Key Takeaways: Assessing Your Recovery Needs
- Evaluate Your Severity: If you experience intense cravings, withdrawal symptoms, or have co-occurring mental health conditions, professional medical detox is strongly recommended over self-management.
- Understand the Timeline: While acute withdrawal typically lasts 1–2 weeks, true recovery is a long-term process requiring months of behavioral therapy and lifestyle adjustment.
- Prioritize Integrated Care: Success rates improve significantly when treatment addresses both substance use and underlying trauma or mental health issues simultaneously.
- Action Step: If you are unsure where to start, schedule a professional assessment to determine if inpatient or outpatient care best suits your safety needs and daily responsibilities.
Understanding Stimulant Use and Stimulant Detox San Antonio
What Defines Stimulant Addiction Today
Stimulant addiction is defined as a pattern of compulsive use of substances like cocaine, methamphetamine, or prescription stimulants, persisting despite harmful consequences to health, relationships, and daily functioning. Unlike occasional or prescribed use, addiction is marked by a strong urge to use, increasing tolerance, and withdrawal symptoms when use is reduced or stopped. This cycle can affect anyone, regardless of age or background; what begins as experimentation or academic pressure can lead to significant changes in brain chemistry.
Medical professionals classify this as a substance use disorder, meaning the brain and behavior adapt in ways that make quitting extremely difficult without structured support. For example, nearly 59% of all overdose deaths in the United States between January 2021 and June 2024 involved stimulants, underscoring the severity of this issue. The presence of intense cravings and failed attempts to cut back are signs that someone might need specialized help, such as a stimulant detox San Antonio program.1
Recognizing the problem is the essential first step toward recovery. With research highlighting how brain changes and environmental stressors contribute to this disorder, compassion and evidence-based care are vital for healing.5
The Rising Crisis: Statistics and Trends
The crisis surrounding stimulant use has escalated, with data revealing a concerning upward trend in both misuse and overdose deaths. The following data highlights the urgency of the situation between 2011 and 2023:
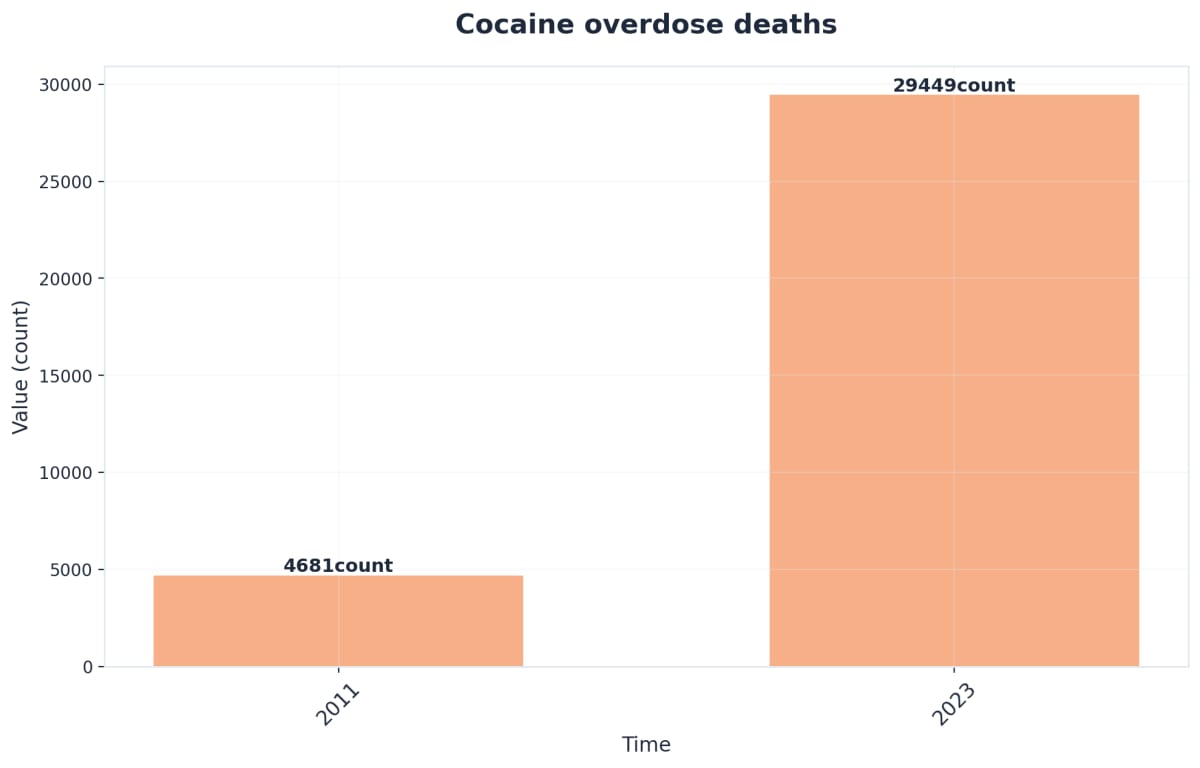
