Key Takeaways: Assessing Your Situation
Before diving into the details, use this quick assessment guide to understand where you or a loved one might stand regarding 7-OH use.
- Identify the Product: If the product is a gummy, vape, or highly concentrated liquid shot, it is likely a synthetic 7-OH product, not natural leaf kratom.
- Check Your Tolerance: If you find yourself needing double the dose you took last week to feel the same effect, physical dependence is likely forming.
- Immediate Action: If you experience shortness of breath or extreme sedation, seek medical help immediately. For long-term recovery, integrated therapy combined with medication-assisted treatment (MAT) shows the highest success rates.
What Makes 7-OH Different from Kratom
Understanding the mechanics of 7-OH addiction starts with recognizing that not all kratom products are created equal. While traditional kratom leaf has been used for centuries, modern 7-OH products are chemically distinct and carry significantly higher risks.
The Chemical Distinction That Matters
Quick Identification Tool:
- Natural Kratom: Greenish powder, bitter tea taste, leafy texture.
- 7-OH Product: Brightly colored gummies, sweet liquids, vape cartridges, pressed tablets.
The chemical distinction that matters lies in concentration and the way 7-OH is produced. Naturally, kratom leaves contain less than 2% 7-hydroxymitragynine (7-OH). In this minor amount, it acts as one of many compounds found in the plant. However, most products linked to 7-OH addiction today are not simply plant extracts.
They are semi-synthetic versions, created by chemically altering purified mitragynine (the main kratom alkaloid) into a concentrated form of 7-OH. This process results in a product that is not only much more potent but also behaves differently in the body than traditional kratom preparations.9
“These concentrated 7-OH products don’t resemble ground-leaf kratom or traditional teas—they are often disguised as candies, vapes, or capsules, amplifying the danger.” — FDA Warning7
This distinction is important because consumers may believe they are using a natural herbal product when, in fact, they are exposed to a substance with a significantly higher risk profile. You’re ready for the next level when you can clearly explain why the way 7-OH is made changes its effects and risks.
Potency Levels and Opioid Receptor Binding
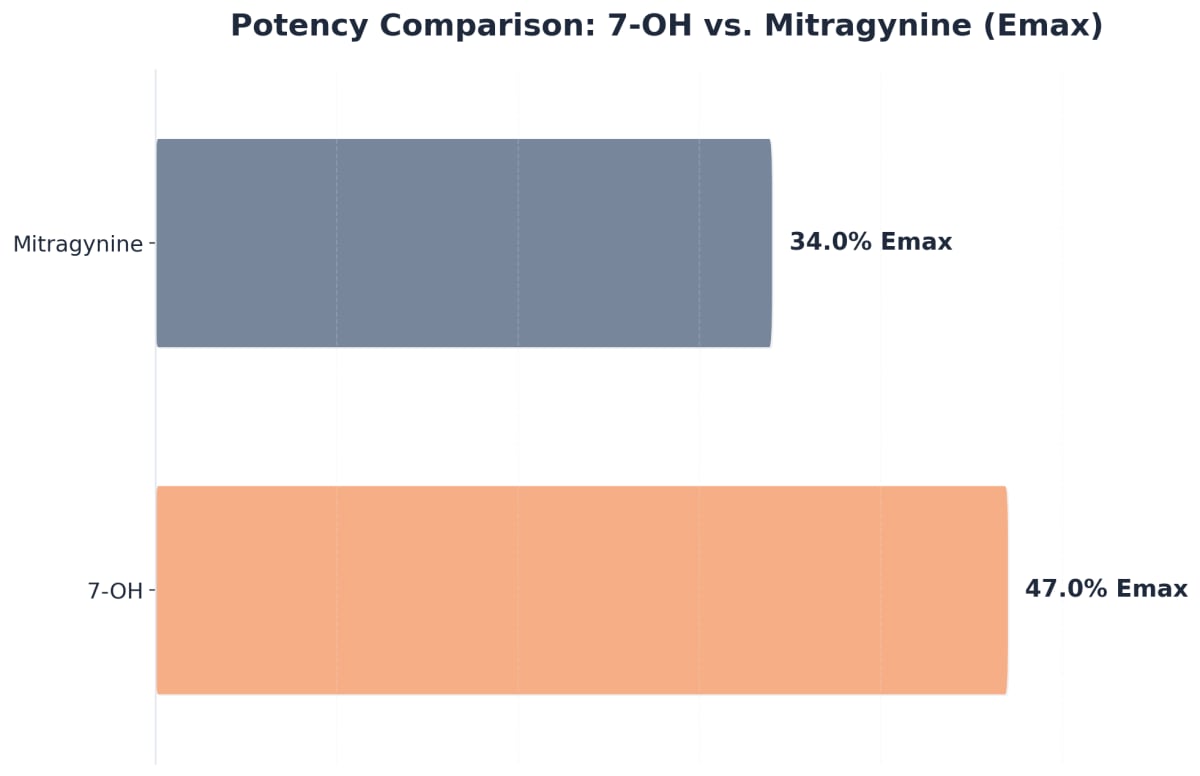
7-OH is dramatically more powerful than kratom’s main natural compound, mitragynine. Scientific studies show that 7-OH is about 22 times more potent as a mu-opioid receptor agonist than mitragynine, the primary alkaloid found in kratom leaves.1

| Feature | Natural Kratom Leaf | Concentrated 7-OH |
|---|---|---|
