Key Takeaways: Your Decision Guide
- Assess Your Needs: If you experience both persistent low mood and substance cravings, integrated depression rehab is statistically more effective than treating conditions separately.
- Evaluate the Program: Use the “Integrated Care Checklist” below to ensure your provider offers a single, coordinated team rather than siloed services.
- Plan for Investment: Expect a 4–8 week timeline for meaningful improvement and prepare for costs ranging from $1,500 (outpatient) to $30,000 (residential), depending on the level of care required.
- Immediate Action: If safety is at risk, prioritize residential care; if you have a stable environment, explore telehealth or outpatient options immediately.
When Depression and Addiction Intertwine
The Bidirectional Relationship Explained
Understanding the connection between depression and substance use is essential for anyone considering depression rehab. The relationship is bidirectional, meaning each condition can both cause and worsen the other. For example, many individuals turn to alcohol or drugs as a way to cope with persistent sadness or hopelessness. Unfortunately, this self-medication often deepens depressive symptoms over time. On the other hand, regular substance use can disrupt the brain’s natural reward and mood systems, making depression more severe and harder to treat.
Research shows that shared brain pathways—especially those involving chemicals like dopamine and serotonin—help explain why these disorders so often overlap. When one system is affected, it can trigger or intensify the other, creating a challenging cycle to break.
This pattern is not just theoretical. Meta-analyses demonstrate a strong link between improvements in depressive symptoms and reductions in substance use, especially when both are treated together.1
This interplay highlights why depression rehab designed specifically for co-occurring disorders is so vital. Addressing one without the other often leads to setbacks or incomplete recovery. By understanding this cycle, individuals and families can better recognize what effective treatment requires. Next, we’ll look at how common this overlap is and what it means for long-term recovery.
Prevalence and Impact on Recovery
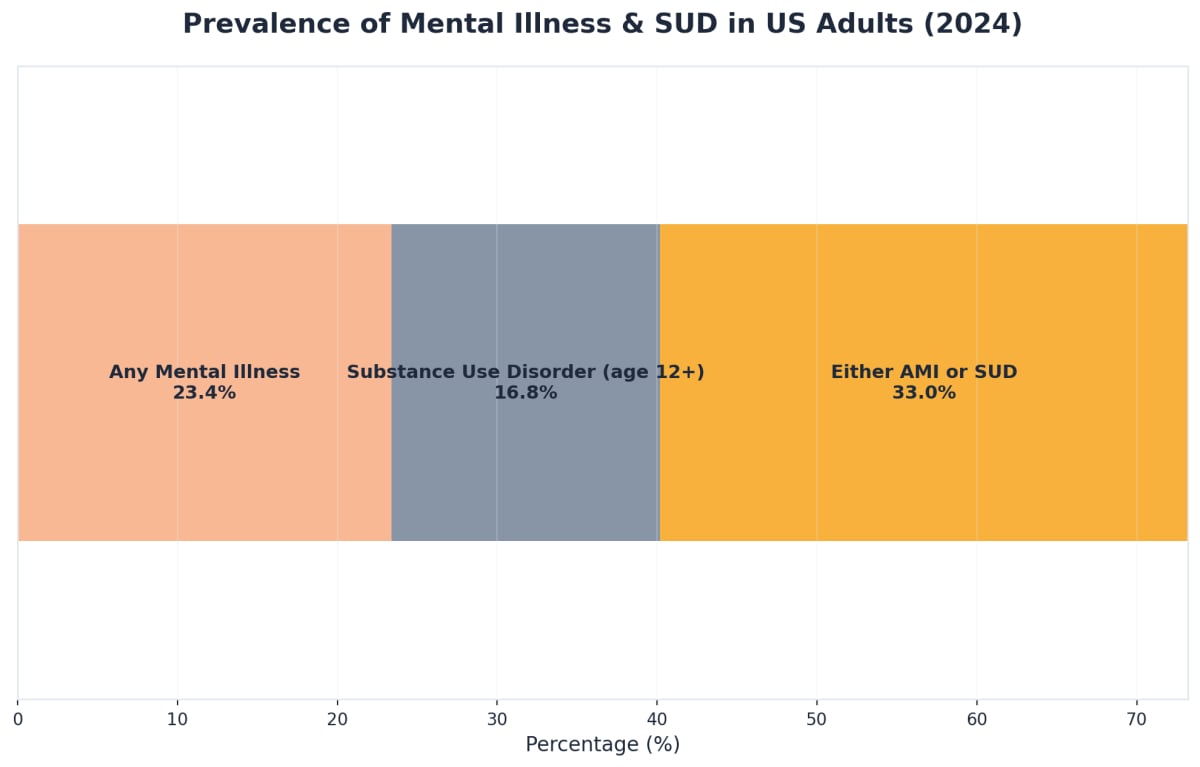
A clear understanding of just how common co-occurring depression and substance use is can help families and individuals see why specialized depression rehab is essential. Up to 56% of those with serious mental illness will experience a substance use disorder at some point in their lives, highlighting the frequency of this overlap. In 2024, roughly one in three adults in the United States had either a mental illness or substance use disorder in the past year, underscoring how widespread these challenges are.4,6