| Substance Type | Increase in Fatal Overdoses (2011–2023) | Key Demographic Concern |
|---|---|---|
| Cocaine | ~530% Increase | High polysubstance involvement |
| Psychostimulants (e.g., Methamphetamine) | ~1,400% Increase | Rapidly rising across all age groups |
| Prescription Stimulants | Variable | Significant misuse among young adults (18–25) |
Among young adults aged 18 to 25, stimulant misuse remains a critical concern. Although the percentage of young adults misusing central nervous system (CNS) stimulants declined from 6.7% in 2021 to 4.7% in 2024, the absolute number of individuals affected remains significant. Stimulants are now implicated in more than one-third of youth opioid overdose deaths, demonstrating the dangerous overlap between different substances.2,3
Disparities across demographics further complicate this trend, with Black and Latino communities often facing additional barriers to accessing care. These statistics underscore the need for timely interventions like stimulant detox San Antonio to help families and professionals respond effectively.7
Why Professional Stimulant Detox San Antonio Makes the Difference
The Neuroscience Behind Recovery Success
Recovery is not simply a matter of willpower; it is a process rooted in brain chemistry. Regular use of stimulants like methamphetamine or cocaine intensely activates the brain’s reward system, leading to powerful cravings and a diminished response to everyday pleasures. This rewiring makes stopping use incredibly challenging without specialized support.
Professional treatment programs are designed to address these neurobiological changes. Research shows that without structured support, only about 15% of people trying to quit methamphetamine remain abstinent after three months, and that number drops to just 5% after three years without rehabilitation. Evidence-based therapies work by helping the brain relearn how to respond to positive, healthy rewards, gradually reducing cravings and relapse risk.4,5
Addressing Co-Occurring Mental Health Needs
When seeking help, addressing co-occurring mental health needs is just as vital as managing withdrawal. Nearly 50% of individuals with a substance use disorder also experience a mental health condition such as anxiety, depression, or post-traumatic stress disorder (PTSD). If these underlying issues are overlooked, the risk of relapse significantly increases.6
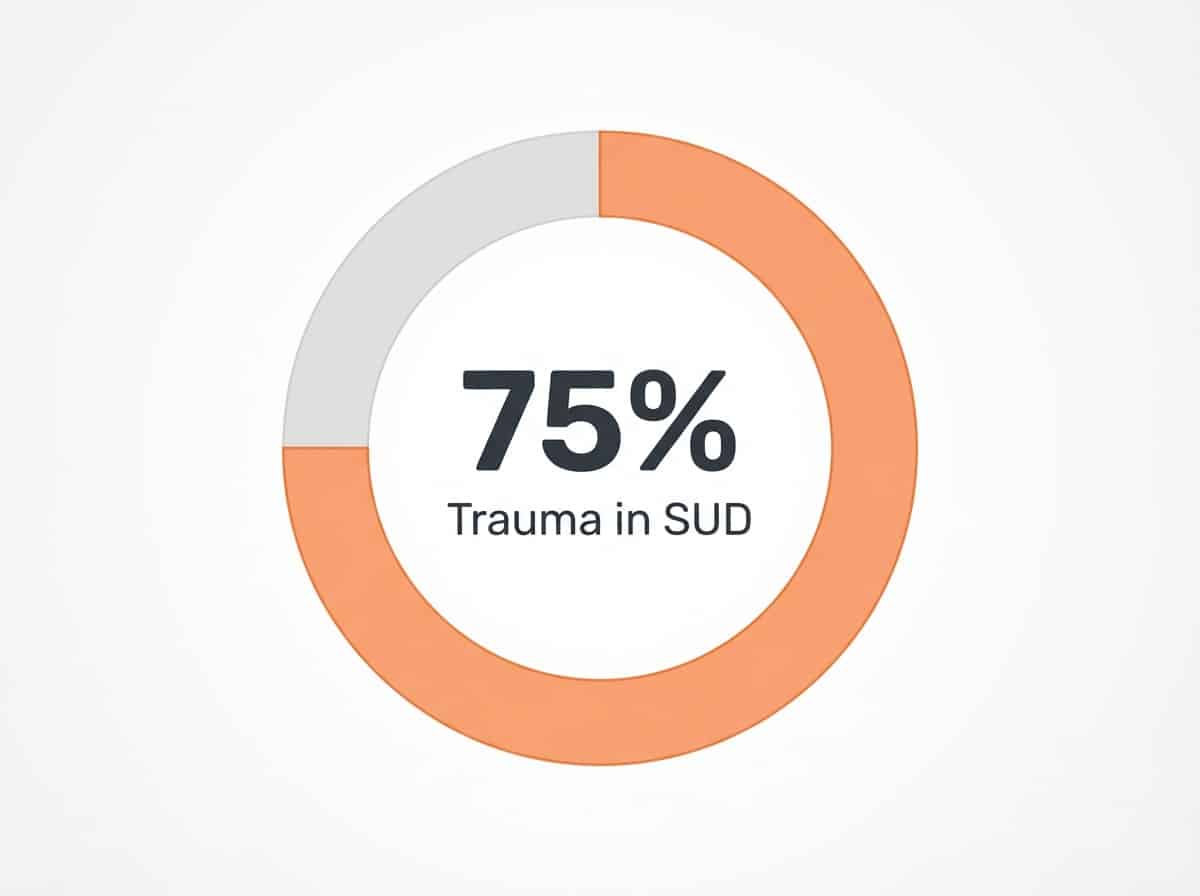
