine the evidence-based framework that underpins effective co-occurring condition treatment in Austin.
Evidence-Based Framework for Co-Occurring Conditions
Integrated Treatment Models in Practice
Integrated treatment models are central to the success of any intensive outpatient program Austin, especially for individuals presenting with co-occurring substance use and mental health disorders. In practice, these programs combine evidence-based therapies with coordinated psychiatric care, peer support, and frequent outcome monitoring. Austin’s integrated models often include collaborative teams—therapists, counselors, and medical professionals—who work together to develop and adapt care plans.
| Therapeutic Modality | Clinical Focus | Application in IOP Setting |
|---|---|---|
| Cognitive Behavioral Therapy (CBT) | Identifying and modifying maladaptive thought patterns. | Core group sessions focusing on relapse prevention and coping strategies. |
| Dialectical Behavior Therapy (DBT) | Emotional regulation and distress tolerance. | Skills training groups tailored for co-occurring anxiety or bipolar traits. |
| Eye Movement Desensitization and Reprocessing (EMDR) | Trauma processing and neural integration. | Individualized sessions addressing underlying PTSD contributing to substance use. |
This multidisciplinary approach allows for seamless adjustments in response to changes in symptom severity, making it especially effective for those living in neighborhoods like Bouldin Creek, Cherrywood, and Old West Austin, where community ties are strong. Integrated intensive outpatient programs in Austin have demonstrated high client satisfaction, with recent studies noting mean satisfaction scores between 9.17 and 9.35 out of 10.2
Telehealth and hybrid models now extend access to those in Rosedale, Govalle, and surrounding areas, minimizing commute time and reducing barriers to participation. Integrated treatment models remain the foundation for positive outcomes, setting the stage for trauma-informed and holistic approaches.
Trauma-Informed Modalities and Holistic Care
Trauma-informed modalities and holistic care have become defining features of the intensive outpatient program Austin landscape, particularly for those experiencing complex co-occurring disorders. In neighborhoods from South Congress and Westlake to Holly and Oak Hill, these programs recognize that trauma is frequently intertwined with substance use and mental health challenges. Austin’s clinics often integrate evidence-based trauma therapies alongside core cognitive-behavioral approaches.
This comprehensive framework allows participants to process traumatic events in a safe and structured setting, increasing engagement and reducing relapse risk. Holistic care further supports this neurobiological healing process. Many programs supplement traditional therapy with mindfulness practices, meditation, yoga, and nutrition support.4
“Yoga classes near Lady Bird Lake helped me find calm before group, and the nutrition sessions gave me energy I hadn’t felt in years.” — Holly Neighborhood Resident
These modalities help clients from neighborhoods like Crestview and Tarrytown build emotional regulation skills, manage stress, and reconnect with their physical wellbeing—key elements in sustaining long-term recovery. Recent research highlights the benefits of such holistic integration, showing improved distress tolerance and neural repair among participants.4
By prioritizing trauma-informed and holistic approaches, the model addresses the full spectrum of client needs. The next section explores what professionals and participants can expect in terms of program structure and scheduling.
What to Expect from an Intensive Outpatient Program Austin
Structured Schedules and Telehealth Options
Austin’s intensive outpatient program landscape is shaped by the rhythms of neighborhoods like South Lamar, East Cesar Chavez, Allandale, and North Burnet. Participants often find that structured schedules accommodate the city’s active professional and creative scenes. Centers near landmarks such as the Austin Community College Highland campus or the North Loop district provide convenient options for those commuting via I-35 or Capital Metro, reducing the impact of downtown congestion.
For clinical reference, a standard intensive outpatient program Austin schedule might look like this within a facility’s management system:
| Day | Schedule |
|---|---|
| Monday | 18:00 – 21:00 (Group Therapy: Relapse Prevention) |
| Wednesday | 18:00 – 21:00 (Group Therapy: Emotional Regulation) |
| Thursday | 18:00 – 19:00 (Individual Counseling) |
| Saturday | 10:00 – 12:00 (Holistic Care: Yoga/Mindfulness) |
Recent developments include the rapid expansion of telehealth. This approach allows individuals in neighborhoods as varied as Travis Heights, Windsor Park, or near Mueller to attend therapy, group sessions, and psychiatric check-ins without needing to navigate parking limitations near The Domain. Research shows that telehealth and hybrid options not only improve access but also maintain clinical effectiveness for individuals with co-occurring disorders.1
Testimonials from North Burnet and East Cesar Chavez highlight how telehealth enabled professionals to stay engaged despite demanding work schedules. One participant noted, “Virtual evening groups let me participate from home after a long day at the office.” Another shared, “Having the option to alternate between in-person and online sessions meant I never had to miss out because of traffic or childcare.”