Despite the high numbers, access to appropriate depression rehab remains a significant barrier. Only 18% of addiction treatment programs and just 9% of mental health programs are truly equipped to provide care for both conditions at the same time. This means that even as more people seek help, many are forced to navigate fragmented systems or receive care for only one aspect of their health.7
This gap in integrated care can directly impact recovery outcomes. Research shows that treating both depression and substance use together—rather than separately—leads to better results, including greater symptom reduction and improved long-term recovery rates. Depression rehab designed with co-occurring disorders in mind offers a coordinated approach, increasing the likelihood of lasting change. Next, we’ll explore why integrated treatment approaches are key to changing outcomes for people facing both depression and substance use challenges.2
Why Integrated Depression Rehab Changes Outcomes
Sequential vs. Parallel vs. Integrated Care
When seeking help for co-occurring depression and substance use disorders, understanding the differences between sequential, parallel, and integrated care is crucial. Use this simple checklist to evaluate potential treatment approaches:
- Sequential: Are depression and substance use addressed separately, one after the other?
- Parallel: Are both treated at the same time but by different care teams?
- Integrated: Is there a single team providing coordinated care for both conditions together?
Sequential treatment means addressing one disorder before the other. While this approach might seem straightforward, it can leave important symptoms unaddressed for too long, increasing risk of relapse. Parallel care involves working with separate providers for each issue at the same time, but communication between teams may be limited. This can lead to mixed messages or inconsistent goals, which often slows progress.
| Treatment Model | Approach | Outcome Risk |
|---|---|---|
| Sequential | Treats one condition first, then the other. | High risk of relapse due to untreated symptoms. |
| Parallel | Treats both simultaneously but with separate teams. | Inconsistent goals due to lack of provider communication. |
| Integrated | Single team treats both conditions in one plan. | Highest success rate; prevents “falling through the cracks.” |
Integrated care stands apart by blending treatment for both depression and substance use into a single, unified plan. A coordinated team works together to address all symptoms at once, creating consistent goals. Research consistently shows that integrated care in depression rehab for co-occurring disorders results in better outcomes: individuals experience greater reductions in both substance use and depressive symptoms compared to those treated sequentially or in parallel.2
This approach works best when someone’s depression and substance use are closely linked, and when clear communication among providers is a priority. Next, we’ll review the research that proves why integrated care sets a higher standard for recovery.