“Up to 75% of people in substance use treatment have a history of trauma, and up to one-third meet criteria for PTSD.”8
Effective professional treatment integrates mental health support alongside substance use care. This means thorough assessment at intake and ongoing collaboration between addiction specialists, therapists, and medical providers. Integrated care plans may include individual therapy, psychiatric support, group sessions, and medication management tailored to each person’s unique needs.

Evidence-Based Approaches to Stimulant Recovery
Behavioral Therapies That Create Lasting Change
Behavioral therapies are the foundation of long-term change for individuals seeking stimulant detox San Antonio. Two approaches stand out for their proven impact: contingency management and cognitive behavioral therapy (CBT). To ensure you are receiving quality care, look for these key elements in a program:
- Evidence-based approaches: Utilization of contingency management or CBT.
- Individualized planning: Treatment tailored to your specific history and needs.
- Trauma-informed care: Integration of trauma support when relevant.
- Progress monitoring: Regular adjustments to the care plan based on your growth.
- Skill-building: Focus on relapse prevention and coping mechanisms.
Contingency management uses motivational incentives to reinforce positive behaviors, showing an odds ratio of 2.29 for achieving abstinence at 12 weeks compared to standard care. Meanwhile, CBT helps individuals recognize thought patterns and triggers, allowing them to navigate high-risk situations and set healthy goals.4,5
The Role of Medical Support in Detox
Medical support plays a vital role in the detox process, particularly for those facing intense withdrawal symptoms. While there are no FDA-approved medications specifically for stimulant withdrawal, professional medical teams monitor vital signs and manage symptoms like severe anxiety or agitation. Use the following checklist to determine if medical support is necessary for your situation:
- Severe Symptoms: Are you experiencing agitation, paranoia, or suicidal thoughts?
- Mental Health History: Do you have co-occurring conditions like depression or anxiety?
- Past Complications: Have you had medical issues during previous withdrawal attempts?
- Polysubstance Use: Are you using stimulants in combination with other drugs?
- Environment: Do you lack a stable, safe living environment or support system?