| 7-OH Content | Less than 2% | Highly Concentrated |
| Potency | Mild to Moderate | High (Opioid-like) |
| Addiction Risk | Lower | High (Rapid Onset) |
This means that even small amounts of 7-OH can trigger opioid-like effects that are much stronger than those produced by typical kratom products. In fact, 7-OH’s ability to bind to opioid receptors is so pronounced that its effects approach those of some prescription painkillers and even fentanyl. As a result, 7-OH addiction can develop faster and with more intense withdrawal symptoms than what is typically observed with natural kratom use.1
How 7-OH Addiction Develops and Progresses
From Casual Use to Physical Dependence
Self-Assessment Checklist: Are You Moving Toward Dependence?
- [ ] Do you need to take 7-OH just to feel “normal” in the morning?
- [ ] Have you increased your dose in the last 7 days?
- [ ] Do you feel irritable or anxious when you run out?
At first, many individuals try 7-OH because it is marketed as a legal or “herbal” product. The powerful opioid-like effects often surprise new users, since 7-OH is much more potent than natural kratom. With repeated use, the brain and body begin to adapt. Tolerance can build quickly—even within a few days—meaning a person needs more of the substance to get the same effects.3
This adaptation is a key marker in the development of 7-OH addiction, as the body starts to depend on the compound to function normally. Physical dependence can show up as cravings, irritability, or feeling unwell when not using 7-OH. According to experts, the transition from experimentation to dependence can happen rapidly due to the high potency and opioid receptor activity of 7-OH.1
Withdrawal Symptoms and Timeline
Withdrawal from 7-OH can be especially intense due to its potent action at the brain’s opioid receptors. When someone stops using 7-OH after developing dependence, symptoms may emerge within 6-24 hours. Common physical symptoms include:
- Muscle aches and bone pain
- Runny nose and excessive sweating
- Chills and temperature fluctuations
- Digestive upset (nausea, vomiting)
Emotional symptoms such as anxiety, irritability, and trouble sleeping are also frequently reported. People often describe a strong urge to use again just to feel normal, which is a hallmark of 7-OH addiction withdrawal. The acute withdrawal phase usually peaks around 2-4 days and can last up to a week, though some symptoms—especially sleep problems and mood changes—may linger longer.4
Health Risks and Overdose Dangers
Respiratory Depression and Fatal Outcomes
Emergency Warning Signs (Click to Expand)
If you or someone else exhibits bluish lips, extreme drowsiness, inability to wake up, or slow/shallow breathing, call emergency services immediately. These are signs of respiratory depression.