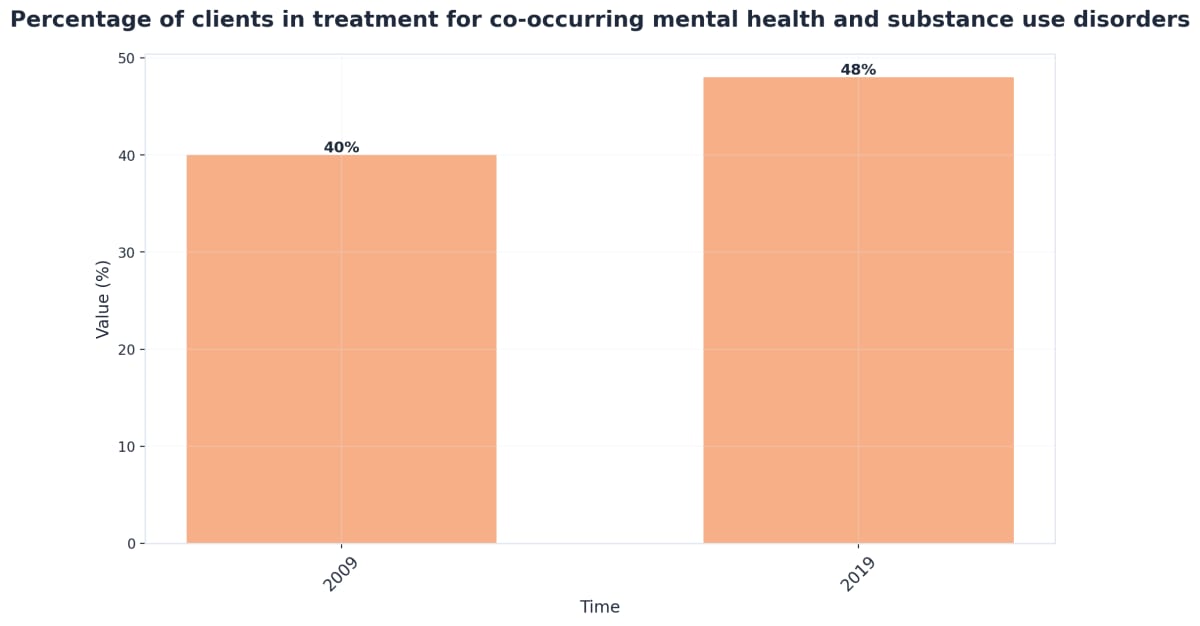
Evidence-Based Results from Research
The case for integrated care in depression rehab is built on consistent, high-quality research. Multiple studies confirm that treating depression and substance use together—rather than in isolation—leads to more substantial and lasting improvements. For example, individuals who receive integrated care experience greater reductions in both substance use and depressive symptoms, as well as improved daily functioning, when compared to those who undergo sequential or parallel treatment models. Meta-analyses also reveal a strong link between the improvement of depressive symptoms and reductions in substance use; the more depression lifts, the more likely substance use is to decline as well.1,2
Recent advancements have broadened access and effectiveness. Digital and telehealth-based programs for depression rehab now rival traditional in-person care, with some studies showing a 39% reduction in relapse odds when remote interventions supplement face-to-face services. For young people, telehealth solutions are especially promising, demonstrating comparable results to in-person treatment for depression and even greater improvements for anxiety disorders.3,9
Despite these positive developments, a significant gap exists between what research shows is effective and what most people can access. Only 18% of addiction programs and 9% of mental health programs are equipped to offer fully integrated, dual diagnosis treatment. This means that, while integrated depression rehab delivers the best outcomes, finding a program with true dual-focus remains a challenge for many. With the evidence pointing clearly toward integrated care, the next section explores which therapies, medications, and support systems make these programs successful.7
Core Components of Effective Depression Rehab Programs
Behavioral Therapies That Address Both
A successful depression rehab program for co-occurring disorders places behavioral therapies at its core. To help individuals and families evaluate treatment options, use this quick assessment:
- Does the program offer
CBT(Cognitive Behavioral Therapy) adapted for both depression and substance use? - Are therapists skilled in approaches like
DBT(Dialectical Behavior Therapy) or motivational interviewing? - Is the focus on practical coping skills that address both mood and substance challenges?