A medically supported environment offers 24/7 care and immediate access to interventions, such as medication to ease sleep problems or manage acute psychological distress. This level of care is critical for safety and stability, allowing you to focus on the initial steps of healing without the immediate risk of medical emergencies.4
Building Your Personalized Recovery Path
Recovery from substance use disorder is deeply personal. Creating a personalized recovery path means acknowledging your unique circumstances, challenges, and strengths while exploring treatment options that align with your specific needs and goals.
Your journey begins with an honest assessment of where you are today. This includes understanding the severity of your substance use, identifying co-occurring mental health conditions, recognizing your support system, and acknowledging any barriers you might face. A comprehensive evaluation by treatment professionals helps identify which level of care—whether inpatient, outpatient, or residential—best matches your current situation.
The most effective approach incorporates multiple evidence-based treatments tailored to your preferences. Consider these examples of personalized care:
- Anxiety & Addiction: Combining Cognitive Behavioral Therapy (CBT) with mindfulness practices.
- Trauma History: Prioritizing EMDR therapy alongside standard counseling.
- Holistic Needs: Integrating yoga, exercise, and nutrition planning with medication-assisted treatment.
Research shows that individualized treatment plans increase completion rates by up to 40% compared to one-size-fits-all programs. Your recovery plan should fit realistically into your life while providing the intensity of support necessary for healing. Whether you need the flexibility of an intensive outpatient program or the structure of residential treatment, the key is remaining committed to finding what truly works for you.
Frequently Asked Questions
How do I choose between inpatient and outpatient stimulant addiction treatment programs?
Choosing between inpatient and outpatient stimulant addiction treatment depends on your needs, safety, and support system. Inpatient care offers a structured, 24/7 environment with medical supervision—this approach is ideal if you have a history of severe withdrawal symptoms, co-occurring mental health conditions, or limited support at home. Outpatient options work well if you have a stable living situation, strong external support, and mild to moderate symptoms. Research shows that integrating behavioral therapies and ongoing support in both settings can enhance recovery outcomes. If you’re unsure, a professional assessment is the best first step to determine which stimulant detox San Antonio program is the right fit for you.4
What happens if I experience a setback during my recovery from stimulant addiction?
Experiencing a setback—such as returning to stimulant use—does not mean failure. Recovery is a process, and setbacks are a common part of that journey. The most effective response is to reach out for support as soon as possible, whether from your care team, a peer in recovery, or a trusted loved one. Programs offering stimulant detox San Antonio emphasize that promptly reconnecting with treatment and discussing what led to the setback can help adjust your recovery plan and reduce the risk of future recurrence. Many people find that addressing triggers, stressors, or mental health needs with professional guidance leads to renewed progress. Remember, each setback is an opportunity to learn, adapt, and continue healing.5
Can family members participate in my stimulant addiction treatment?
Yes, family members can play a vital role in your stimulant addiction treatment. Many programs offering stimulant detox San Antonio actively encourage family involvement throughout the recovery process. Family support can improve treatment engagement, reduce substance use, and help build healthier relationships. Studies show that family-based approaches lead to better outcomes than individual treatment alone, with benefits lasting well beyond the initial phase of care. Family participation might include attending educational sessions, joining therapy groups, or taking part in family counseling. These opportunities allow loved ones to learn about addiction, develop effective communication skills, and offer encouragement as you move forward in recovery.9
How long does stimulant addiction recovery typically take?
The duration of stimulant addiction recovery varies for each person, but research suggests it is a long-term process rather than a set timeline. Initial withdrawal symptoms after stimulant detox San Antonio typically last one to two weeks. However, ongoing recovery—including therapy, support groups, and lifestyle changes—often extends for months or even years. Studies indicate that without professional treatment, only about 15% of people remain abstinent at three months, highlighting the importance of continued support for lasting change. Individual factors like co-occurring mental health needs, family involvement, and commitment to recovery all influence the timeframe.4
Will my insurance cover stimulant addiction treatment services?
Most insurance plans are required by federal law to provide the same level of coverage for behavioral health services—including stimulant detox San Antonio—as they do for other medical conditions. This is due to mental health parity regulations, which aim to ensure that substance use treatment is not subject to stricter limits or higher costs than physical health care. However, the extent of coverage can vary depending on your specific plan, network providers, and any prior authorization requirements. Recent policy updates have strengthened parity rules, but some individuals may still encounter challenges with reimbursement or access. It’s always best to contact your insurance company directly and ask about specific coverage for stimulant addiction treatment.10
What if I have both trauma and stimulant addiction issues?