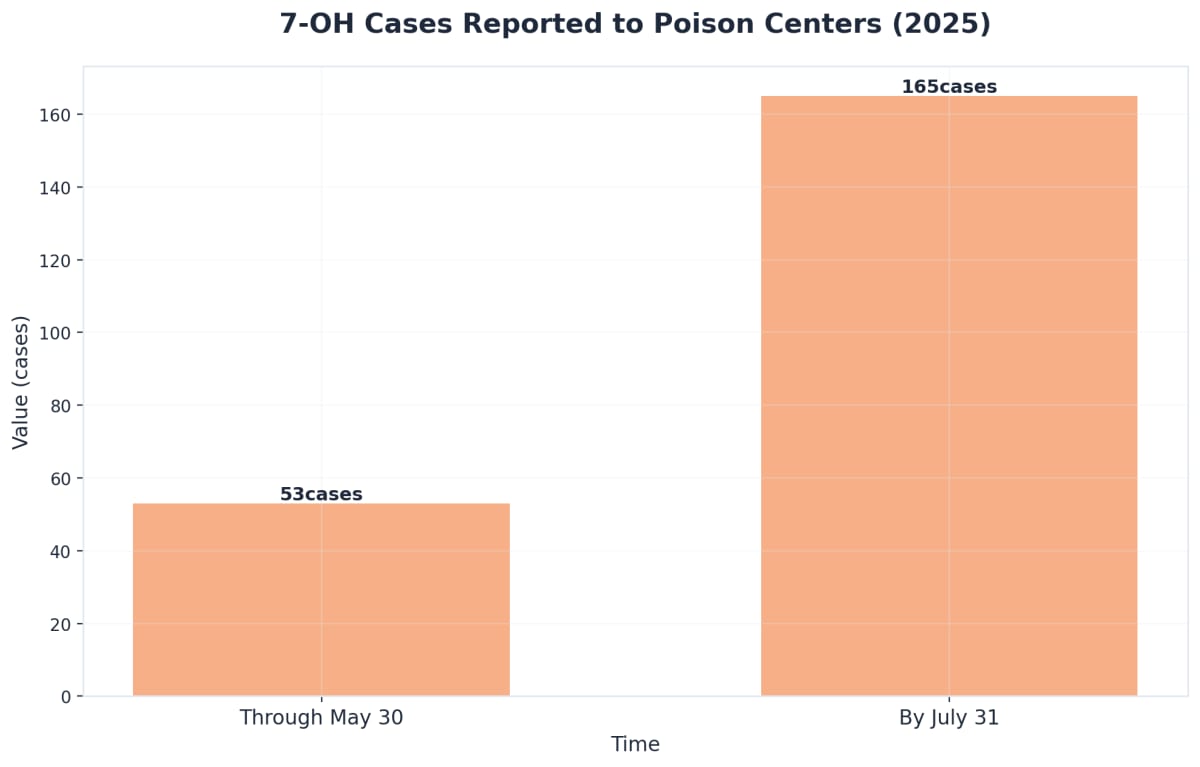
7-OH is much stronger than natural kratom, acting powerfully on the same brain receptors as prescription opioids and fentanyl. One of the most serious risks with 7-OH addiction is respiratory depression—a condition where breathing slows down or stops altogether. This happens because 7-OH powerfully activates the mu-opioid receptors in the brainstem, the area that controls automatic breathing.
Even moderate doses can dangerously suppress breathing, especially when 7-OH is used with other depressants like alcohol. Recent health alerts have documented multiple fatal overdoses in otherwise healthy young adults, with 7-OH identified as the main cause. In Los Angeles County, three deaths in people ages 18–40 were tied directly to 7-OH, and experts warn that accidental overdose can happen quickly due to unpredictable product strength.10
Polysubstance Use and Compounding Risks
Polysubstance use—taking 7-OH along with substances like alcohol, benzodiazepines, or prescription opioids—can multiply the dangers of each drug. When 7-OH is used together with other central nervous system depressants, the risk of life-threatening effects such as severe respiratory depression rises sharply.
According to public health data, 83% of kratom-involved overdose deaths in Washington State during 2024 involved more than one substance. Toxicology reports from several fatal cases show that alcohol and other sedatives, when present with 7-OH, often play a significant role in overdose outcomes. The effects can be especially unpredictable because each substance may intensify the impact of the others, leading to a much higher chance of accidental death for those struggling with 7-OH addiction.4,10
Evidence-Based Treatment for 7-OH Addiction
Medication-Assisted Treatment Protocols
Treatment Planning Guide:
- Initial Assessment: 1-2 hours (Medical history review)
- Induction Phase: 24-48 hours (Stabilizing on medication)
- Maintenance Phase: Ongoing (Months to years depending on need)
MAT for 7-OH addiction often centers around medications like buprenorphine, which binds to the same opioid receptors as 7-OH but in a safer, controlled way. This approach can significantly reduce withdrawal symptoms and cravings, making early recovery more manageable. Recent clinical case reports show that buprenorphine has been used successfully to stabilize individuals experiencing severe 7-OH withdrawal, even when symptoms were resistant to other treatments.14
While there are currently no FDA-approved medications specifically for 7-OH, experience from opioid use disorder treatment is informing best practices. Each MAT plan should be tailored to the individual’s needs, with careful monitoring to adjust dosages and address any side effects.