CBT is especially prominent in effective depression rehab settings. It helps people recognize how negative thinking patterns and learned behaviors can fuel both depression and substance use, then teaches practical strategies to break these cycles. In programs treating co-occurring disorders, CBT is often integrated with techniques tailored to substance use triggers, relapse prevention, and emotional regulation.10
Dialectical Behavior Therapy (DBT) is another widely used approach. Originally developed for intense emotional distress, DBT teaches mindfulness, distress tolerance, and interpersonal effectiveness—skills that are valuable for managing urges and depressive symptoms alike.
Motivational interviewing rounds out the toolkit for depression rehab by fostering internal motivation for change. By focusing on each individual’s reasons for recovery, this approach helps people move from ambivalence to action, building a foundation for long-term improvement. Integrated behavioral therapies work best when treatment teams coordinate care and adapt techniques for the unique patterns of each person’s depression and substance use. For those seeking a path to lasting recovery, prioritizing programs that blend these evidence-based therapies is essential. Next, we’ll look at how medications and family involvement can further enhance the effectiveness of integrated depression rehab.2
Medication and Family Involvement Roles
Successful depression rehab for co-occurring disorders is strengthened by two often-overlooked factors: thoughtfully chosen medications and active family involvement. Use this decision tool to discuss options with your care team:
- Has the team explained the pros and cons of different antidepressant classes, especially if substance use is present?
- Is medication integrated with therapy and regular monitoring for side effects or substance interactions?
- Are family members invited to participate in education sessions or therapy?
Pharmacological treatment is most effective when tailored to the unique needs of people facing both depression and substance use. While antidepressants can reduce depressive symptoms, research shows the impact on substance use varies. For example, certain non-SSRI antidepressants, such as tricyclics, may be more effective for those with alcohol dependence, while SSRIs may not offer the same benefit for individuals with drug dependence. Collaborative medication management—where prescribers, therapists, and clients regularly review progress—can help maximize benefits and minimize relapse risk.1
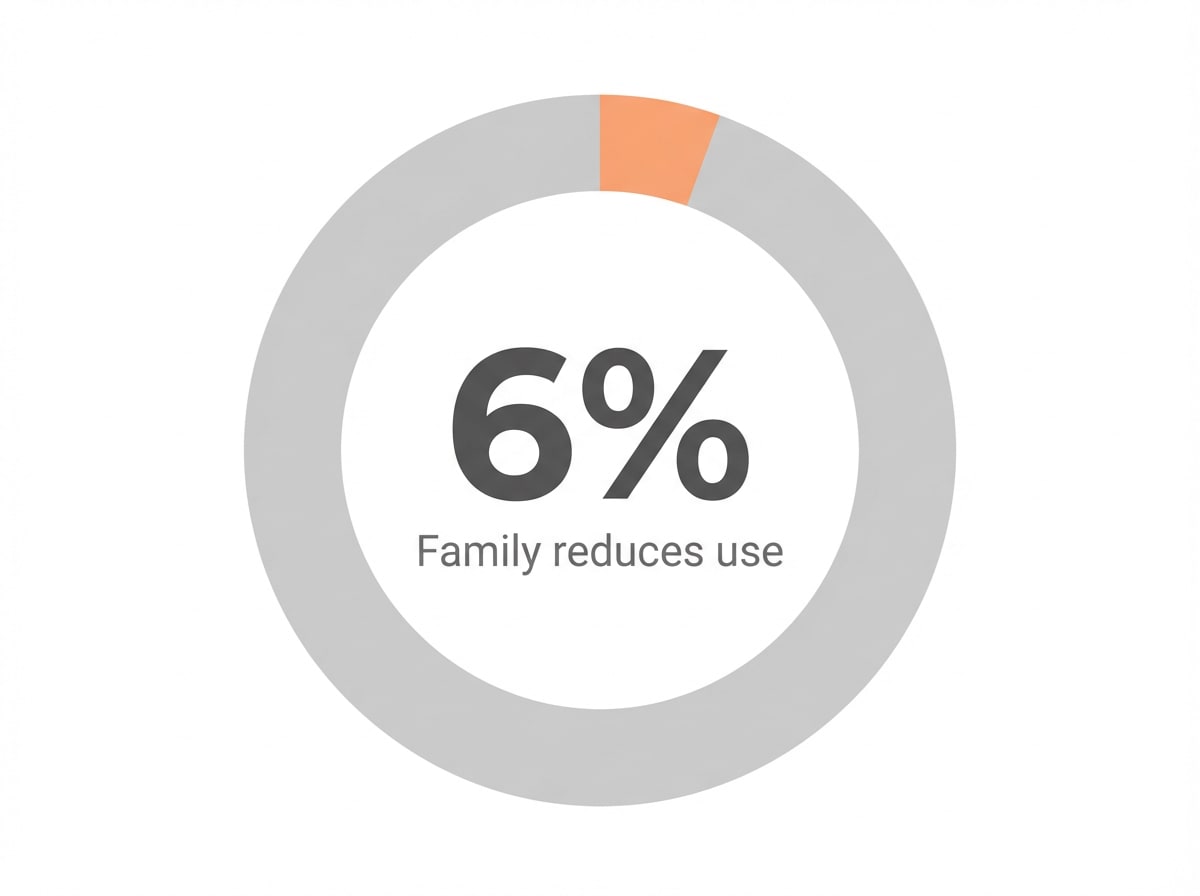
Family involvement is another powerful resource. Programs that include loved ones in the recovery process see measurable gains—studies report a 6% greater reduction in substance use when significant others participate, compared to individual therapy alone. Family members can learn about the signs of relapse, develop supportive communication skills, and help reinforce healthy routines. This support not only improves outcomes during depression rehab but can also provide a safety net after formal treatment ends. As you weigh options for depression rehab, consider how medication, therapy, and family support combine to create a truly integrated approach. Next, we’ll guide you through ways to choose the right path for your specific situation.8