Appropriate Treatment Matching Criteria
Appropriate treatment matching within the intensive outpatient program Austin system is rooted in a careful, individualized assessment process that reflects both clinical needs and the realities of local living. Professionals in Austin routinely evaluate multiple dimensions of a client’s presentation to ensure optimal placement.
- Symptom Severity: Assessing the acuity of both mental health and substance use disorders.
- Functional Stability: Evaluating the client’s ability to maintain employment or family responsibilities.
- Withdrawal Risk: Ensuring the individual does not require 24-hour medical detoxification.
- Environmental Support: Confirming stable housing in areas like Central Austin, East Austin, or South Menchaca.
Research consistently shows that outcomes are strongest when participants are matched to the appropriate level of care from the outset, yielding similar reductions in substance use and improvements in overall functioning as inpatient programs for those who meet criteria. High-need cases are referred to higher-intensity services, while flexible scheduling and telehealth expansion have increased access for professionals in Clarksville, students in West Campus, and parents in Windsor Park.1
A local case from East Austin highlights this approach: a participant shared that being matched to IOP, rather than a more restrictive setting, allowed her to care for her children and attend sessions near Boggy Creek. This underscores the city’s commitment to individualized, neighborhood-based care. Next, the focus turns to long-term recovery strategies and Austin’s continuing care resources.
Long-Term Recovery and Continuing Care Systems
Sustainable recovery from co-occurring disorders extends far beyond the completion of an intensive outpatient program Austin, requiring structured continuing care systems that support long-term clinical outcomes. Professionals working in dual diagnosis treatment understand that the transition from intensive structure to ongoing maintenance represents a critical juncture where relapse risk intensifies without appropriate support frameworks.
The architecture of effective continuing care begins during program participation itself, with transition planning integrated throughout the intensive treatment phase rather than introduced as an afterthought. Clinical teams develop personalized maintenance protocols that identify high-risk situations, establish response strategies, and outline specific touchpoints for ongoing professional support. Regular monitoring through scheduled clinical contacts allows for real-time intervention when symptom patterns shift.
Centers like Continuum Outpatient Center structure their continuing care systems to provide seamless transitions to less intensive maintenance programming, preserving therapeutic relationships while adjusting treatment frequency. Alumni programming serves essential functions beyond peer support, creating structured environments where individuals maintain accountability to recovery principles. These programs function as early warning systems, with peer networks often detecting subtle changes in presentation before clinical deterioration becomes apparent.
Psychiatric continuity remains non-negotiable for individuals whose co-occurring disorders include conditions requiring pharmacological management. Telehealth integration has fundamentally transformed continuing care accessibility, eliminating logistical barriers that previously compromised treatment engagement. Furthermore, family system involvement addresses the relational dynamics that significantly influence long-term outcomes, ensuring that individual recovery occurs within a supportive interpersonal context.
Wellness practice integration—including mindfulness applications, movement therapies, nutritional strategies, and stress regulation techniques—sustains the holistic framework central to effective programming, supporting neurobiological recovery processes and building resilience against chronic stress.
Frequently Asked Questions
Do intensive outpatient programs serve neighborhoods throughout the Austin metro area?
Yes, intensive outpatient program Austin services are delivered across the entire metro area, reaching neighborhoods such as Mueller, South Congress, Hyde Park, East Riverside, and North Loop. Many programs are strategically located near local landmarks—like Sixth Street, The Domain, or the UT campus—making them accessible for residents navigating Austin’s unique traffic flows and parking concerns. Telehealth options further extend access, allowing participation from more remote or underserved areas. Research confirms that the expansion of intensive outpatient program Austin models, both in-person and virtually, has significantly increased reach and improved outcomes for individuals with co-occurring disorders citywide.1
How does insurance coverage work for dual diagnosis intensive outpatient programs in Texas?
Insurance coverage for dual diagnosis intensive outpatient program Austin services is governed by federal laws, including the Mental Health Parity and Addiction Equity Act (MHPAEA), which requires most health insurers to provide the same level of coverage for mental health and substance use treatment as for other medical care. In practice, this means many Austin-area residents—whether in neighborhoods like Mueller, South Lamar, or North Loop—can access IOPs using commercial insurance, Medicaid, or employer-sponsored plans. However, network adequacy and specific coverage details can vary widely, so professionals should verify benefits, preauthorization requirements, and out-of-pocket responsibilities for each individual case. Some programs also offer support navigating insurance paperwork and appeals. This approach ensures that those needing dual diagnosis care in Texas are more likely to obtain appropriate, evidence-based treatment without unnecessary delays.9
What role do peer support and 12-step programs play in sustaining recovery after intensive outpatient treatment?