If you are facing both trauma and stimulant addiction, know that you are not alone—up to 75% of people seeking substance use treatment have experienced significant trauma. When selecting a stimulant detox San Antonio program, look for one that offers trauma-informed care. This approach means your treatment team understands how past traumatic experiences can affect your recovery and will tailor support to help you feel safe, respected, and empowered. Integrated care addresses both trauma and stimulant use together, which research shows leads to better outcomes than treating each issue separately. Healing is possible with the right support and compassionate guidance.8
How do I maintain my recovery after completing a stimulant addiction treatment program?
Maintaining your recovery after completing a stimulant addiction treatment program involves a blend of ongoing support, healthy routines, and a strong personal commitment. Staying engaged with therapy, joining peer support groups, and building a daily structure—including work, hobbies, or volunteering—can reinforce new habits and reduce risk of relapse. Recovery research highlights that continued connection to care, family involvement, and regular goal-setting all strengthen long-term outcomes. If you completed stimulant detox San Antonio, consider outpatient programs or alumni groups for ongoing guidance. Practicing self-care, reaching out for help early when challenges arise, and celebrating progress—no matter how small—are essential steps for lasting recovery.9
Taking the First Step Toward Healing
Once you understand that recovery can be tailored to your needs, the next step is reaching out for that personalized support. Recovery begins with a single, courageous decision to seek help. That first step might feel overwhelming, but it represents a powerful commitment to personal wellness and a healthier future. The journey often begins with a phone call to an addiction counselor, a visit to a treatment center for an initial consultation, or a conversation with a primary care physician who can provide referrals.
Reaching out to treatment professionals doesn’t require having all the answers. When contacting potential providers, consider asking specific questions:
- What treatment approaches do they offer?
- What does a typical day in their program look like?
- Do they accept your insurance or offer payment plans?
- How do they handle co-occurring mental health conditions?
These conversations provide valuable insights into what recovery looks like and help determine which approaches align best with individual needs and circumstances.
Support systems provide essential encouragement during this transitional period. Whether connecting with trusted friends, family members, or professional counselors, having people who understand the journey makes the process less isolating. Many treatment centers offer free confidential assessments to help determine the most appropriate level of care, and national hotlines like SAMHSA’s National Helpline (1-800-662-4357) provide 24/7 support and local treatment referrals.
Contact rippleranch.com today to learn how our evidence-based treatment approaches can help you reclaim your health, restore your relationships, and build the fulfilling life you deserve.
References
- NIDA: National Overdose Awareness Day – Prescription Stimulants as Emerging Threat. https://www.nida.nih.gov/news-events/news-releases/2024/05/national-overdose-awareness-day-prescription-stimulants-emerging-threat
- SAMHSA NSDUH Data Brief: Trends in Substance Use among Young Adults (2024). https://www.samhsa.gov/data/sites/default/files/reports/rpt56978/2024-nsduh-data-brief-young-adult.pdf
- NIDA: Opioid Overdose Crisis – Polysubstance and Stimulant Co-involvement. https://www.nida.nih.gov/research-topics/opioids/opioid-overdose-crisis
- NIDA Research Report: Treatment of Methamphetamine Addiction. https://www.nida.nih.gov/publications/research-reports/treatment-methamphetamine-addiction
- APA: Substance Use Disorders – Understanding and Recovery. https://www.apa.org/science/about/psa/substance-use
- NIMH: Substance Use Disorders and Mental Health. https://www.nimh.nih.gov/health/topics/substance-use-disorders/index.shtml
- NIH: Racial-Ethnic Disparities in Substance Abuse Treatment. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3665009/
- NIH: Trauma-Informed Care Framework for Behavioral Health. https://www.ncbi.nlm.nih.gov/books/NBK207195/
- NIH: Family Involvement in Treatment and Recovery for Substance Use Disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC8380649/
- APA Policy Updates: Access to Mental Health Care and Insurance Parity. https://updates.apaservices.org/new-policies-affecting-access-to-mental-health-care
- Source 10. not_provided