Choosing the Right Path for Your Situation
Selecting between these two treatment approaches represents one of the most significant decisions in a recovery journey. The right choice depends on multiple interconnected factors that deserve careful consideration and honest assessment.
Three Critical Questions to Ask Yourself:
- Is my physical safety at risk during withdrawal or early recovery?
- Does my current environment support or undermine my recovery goals?
- What level of structure and accountability do I honestly need right now?
The severity of substance use plays a central role in determining the appropriate level of care. Individuals who have been using substances heavily for extended periods, or who have experienced dangerous withdrawal symptoms in the past, typically benefit from the medical supervision available in residential settings. The 24-hour monitoring provides a safety net during the vulnerable early stages of recovery when physical and psychological challenges are most intense.
Personal responsibilities and life circumstances also influence this decision significantly. Consider Maria, a single mother with strong family support—she found that outpatient treatment allowed her to maintain her parenting role while her sister helped with childcare during evening sessions. However, it’s worth considering whether attempting to juggle multiple responsibilities while beginning recovery could compromise the healing process. Sometimes, taking a temporary step back through residential care creates a stronger foundation for long-term stability. James, a marketing executive, initially resisted inpatient treatment due to work concerns, but ultimately found that his employer supported a medical leave, and the intensive 30-day program addressed underlying issues his previous outpatient attempts had missed.
The home environment deserves honest evaluation when weighing these options. A living situation filled with triggers, easy access to substances, or relationships that enable continued use makes outpatient treatment considerably more challenging. Conversely, a supportive home environment with people committed to recovery can strengthen outpatient treatment outcomes.
| Factor | Residential (Inpatient) | Outpatient |
|---|---|---|
| Structure | 24/7 monitoring and support. | Scheduled sessions; return home daily. |
| Cost Range | $5,000 – $30,000 (30 days) | $1,500 – $10,000 (3 months) |
| Best For | Severe symptoms, unsafe home environment. | Stable home life, strong support system. |
Previous treatment history provides valuable information for this decision. Someone who has completed outpatient programs multiple times without achieving lasting recovery may need the more intensive structure of residential care. Patterns of relapse often indicate that a higher level of support is necessary to address underlying issues effectively.