Peer support and 12-step programs play a vital role in sustaining recovery after completing an intensive outpatient program Austin. Involvement in these groups—whether in-person meetings in neighborhoods like Hyde Park or virtual sessions accessible citywide—provides ongoing accountability, encouragement, and a sense of community. Research highlights that weekly 12-step participation is associated with a 77.7% abstinence rate from illicit drugs at 24 months post-treatment, nearly double the rate of those not participatin. For alcohol use, any level of 12-step involvement increases abstinence rates to 68%, compared to 38.8% without such support. These outcomes underscore how local peer networks and structured support groups are essential elements of long-term recovery for individuals with co-occurring disorders.8
Can working professionals maintain employment while participating in an intensive outpatient program?
Yes, working professionals in Austin often maintain employment while participating in an intensive outpatient program Austin. Most programs offer flexible scheduling with morning, afternoon, or evening sessions to accommodate standard work hours. The rise of telehealth and hybrid models means professionals can attend therapy or group sessions from home or the office, reducing the need to navigate traffic near The Domain or Downtown and minimizing time away from work. Research shows that this flexibility enables individuals to receive evidence-based care without disrupting their careers, and clinical outcomes remain on par with inpatient treatment for appropriately matched participants.1
How do telehealth options compare to in-person intensive outpatient sessions for treatment effectiveness?
Telehealth options for intensive outpatient program Austin delivery have become widely utilized, particularly in neighborhoods where traffic congestion or limited parking—such as The Domain or Downtown—can pose barriers to in-person attendance. Research indicates that telehealth and hybrid IOP models maintain clinical effectiveness equivalent to traditional in-person sessions, showing comparable reductions in substance use and improvements in mental health outcomes for individuals with co-occurring disorders. Professionals report high satisfaction with the flexibility telehealth offers, especially for participants in areas like Windsor Park or East Riverside who juggle work and family commitments. The ability to attend group therapy, individual counseling, and psychiatric check-ins remotely has increased retention and engagement without sacrificing treatment quality. Both modalities, when matched to participant needs, support positive, evidence-based outcomes.1
What are the completion rates for intensive outpatient programs and factors that support retention?
Completion rates for intensive outpatient program Austin services vary, but research suggests that retention improves significantly when participants experience strong peer support, accessible locations, and individualized care planning. Nationally, IOP completion rates often range from 50% to 70%, with higher rates observed in programs that integrate regular outcome tracking and robust continuing care. In Austin, factors like neighborhood accessibility—such as locations in Hyde Park, South Lamar, and near The Domain—reduce barriers related to transportation and scheduling. Active engagement with 12-step groups and alumni networks has also been linked to higher completion rates and sustained recovery. For professionals, fostering a sense of community and flexible participation options is key to supporting retention.1,2,8
Accessing Dual Diagnosis IOP Services in Austin
Understanding how continuing care systems support sustained wellness naturally leads to the practical question of accessing these services. Connecting with an intensive outpatient program austin begins with understanding available pathways to care throughout the San Antonio and Austin metropolitan areas. Many individuals start by consulting with primary care physicians or mental health professionals who can provide referrals to specialized programs.
The region provides multiple access points for those seeking dual diagnosis services. Facilities like Ripple Ranch Recovery Center, located on a 20+ acre property in Spring Branch, Texas, serve both the San Antonio and Austin metropolitan areas with comprehensive dual diagnosis treatment. Through their partnership with Continuum Outpatient Center, they offer flexible intensive outpatient programs that integrate mental health and addiction care. Telehealth assessments have expanded availability, allowing initial consultations without travel barriers—particularly valuable for working professionals seeking discrete treatment options.
Most services require a brief assessment process covering substance use history, mental health symptoms, and previous treatment experiences. This evaluation ensures proper placement and identifies any medical considerations requiring attention before beginning outpatient services. Providers typically conduct these assessments with sensitivity to the complexity of co-occurring conditions, recognizing that integrated evaluation leads to more effective treatment planning.
Insurance verification typically happens during initial contact, clarifying coverage details and out-of-pocket responsibilities. Centers like Ripple Ranch Recovery accept most major insurance plans, working to ensure accessibility for those seeking an intensive outpatient program Austin and surrounding areas. Treatment coordinators guide individuals through enrollment steps, scheduling flexibility, and program expectations, focusing on reducing barriers and creating pathways to specialized, coordinated care.