Integrated Therapy and Long-Term Recovery
Integrated therapy goes beyond medications by addressing the psychological, emotional, and social challenges of 7-OH addiction. Cognitive-behavioral therapy (CBT) is often used to help individuals understand triggers and build coping skills. Motivational interviewing and contingency management can increase motivation and reinforce healthy choices.
For those considering treatment options, costs and time investments vary:
| Treatment Type | Typical Time Commitment | Estimated Cost Range (Without Insurance) |
|---|---|---|
| Outpatient Therapy | 1-3 hours/week | $100 – $250 per session |
| Intensive Outpatient (IOP) | 9-15 hours/week | $3,000 – $10,000 per month |
| Residential Rehab | 30-90 days (24/7) | $15,000 – $60,000+ per month |
Research shows that combining these therapies leads to better outcomes than relying on medication alone. For those on the business application track—such as treatment centers—integrated care means coordinating medical, counseling, and social services for each individual.4
Frequently Asked Questions
How can I tell if a product contains 7-OH instead of natural kratom?
Spotting the difference between a product containing 7-OH and natural kratom can be challenging, as many 7-OH products are mislabeled or disguised. Natural kratom is typically found as a greenish powder or in traditional capsules made from ground leaves. In contrast, products containing concentrated 7-OH are often sold as vapes, gummies, candies, or brightly packaged capsules—formats not typical for natural kratom. If a product has no clear ingredient list, is marketed as extremely potent, or comes in forms appealing to youth, it may contain 7-OH rather than pure kratom leaf. Laboratory testing is the only way to be certain, as visual cues are not always reliable. The FDA warns that many 7-OH products are intentionally disguised and sold as “kratom” to mislead consumers, increasing the risk for 7-OH addiction.7
Will naloxone work to reverse a 7-OH addiction overdose?
Naloxone can reverse an overdose caused by 7-OH addiction, as 7-OH acts on the same mu-opioid receptors that naloxone targets. When given promptly, naloxone can restore breathing and help save lives during a 7-OH overdose. However, because 7-OH is very potent, higher or repeated doses of naloxone may be needed compared to standard opioid overdoses. Medical professionals recommend calling emergency services immediately, even after naloxone is given, since symptoms can return as naloxone wears off and 7-OH remains active in the body.4
Can someone with 7-OH addiction safely detox at home?
Detoxing from 7-OH addiction at home is not considered safe due to the severity and unpredictability of withdrawal symptoms. Because 7-OH is a highly potent opioid-like substance, withdrawal can bring on intense physical discomfort, severe anxiety, trouble sleeping, and strong cravings. In some cases, symptoms may escalate quickly, leading to dehydration, heart issues, or other complications that require urgent medical attention. Experts strongly recommend seeking care from medical professionals or a supervised treatment program to manage withdrawal safely and reduce the risk of relapse or medical emergencies.4
What should family members know about supporting someone through 7-OH addiction recovery?
Family members play a vital role in supporting someone through 7-OH addiction recovery. Encouragement, patience, and understanding can make a significant difference, as recovery is often challenging and progress may be uneven. It’s helpful to learn about 7-OH addiction, recognize that withdrawal and cravings are part of the process, and avoid judgment when setbacks happen. Attending support groups for families or seeking counseling can strengthen your ability to help. Experts recommend being involved in treatment planning, maintaining open communication, and offering consistent emotional support. Family involvement is linked to better outcomes in recovery from opioid-like substances such as 7-OH.4
How does 7-OH addiction affect people with co-occurring mental health conditions?
7-OH addiction can have a more severe impact on people with co-occurring mental health conditions such as depression, anxiety, or PTSD. The strong opioid-like effects of 7-OH may temporarily mask emotional distress, but over time, substance use can worsen symptoms and make mental health harder to manage. Withdrawal from 7-OH can also trigger or intensify anxiety, mood swings, and sleep problems, complicating recovery for those already struggling with mental health concerns. Experts recommend integrated treatment that addresses both 7-OH addiction and mental health needs together to improve long-term outcomes 4.
Are there outpatient treatment options available for 7-OH addiction?