Mental health considerations cannot be overlooked when choosing the right treatment path. Co-occurring conditions like depression, anxiety, trauma, or other psychiatric concerns often require the integrated care available in residential settings. Attempting to address substance use without simultaneously treating mental health conditions frequently leads to incomplete recovery.
Financial considerations and insurance coverage naturally enter this equation as well. Many insurance plans cover both treatment types, though coverage levels vary—some plans cover 50-80% of costs after deductibles are met. Beyond insurance, many facilities offer payment plans, sliding-scale fees based on income, or can connect individuals with state-funded programs and grants. Treatment centers can provide detailed information about what specific plans cover and help identify the most feasible options within those parameters.
Ultimately, this decision should involve input from medical professionals, addiction specialists, and trusted family members. An honest assessment conducted during a professional evaluation can clarify which path offers the greatest likelihood of successful, sustained recovery. The goal isn’t simply to begin treatment—it’s to choose the approach that provides the best chance for transformation and healing.
Frequently Asked Questions
How do I know if a program truly offers depression rehab for co-occurring disorders versus treating conditions separately?
To determine if a program truly offers depression rehab for co-occurring disorders, look for a coordinated plan where both depression and substance use are addressed together by one integrated team. Ask whether therapists and medical staff have specific training in dual diagnosis and if treatment sessions regularly include discussions of both mental health and substance use topics. A red flag is when care is delivered in separate silos, with little communication between providers treating each condition. Only about 18% of addiction programs and 9% of mental health programs actually deliver this kind of integrated care, so it’s important to ask detailed questions before enrolling.7
Can telehealth or outpatient programs be as effective as residential treatment for depression rehab for co-occurring disorders?
Yes, telehealth and outpatient programs can be as effective as residential treatment for depression rehab when addressing co-occurring disorders, depending on individual circumstances. Recent studies show that telehealth-based depression rehab provides comparable results to in-person care for depression—and even greater improvements for anxiety in young people. Digital interventions also expand access and flexibility, making it easier for many to receive integrated care without leaving home. Outpatient options are a good fit for those with stable living environments and strong support systems. Residential treatment remains essential if safety or daily functioning is at risk, but many benefit from the accessibility and proven outcomes of telehealth and outpatient depression rehab.3,9
What should I expect during the first few weeks of depression rehab for co-occurring disorders?
During the first few weeks of depression rehab for co-occurring disorders, individuals can expect a thorough assessment from a team experienced in both mental health and substance use care. This initial phase includes setting collaborative goals, beginning evidence-based therapies like Cognitive Behavioral Therapy (CBT), and exploring any necessary medication options. Many programs also offer group support and introduce family involvement early, as research shows this can enhance progress. Adjusting to structured routines, open communication with care providers, and learning new coping skills are all part of the early experience. These foundational steps help set the stage for lasting recovery.8
How long does depression rehab for co-occurring disorders typically take to show meaningful improvement?
Most people begin to notice meaningful improvement from depression rehab for co-occurring disorders within four to eight weeks of starting integrated care. This timeframe reflects research showing that evidence-based therapies, when combined with medication and support, often lead to significant symptom relief in the first two months. However, timelines can vary based on individual needs, the severity of symptoms, and the level of support available. Some may experience steady progress early, while others require a longer period for changes to take hold. Regular communication with your care team and ongoing family involvement can help sustain momentum and address any challenges as they arise.2
Will my family be involved in my depression rehab for co-occurring disorders treatment plan?