Contact rippleranch.com today to learn how our evidence-based treatment approaches can help you reclaim your health, restore your relationships, and build the fulfilling life you deserve.References
- Substance Abuse Intensive Outpatient Programs: Assessing the Evidence. https://pmc.ncbi.nlm.nih.gov/articles/PMC4152944/
- Clients’ Experiences and Satisfaction with an Integrated Intensive Outpatient Program. Actas Esp Psiquiatr. 2025;53(2):340–347. https://pmc.ncbi.nlm.nih.gov/articles/PMC11898248/
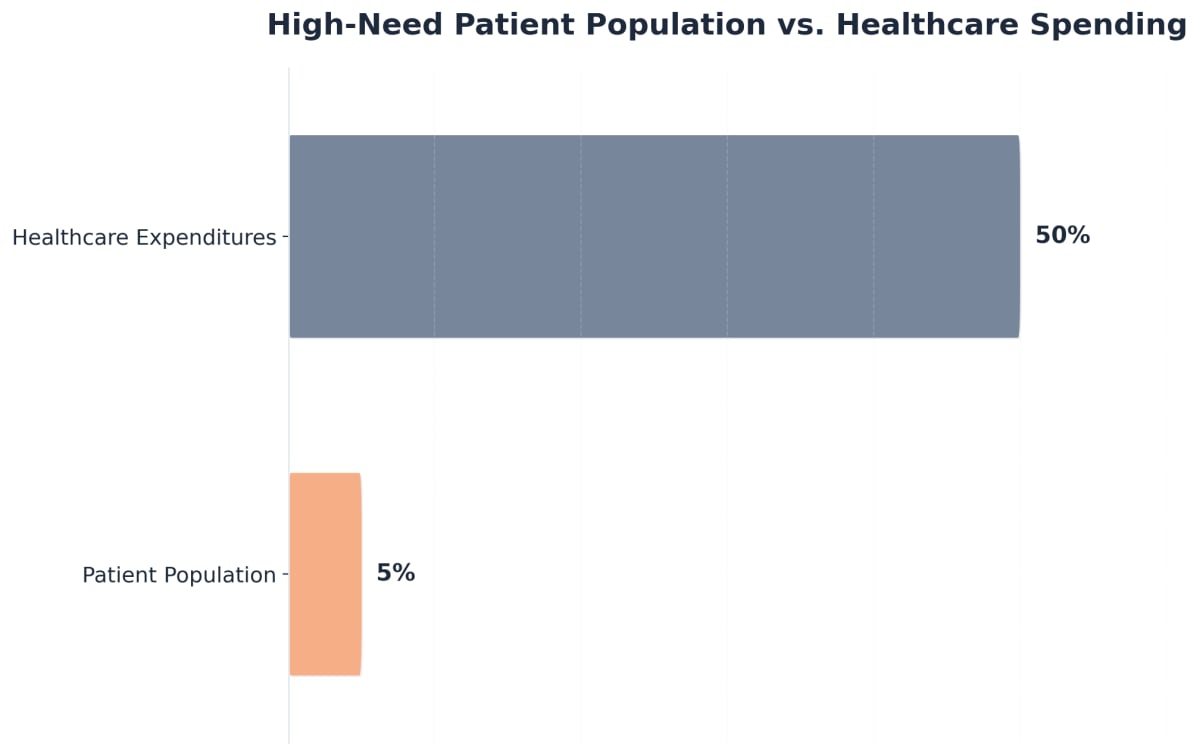
- A systematic review of intensive outpatient care programs for high-need, high-cost patients. Transl Behav Med. 2020;10(5):1187-1199. https://pubmed.ncbi.nlm.nih.gov/33044534/
- Prevalence, Patterns, and Correlates of Co-Occurring Substance Use and Mental Disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC3327759/
- Co-Occurring Disorders and Other Health Conditions. https://www.samhsa.gov/substance-use/treatment/co-occurring-disorders
- Cognitive-Behavioral Therapy for Substance Use Disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC2897895/
- The Continuing Care Model of Substance Use Treatment. https://pmc.ncbi.nlm.nih.gov/articles/PMC4007701/
- Benefits of peer support groups in the treatment of addiction. https://pmc.ncbi.nlm.nih.gov/articles/PMC5047716/
- The Mental Health Parity and Addiction Equity Act (MHPAEA). https://www.cms.gov/marketplace/private-health-insurance/mental-health-parity-addiction-equity
- Chapter 3—Family Counseling Approaches. https://www.ncbi.nlm.nih.gov/books/NBK571088/