Yes, outpatient treatment options are available for individuals struggling with 7-OH addiction. Outpatient programs offer structured care while allowing people to live at home, attend work or school, and maintain family responsibilities. These programs often include counseling, medication-assisted treatment, and peer support, all tailored to address the unique challenges of 7-OH addiction. Clinical reports show that medications like buprenorphine, combined with therapy, can help reduce cravings and support recovery in an outpatient setting. For many, outpatient care provides flexibility and ongoing support, which can be crucial for building long-term recovery from 7-OH addiction.4
What makes 7-OH addiction particularly dangerous for young adults?
7-OH addiction is particularly dangerous for young adults because these products are often marketed in brightly colored packaging and forms like gummies or vapes, making them especially appealing to youth . The concentrated potency of 7-OH far exceeds that of traditional kratom, putting young people at greater risk for rapid physical dependence, severe withdrawal, and accidental overdose—even with small amounts. Recent health alerts have documented overdose deaths in otherwise healthy individuals aged 18–40, emphasizing the unpredictable and life-threatening nature of 7-OH addiction in this age group.10
Conclusion
Recovery from substance use disorders represents a deeply personal journey that looks different for everyone. Throughout this exploration of substance use treatment, we’ve examined the various pathways available—from inpatient residential programs that provide intensive 24/7 care, to outpatient options that allow individuals to maintain daily responsibilities while receiving treatment, to medication-assisted treatment that combines FDA-approved medications with counseling and behavioral therapies.
Each approach offers distinct advantages, and the most effective recovery plans often incorporate multiple levels of care tailored to individual circumstances. Inpatient treatment provides structured environments ideal for those needing medical supervision during detoxification or those with co-occurring mental health conditions. Outpatient programs offer flexibility for those with strong support systems at home. Medication-assisted treatment has proven particularly effective for opioid and alcohol use disorders, addressing both the physical and psychological aspects of addiction. Many find that combining these approaches—along with peer support groups and ongoing therapy—creates the comprehensive foundation needed for lasting recovery.
No one has to face this challenge alone. Professional treatment providers, support groups, and caring communities stand ready to offer guidance, encouragement, and evidence-based care. Taking that first step—whether it’s making a phone call, attending a meeting, or simply asking for help—requires tremendous courage. That courage, combined with the right support and resources, can open the door to lasting recovery and a healthier, more fulfilling life ahead.
Contact rippleranch.com today to learn how our evidence-based treatment approaches can help you reclaim your health, restore your relationships, and build the fulfilling life you deserve.
References
- Kratom Byproducts: 7-OH and MP – MATTERS Network. https://mattersnetwork.org/kratom-byproducts-7-oh-and-mp/
- FDA Takes Steps to Restrict 7-OH Opioid Products Threatening American Consumers. https://www.fda.gov/news-events/press-announcements/fda-takes-steps-restrict-7-oh-opioid-products-threatening-american-consumers
- What to Know About 7-OH, the New Vape Shop Hazard – JAMA. https://www.jama.com/articles/10.1001/jama.2025.13592
- Kratom & 7-OH: What do we know about use, safety, and overdose – University of Washington. https://adai.uw.edu/wordpress/wp-content/uploads/dlm_uploads/Kratom-202404.pdf
- 7-Hydroxymitragynine Is an Active Metabolite of Mitragynine and a Partial Agonist of the Human μ-Opioid Receptor. https://pmc.ncbi.nlm.nih.gov/articles/PMC6598159/
- Operation Vape Trail Cracks Down on Illegal Substances in Vape Shops – DEA. https://www.dea.gov/press-releases/2025/09/22/operation-vape-trail-cracks-down-illegal-substances-vape-shops
- FDA and Kratom – Official FDA Page. https://www.fda.gov/news-events/public-health-focus/fda-and-kratom
- Health Advisory: Serious Illnesses Associated with 7-OH Use – America’s Poison Centers. https://poisoncenters.org/news-alerts/13531044
- From kratom to 7-hydroxymitragynine: evolution of a natural remedy into a public health threat. https://pmc.ncbi.nlm.nih.gov/articles/PMC12671409/
- Multiple Fatal Overdoses Tied to Synthetic Kratom Compound – Los Angeles County Department of Public Health. https://public.health.lacounty.gov/phcommon/public/media/mediapubhpdetail.cfm?prid=5139