Family involvement is often a key part of your depression rehab for co-occurring disorders treatment plan. Many programs invite loved ones to participate in education sessions, therapy discussions, or supportive activities. Research shows that when family members are included, there is a 6% greater reduction in substance use compared to individual therapy alone. Your care team may also help family members learn how to support your recovery, recognize warning signs, and build healthy communication patterns. This collaborative approach not only supports your progress during depression rehab but can provide important encouragement and accountability after formal treatment ends.8
What happens if depression rehab for co-occurring disorders includes medications I’ve tried before without success?
If depression rehab for co-occurring disorders includes medications you’ve tried before without success, there are still several hopeful options. Integrated treatment teams will often review why past medications may not have worked—factors like dose, duration, or interactions with substances can all play a role. Sometimes, switching to a different class of antidepressant, such as from an SSRI to a tricyclic, may offer better results, especially for those with alcohol dependence. Your care plan should be regularly adjusted based on your feedback and ongoing progress. Openly sharing your experiences helps the team personalize depression rehab and explore new strategies until meaningful improvement is achieved.1
How can I maintain progress after completing depression rehab for co-occurring disorders?
Maintaining progress after completing depression rehab for co-occurring disorders centers on staying engaged with aftercare, building a supportive network, and using the coping tools learned in treatment. Regular check-ins with your care team and attending follow-up appointments can help catch setbacks early. Many people benefit from ongoing therapy, support groups, or digital resources—telehealth and online programs have proven effective for continued care and relapse prevention. Including family or trusted friends in your support plan increases accountability and connection, both of which lower relapse risk. Staying proactive and reaching out for help when challenges arise will help you sustain the positive changes made in depression rehab.3,8
Conclusion
Navigating the path to recovery from substance use requires understanding the treatment options available. Each approach offers distinct advantages: flexibility and real-world application on one hand, intensive support and structure during vulnerable times on the other. Both have proven effective when matched appropriately to individual circumstances.
The decision about which treatment path to pursue shouldn’t be made lightly or alone. Healthcare professionals can assess the severity of substance use, evaluate co-occurring conditions, and consider personal circumstances to recommend the most appropriate level of care. Their expertise helps ensure individuals receive the support that aligns with their specific needs and situation.
Taking that first step toward healing requires tremendous courage—acknowledging the need for help and reaching out represents a profound act of self-compassion and strength. Whether someone is just beginning to explore treatment options or ready to commit to recovery, both paths lead toward the same destination: a healthier, more fulfilling life free from substance dependence. Recovery is possible, and choosing to seek help today can transform tomorrow. If you or someone you care about is struggling with substance use, reach out to a healthcare provider or call SAMHSA’s National Helpline at 1-800-662-4357 for free, confidential support and treatment referrals available 24/7.
References
- Treatment of Co-occurring Depression and Substance Dependence. PMC/NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC2722074/
- Integrating Treatment for Co-Occurring Mental Health Conditions. PMC/NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC6799972/
- Digital Integrated Interventions for Comorbid Depression and Substance Use Disorder. JMIR Mental Health. https://mental.jmir.org/2025/1/e67670/
- Integrated Treatment for Co-Occurring Disorders: Building Your Program. SAMHSA. https://library.samhsa.gov/sites/default/files/ebp-kit-building-your-program-10112019.pdf
- The Impact of Addiction Medications on Treatment Outcomes. PMC/NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC4866634/
- SAMHSA Releases Annual National Survey on Drug Use and Health. SAMHSA. https://www.samhsa.gov/newsroom/press-announcements/20250728/samhsa-releases-annual-national-survey-on-drug-use-and-health
- Dual Diagnosis Capability in Mental Health and Addiction Treatment. PMC/NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC3594447/
- Involving Family Members in Substance Use Disorder Treatment. Recovery Answers. https://www.recoveryanswers.org/research-post/involve-family-in-treatment-enhance-substance-use-disorder-outcomes/
- Artificial Intelligence-Driven Analysis of Telehealth Effectiveness in Youth. PMC/NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC11856424/
- What is Cognitive Behavioral Therapy? APA. https://www.apa.org/ptsd-guideline/patients-and-families/cognitive-behavioral
